Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Susan Simpkin, Medical Registrar, Waikato Hospital, Hamilton, New Zealand, 2010. Updated by Hon Assoc Prof Amanda Oakley, Dermatologist, Waikato Hospital, Hamilton, New Zealand, November 2016.
Introduction
Smoking and skin damage
Smoking and ageing skin
Smoking and wound healing
Smoking and infections
Smoking and skin cancer
Smoking and palmoplantar pustulosis
Smoking and psoriasis
Smoking and hidradenitis suppurativa
Smoking and vascular disease
Smoking and cutaneous lupus erythematosus
Smoking and oral diseases
Effect of smoking on medicines
Smoking and skin conditions severity
Help to quit smoking
Cutaneous effects of smoking cessation
Skin and hair are exposed to various environmental noxious agents, including tobacco smoke. Tobacco smoke consists of thousands of substances that damage the skin, and nicotine itself is harmful.
Beyond its known links to cancer, lung and heart disease, smoking is associated with premature skin ageing, delayed wound healing, and increased infections, as well as a number of skin disorders, particularly psoriasis, hidradenitis suppurativa and cutaneous lupus erythematosus. There is a general observation that smokers tend to be more severely affected than non-smokers by the majority of inflammatory skin diseases — even acne —and various conditions are often more difficult to treat effectively in smokers.

Cigarette butts
Cigarette butts
Tobacco smoke causes oxidative stress so that insufficient oxygen is supplied to the skin resulting in tissue ischaemia and blood vessel occlusion. It reduces innate and host immune responses, and induces metallo-proteinase MMP-1, an enzyme that specifically degrades collagen.
Nicotine replacement is safer for the skin than smoking, although nicotine itself induces vasoconstriction, inhibits inflammation, delays wound healing and accelerates skin ageing.
Tobacco smoking has unpleasant temporary cutaneous and mucosal effects:
Longer term, the gaunt skin of a 40-year-old heavy smoker resembles that of non-smoking 70-year-old:
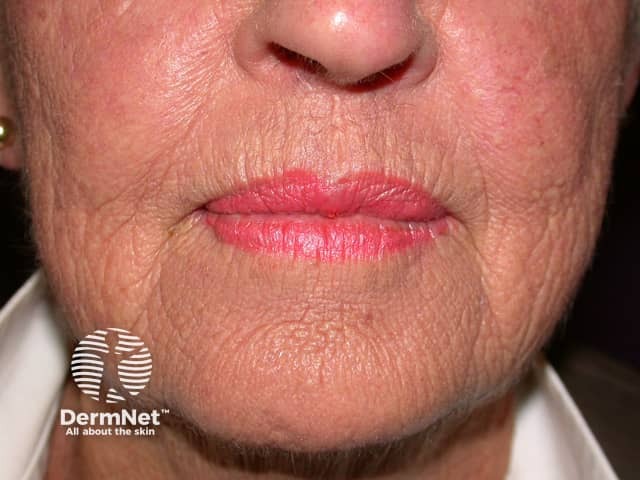
Smoking and its effects on the skin
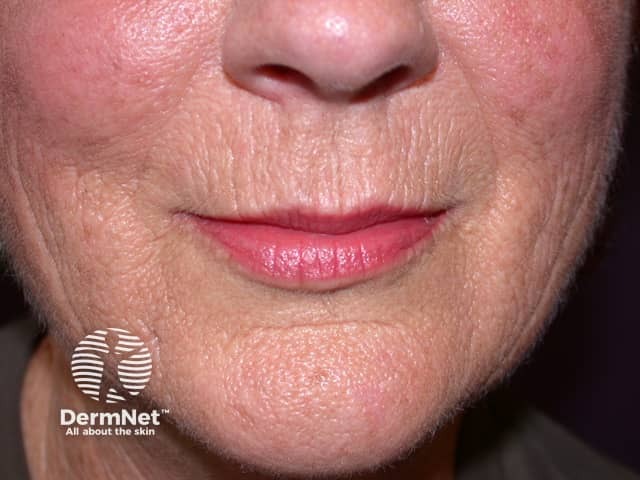
Smoking and its effects on the skin
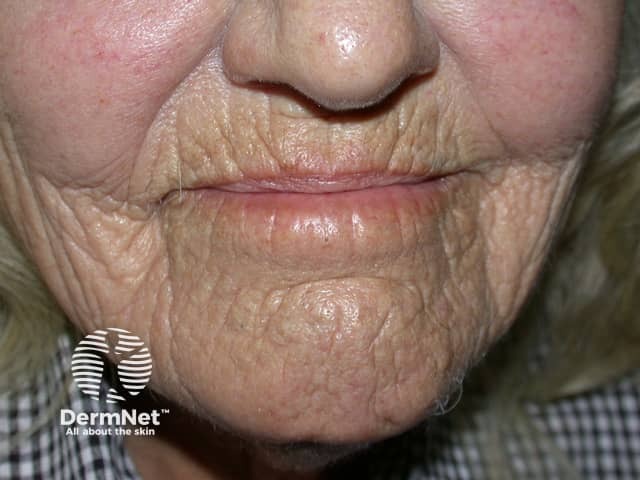
Smoking and its effects on the skin
It is not certain exactly how smoking causes early ageing of the facial skin. Theories include:
Smoking delays wound healing, including skin injuries and surgical wounds. It increases the risk of wound infection, graft or flap failure, death of tissue and blood clot formation. The reasons for this are unclear but involve:
Smoking contributes to the development and persistence of leg ulcers, particularly arterial ulcers, diabetic foot ulcers and calciphylaxis.
