Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Fiona Larsen, Dermatology registrar, Greenlane Hospital, Auckland, New Zealand, 2005.
Hypereosinophilic syndrome is a rare condition defined by three criteria:
The condition largely occurs in males (90%), typically at middle age.
Some patients have an underlying blood disorder present, most commonly a form of leukaemia. Leukaemia may also be diagnosed up to 9-12 years after the initial diagnosis of hypereosinophilic syndrome.
Hypereosinophilic syndrome usually presents with fever, weight loss, fatigue, and rash.
A rash is present in over 50% of patients, but is non-specific in appearance. Most commonly, red swollen itchy nodules (lumps) have been described. It can also resemble urticaria (hives).
An enlarged liver and spleen is often present indicating liver and spleen involvement. The lungs, kidneys, heart and nervous system can be affected.
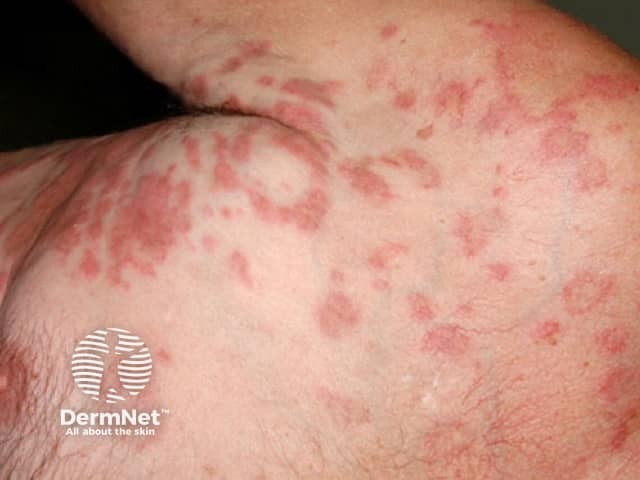
Hypereosinophilic syndrome

Hypereosinophilic syndrome

Hypereosinophilic syndrome
An elevated peripheral blood eosinophil count is found on a full blood count test.
A skin biopsy often reveals an infiltrate of eosinophils.
Approximately 70% of patients respond to high dose oral corticosteroid therapy with oral prednisone, with the eosinophilia returning to normal levels. Other treatments include interferon alpha, hydroxyurea, PUVA therapy and recently imatinib mesylate (Gleevec®) in selected patients. The overall 5-year survival for patients with hypereosinophilic syndrome is 80% and the cause of death is usually heart failure.