Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: August, 2025
Authors: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand (1997); updated by Dr Rianet Post, Dermatologist, Stafford, United Kingdom (2016); minor update by Dr James Séamus Fuller, Dermatology Research Fellow, Skin Health Institute, Melbourne, Australia (2025)
Peer reviewed by: Dr Jonathan Haddad, Great Western Hospital, United Kingdom (2025)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department.
Introduction
Demographics
Causes
Clinical features
Differential diagnoses
Complications
Diagnosis
Treatment
Outcome
Allergic contact dermatitis is a form of dermatitis caused by an allergic reaction to a material (called an allergen) in contact with the skin. The allergen is harmless to people who are not allergic to it.
Allergic contact dermatitis is also known as contact allergy.

Acute weeping exudative allergic contact dermatitis due to a hair dye used on the beard

Chronic lichenified allergic contact dermatitis due to leather in a sandal (ACD-patient1)

Allergic contact dermatitis due to a rubber accelerator (used in the rubber curing process)
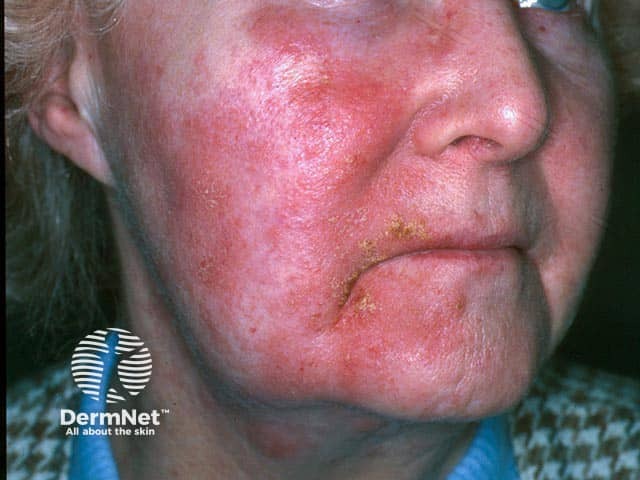
Acute allergic contact dermatitis due to lavender oil used on the pillow case to promote sleep
Allergic contact dermatitis is common in the general population and specific employment groups.
Allergic contact dermatitis is a type IV (delayed) hypersensitivity reaction, which typically occurs 24–72 hours after exposure to an allergen. The mechanism involves CD4+ T-lymphocytes, which recognise an antigen (from an allergen) on the skin surface and release cytokines that activate the immune system and cause dermatitis.
Only a small number of people react to the specific allergen, which is harmless to those who are not allergic to it. This is because the person has become sensitised to the allergen, meaning it will trigger an immune response.
Factors that increase the likelihood of sensitisation include:
Note:
Allergic contact dermatitis usually appears 24-72 hours after contact with the allergen. It usually resolves over several days, provided the skin is no longer in contact with the allergen.
The typical appearance is often a well-demarcated pruritic eczematous eruption, which may be acute (blistering, weeping, and/or oedematous) or chronic (lichenified or scaly plaques).
Allergic contact dermatitis is generally well demarcated and localised to the site of contact with the allergen, but it may extend outside the contact area or become generalised.
Transmission of the allergen from the site of contact, for example via the fingers, can lead to contact dermatitis on other areas of the skin, including the eyelids and genitals.
Dermatitis is unlikely to be due to a specific allergen if the area of skin most in contact with that allergen is unaffected.
Common allergens that trigger contact dermatitis reactions include:
There is a very long list of materials that have caused contact allergy in a small number of individuals.
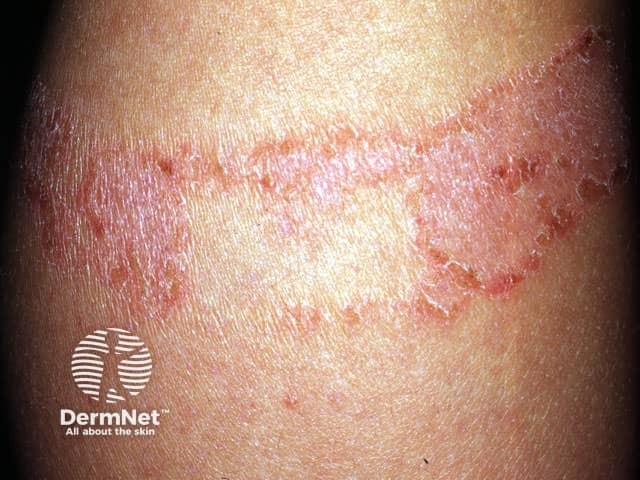
Adhesive plaster reaction
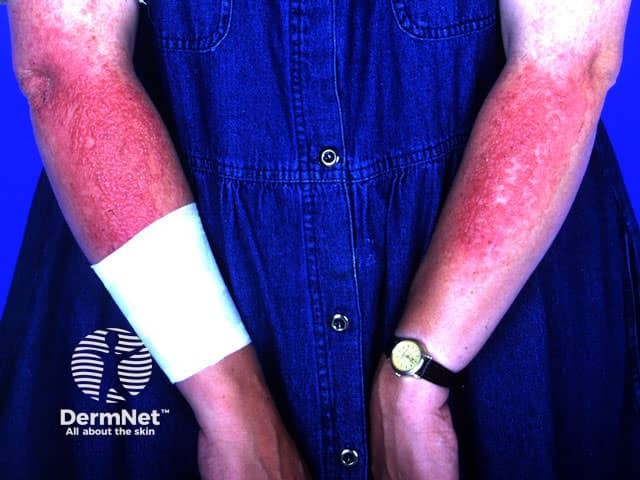
Sunscreen reaction
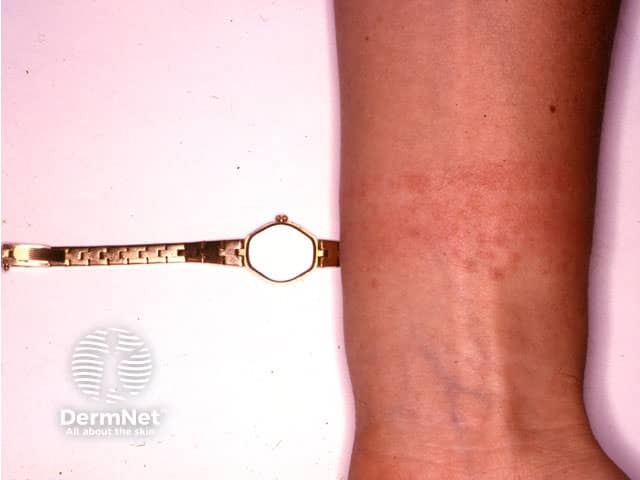
Watch strap reaction