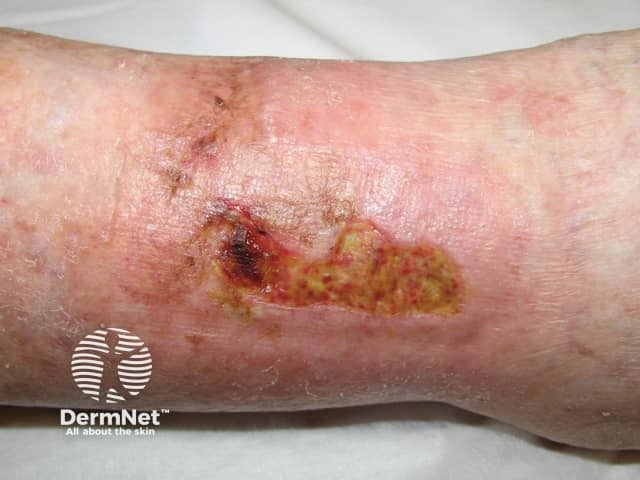
Venous ulcer
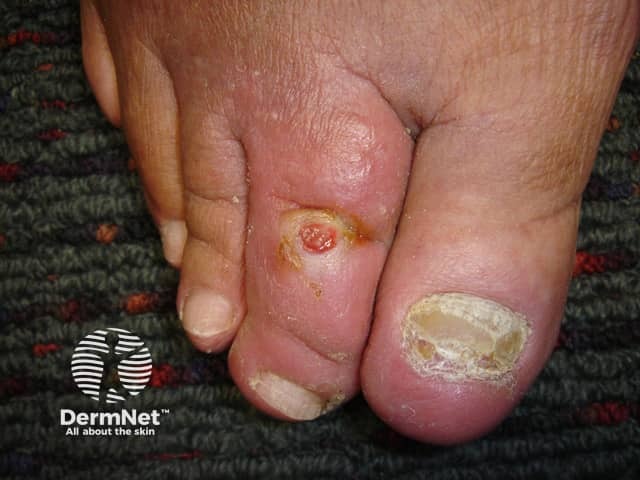
Diabetic foot ulcer
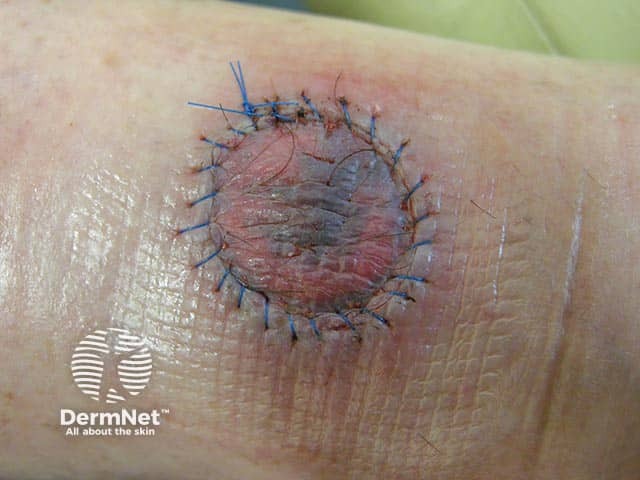
Failing skin graft
Smoking is associated with a greater likelihood or severity of:
If you have genital warts and you smoke, you have a greater chance of developing wart-virus associated cancers, including cervical cancer, vulval intraepitheial cancer, vulval cancer or penile intraepithelial cancer.
