Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amy Stanway, Dermatology Registrar, Waikato Hospital, Hamilton, New Zealand, 2001. Reviewed and updated by Dr Amanda Oakley Dermatologist, Hamilton, New Zealand; Vanessa Ngan, Staff Writer, June 2014. Further updated by Dr Jannet Gomez, Postgraduate Student in Clinical Dermatology, Queen Mary University, London, United Kingdom, February 2016.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Treatment
Outlook
Erysipelas is a superficial form of cellulitis, a potentially serious bacterial infection affecting the skin.
Erysipelas affects the upper dermis and extends into the superficial cutaneous lymphatics. It is also known as St Anthony's fire due to the intense rash associated with it.
[GALLERY 5229: erysipelas1.jpg OR erysipelas1.jpg OR erysipelas4.jpg]
Erysipelas most often affects infants and older people but can affect any age group. Risk factors are similar to those for other forms of cellulitis. They may include:
Unlike cellulitis, almost all erysipelas is caused by Group A beta-haemolytic streptococci (Streptococcus pyogenes). Staphylococcus aureus, including methicillin-resistant strains (MRSA), Streptococcus pneumoniae, Klebsiella pneumoniae, Yersinia enterocolitica, and Haemophilus influenzae have also been found rarely to cause erysipelas.
Symptoms and signs of erysipelas are usually abrupt in onset and often accompanied by fevers, chills and shivering.
Erysipelas predominantly affects the skin of the lower limbs, but when it involves the face, it can have a characteristic butterfly distribution on the cheeks and across the bridge of the nose.

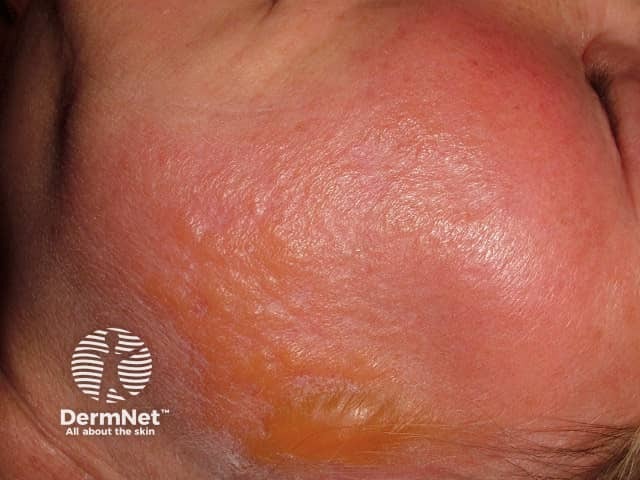
Erysipelas

Erysipelas recurs in up to one-third of patients due to:
Complications are rare but can include:
Erysipelas is usually diagnosed by the characteristic rash. The differential of erysipelas is similar to the cellulitis mimics. There is often a history of a relevant injury. Tests may reveal:
MRI and CT are undertaken in case of deep infection.
For the skin biopsy findings, see erysipelas pathology.
While signs of general illness resolve within a day or two, the skin changes may take some weeks to resolve completely. No scarring occurs.
Long term preventive treatment with penicillin is often required for recurrent attacks of erysipelas.
Erysipelas recurs in up to one-third of patients due to the persistence of risk factors and also because erysipelas itself can cause lymphatic damage (hence impaired drainage of toxins) in involved skin which predisposes to further attacks.
If patients have recurrent attacks, long term preventive treatment with penicillin may be considered.