Allergic contact dermatitis due to an adhesive in orthopaedic strapping
See more images of allergic contact dermatitis
Specific allergic contact dermatitis images.
Sometimes, contact allergy arises only after the skin has been exposed to ultraviolet light. The rash is confined to sun-exposed areas even though the allergen may have been in contact with covered areas. This is called photoallergic contact dermatitis.
Examples of photoallergy include:
Allergic contact dermatitis in patients with skin of colour more frequently presents with leathery, dark (hyperpigmented) patches. This is in contrast to the dry, cracked, erythematous skin typically seen in patients with fairer Fitzpatrick skin types.
In patients with darker skin, positive patch tests:
Post-inflammatory pigmentary changes, including both hypo- and hyperpigmentation, are more common in people with darker Fitzpatrick skin types, which can lead to significant psychological distress.
Allergic contact dermatitis typically starts as a localised reaction to an allergen in contact with the skin, but severe reactions may generalise due to autoeczematisation and can lead to erythroderma.
Ingestion of a contact allergen may rarely lead to symmetrical drug-related intertriginous and flexural exanthema or systemic contact dermatitis.
Allergic contact dermatitis is often a clinical diagnosis, without the need for specific testing. It is essential to take a detailed history that includes occupation, hobbies, products used at home and at work, sun exposure,allergens in use by consorts, and comorbidities. The morphology and location of the dermatitis are often the best indicators of the offending agent.
Patch testing is the gold standard in diagnosing allergic contact dermatitis and should be performed when contact allergy is suspected in patients with recurrent or chronic symptoms. Patch testing can establish the allergen(s) causing the rash to avoid future exposure.
Patients can also perform open application tests. This is done by applying the suspected product to a small area of sensitive skin (eg, inner aspect of upper arm) multiple times daily over several days, and then observing for a reaction. It can be done after patch testing to determine whether positive patch results lead to clinically significant reactions to products.
Other tests include:

A positive patch test to a piece of a suspect rubber glove 48 hrs after application on the skin
Identification and avoidance of offending allergens and potential cross-reacting agents is the principal management strategy.
Active dermatitis is usually treated with the following:
Sensitisation is usually life long. The prognosis is usually good and depends on patient education, adherence to allergen avoidance, and the treatment of active dermatitis.
The rash usually resolves if the allergen is avoided, but in some cases can persist indefinitely eg, chromate allergy. Furthermore, allergic contact dermatitis can recur even with minimal exposure to the allergen. Some allergens are difficult to avoid, with airborne allergens being particularly problematic eg, pollens and resins.
The longer a person suffers from severe allergic contact dermatitis, the longer it will take to clear after the diagnosis and cause are confirmed.