Smoking cigarettes doubles the risk of developing a type of skin cancer called squamous cell carcinoma, compared to non-smokers. There is also an increased risk of oral leukoplakia (precancer) and oral cancer; 75% of cases of oral cancer and lip cancer occur in smokers. Smoking does not appear to increase the risk of basal cell carcinoma.
Smoking cessation reduces the risk of metastasis (spread) from lip cancer by 2–3-fold.
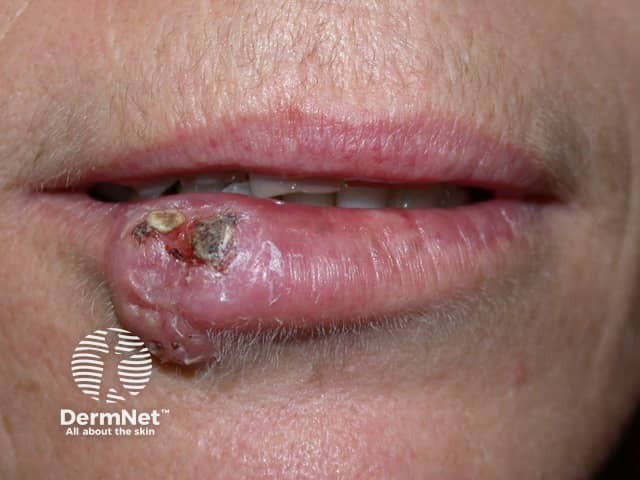
Lip cancer (squamous cell carcinoma)
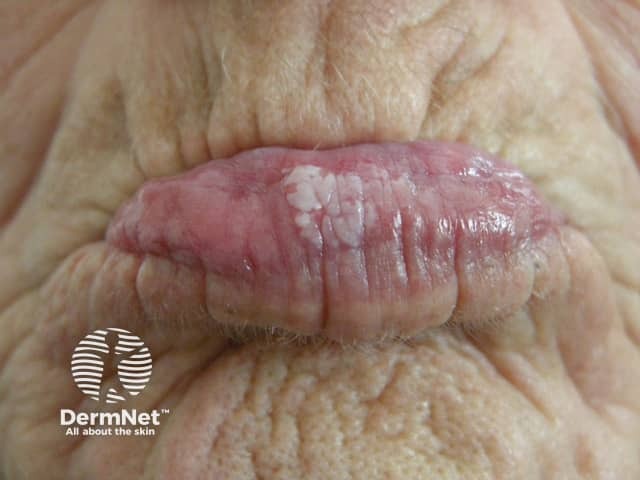
Oral leukoplakia
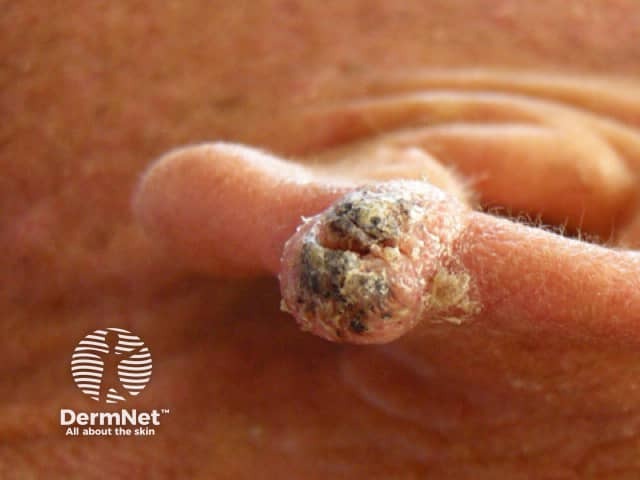
Ear cancer (squamous cell carcinoma)
Palmoplantar pustulosis is treatment-resistant, chronic, and disabling dermatosis characterised by pustules, erythema and scaling on the soles and palms. It mainly affects middle-aged women, >90% of whom smoke. The mechanism relates to nicotine binding with acetylcholine receptors in the sweat gland and duct, to change their structure and induce inflammation.
Cessation of smoking gradually results in improvement and the pustules may eventually clear up in many patients.
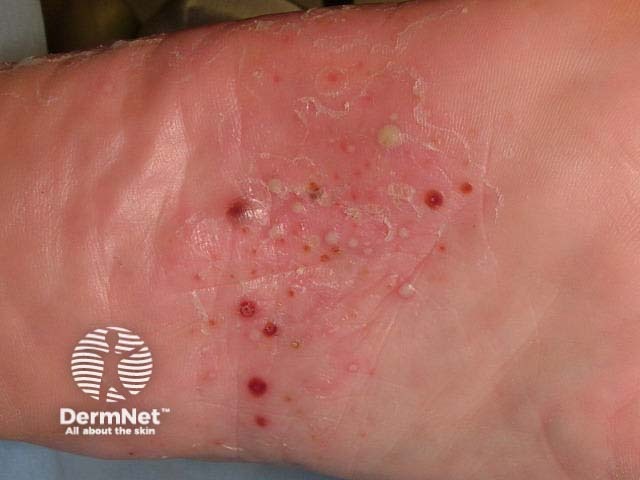
Plantar pustulosis
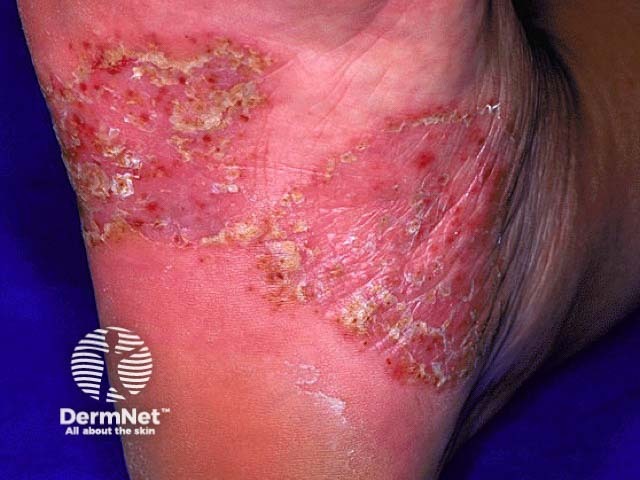
Plantar pustulosis
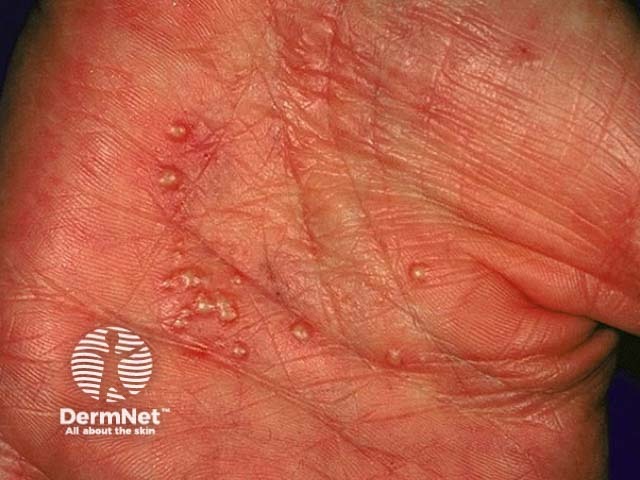
Palmar pustulosis
Several studies have confirmed that smokers tend to have more extensive and severe psoriasis than those that do not. Patients with chronic plaque psoriasis smoke more than patients without psoriasis. The research is confounded by those with obesity or metabolic syndrome and quality of life issues.
The mechanism appears to be that smoking induces inflammatory mediators and promotes keratinocyte proliferation. Nicotine itself binds to dendritic cells, T-cells and keratinocytes.
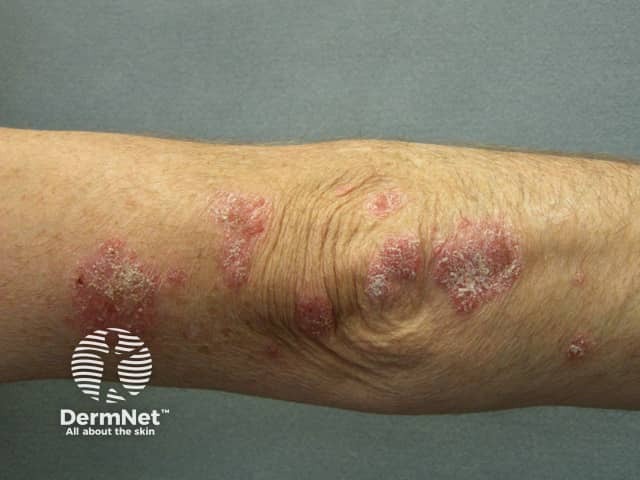
Smoking and psoriasis
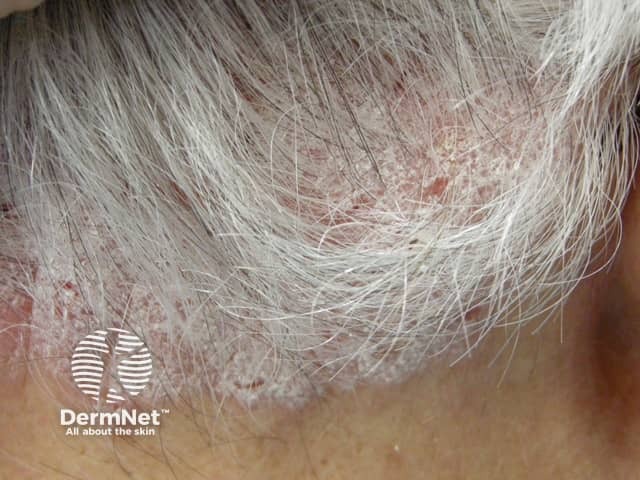
Smoking and psoriasis
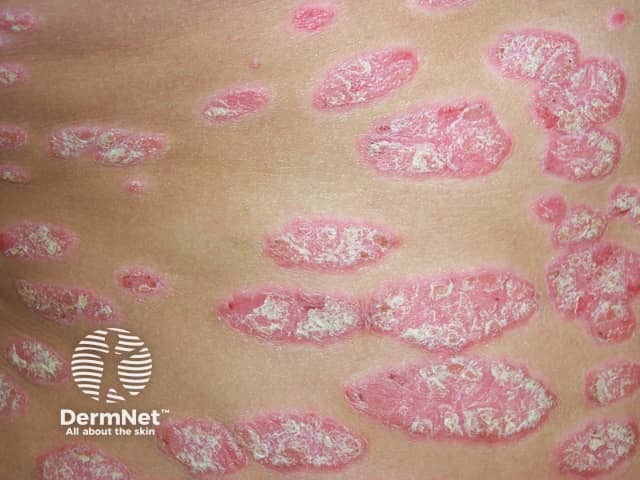
Plaque psoriasis
The majority of patients with hidradenitis suppurativa (HS) are smokers, and smokers have a greater burden of disease than non-smokers. There is genetic predisposition to HS, and it is particularly prevalent in obese women. The pathogenesis involves nicotine/acetylcholine-induced follicular occlusion, follicular rupture, and immune dysregulation. Smokers respond poorly to current treatment options.
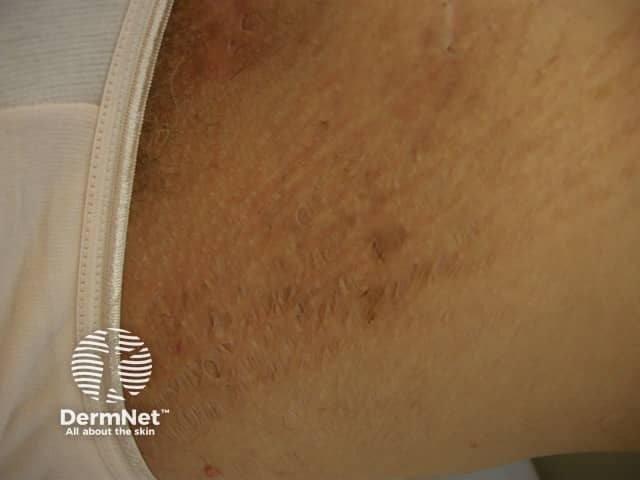
Smoking and hidradenitis suppurativa
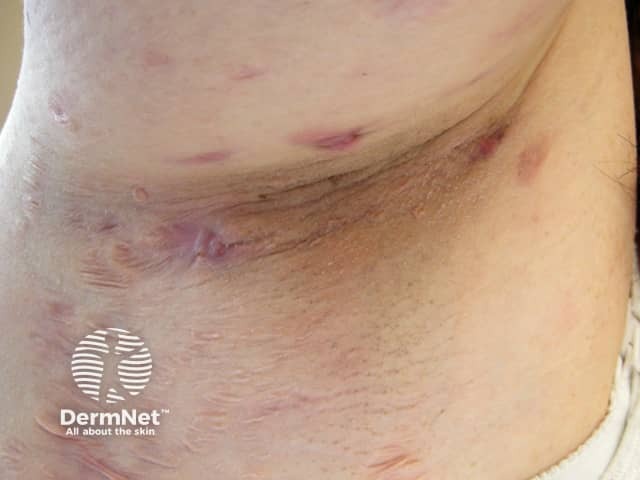
Smoking and hidradenitis suppurativa
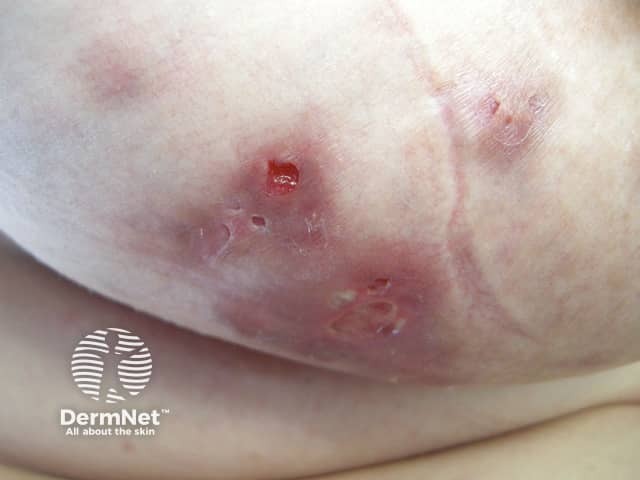
Smoking and hidradenitis suppurativa
Nicotine causes vasoconstriction and hypercoagulability, increasing the chance of blood clots occluding blood vessels.
Smoking can aggravate or initiate:
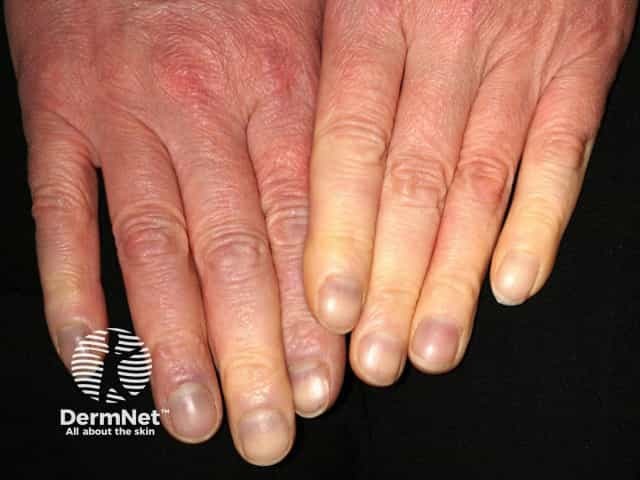
Raynaud phenomenon
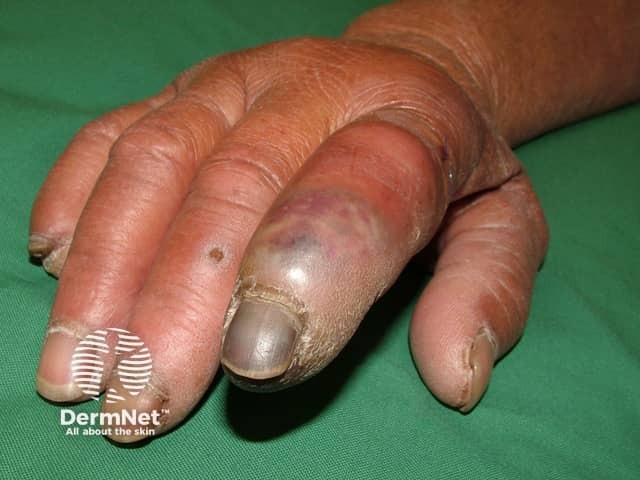
Antiphospholipid syndrome
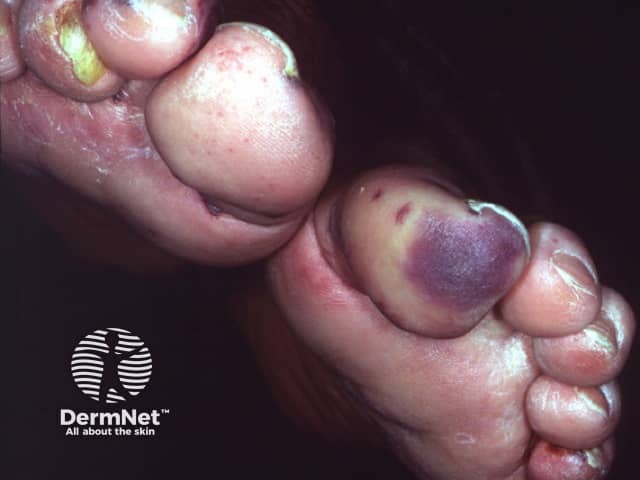
Cholesterol emboli
There is more than ten-fold risk of chronic cutaneous lupus erythematosus (especially discoid lupus erythematosus) in smokers compared to non-smokers. Smoking increases autoimmune activity by activating the lymphocytes. There is also suspicion that treatment of chronic cutaneous LE is less effective in smokers.
Treatment of cutaneous lupus erythematosus with hydroxychloroquine and other medications is less effective in smokers.
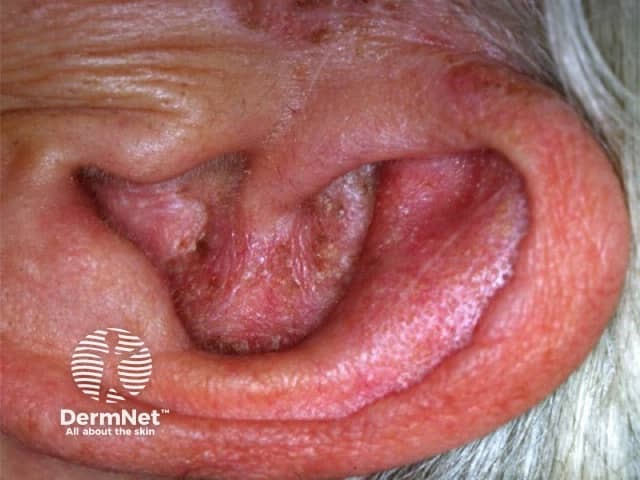
Smoking and discoid lupus erythematosus
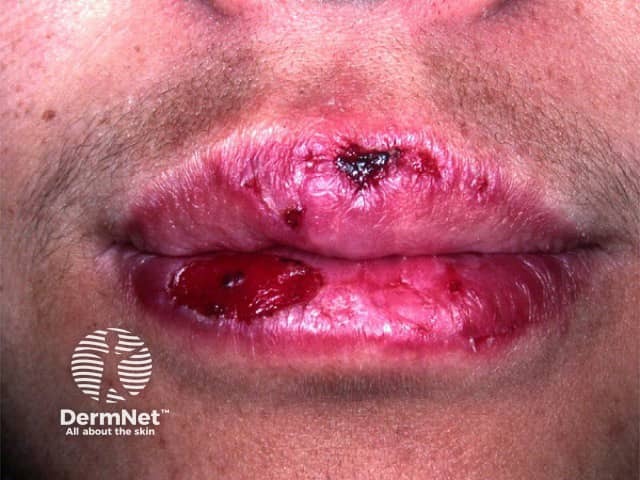
Smoking and discoid lupus erythematosus
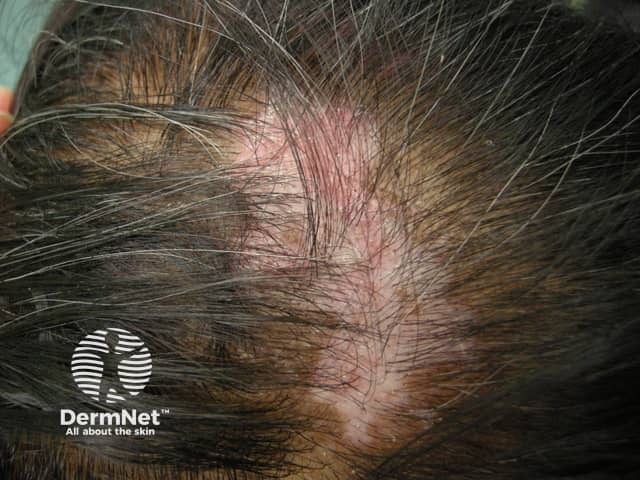
Smoking and discoid lupus erythematosus
Conditions affecting the mouth tend to be more common in smokers. These include:
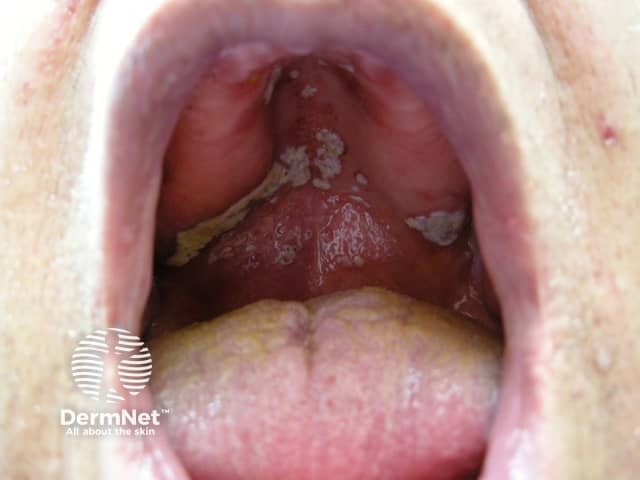
Oral candidiasis
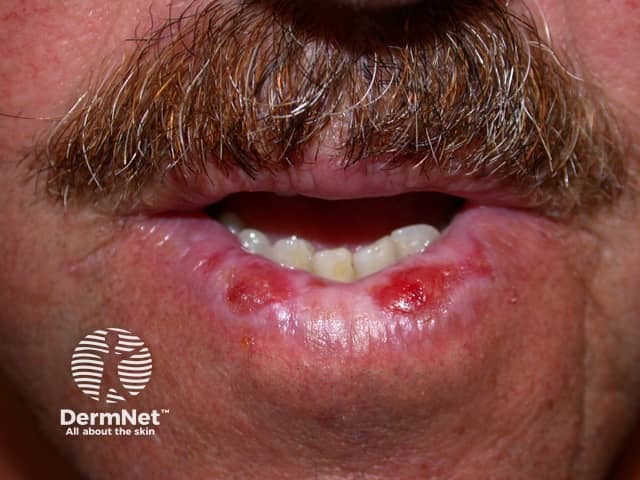
Cheilitis
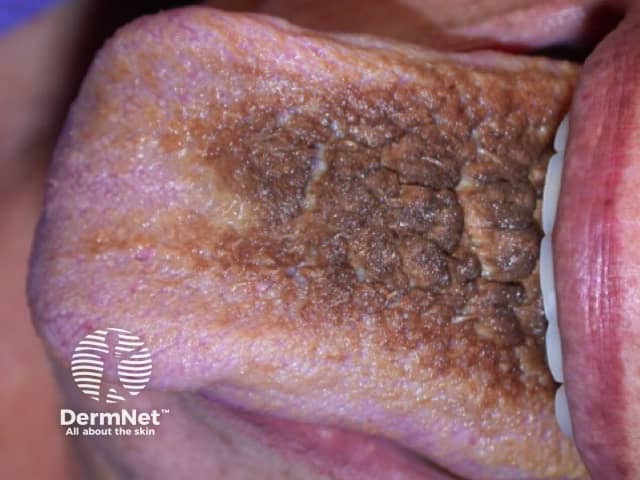
Black hairy tongue
Polycyclic aromatic hydrocarbons from smoking induces CYP1A2 enzymes in the liver. These enzymes destroy toxins. The result is that smokers need higher doses of many medicines compared to non-smokers to achieve the same result. These include insulin, pain relievers, antipsychotics, anticoagulants, caffeine and alcohol.
Alcohol intake and caffeine intake are on average double in smokers. This tolerance of alcohol and caffeine is quickly lost when a smoker stops smoking. Previously tolerated amounts of alcohol and caffeine can thus result in unexpected toxicity.
Alcohol ingestion can also lead to smoking more.
Some inflammatory diseases are less common or less severe in smokers than non-smokers. These include:
However, smoking is not recommended as treatment due to its adverse effects and risk of addiction.
If you want to stop smoking or are thinking about quitting, there are people and services who can help.
A combination of approaches is often best. A meter to measure carbon monoxide in breath can be used to guide treatment.
Nicotine-containing patches, gum, lozenges, nasal spray, inhalers and e-cigarettes may or may not be beneficial to the skin in patients attempting to stop smoking.
Cutaneous side effects may result in poor patient adherence to treatment.