Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amy Stanway, Dermatology Registrar, Waikato Hospital, Hamilton, New Zealand, 2003. Updated by A/Prof Amanda Oakley, January 2016.
Introduction
Classification
Demographics
Causes
Clinical features
Diagnosis
Treatment
Outlook
Cutaneous vasculitis is a group of disorders in which there are inflamed blood vessels in the skin. These may include capillaries, venules, arterioles and lymphatics.
In most cases, an underlying cause is not found and the disease is self-limiting.
Cutaneous vasculitis can affect people of all ages and races. Some types of vasculitis have a predilection for certain age groups.
Many different insults may cause an identical inflammatory response within the blood vessel wall. Three main mechanisms are proposed.
Clinical presentation of cutaneous vasculitis mainly depends on the size of the inflamed blood vessel.
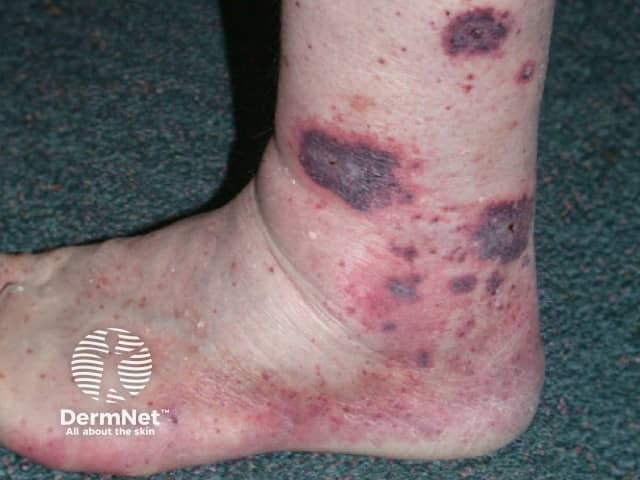
Cutaneous vasculitis

Cutaneous vasculitis

Cutaneous vasculitis

Cutaneous vasculitis

Cutaneous vasculitis
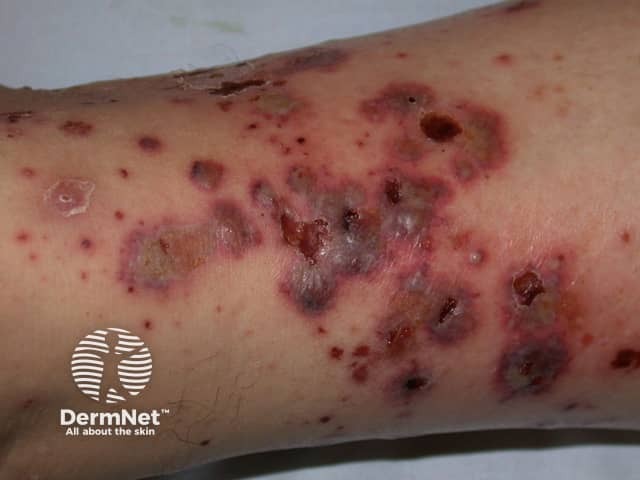
Cutaneous vasculitis
See more images of cutaneous vasculitis ...
The diagnosis of vasculitis can often be made on the basis of its appearance without requiring any further tests. Sometimes a skin biopsy is performed to confirm the diagnosis but this rarely explains what caused it, as vasculitis is the common endpoint of many different events.
Screening tests are requested in most cases of vasculitis to identify any underlying cause and to determine the extent of involvement of internal organs.
Treatment depends on the severity of the disease and may include general measures, systemic corticosteroids, and immune-modulating agents.
If cutaneous vasculitis is a manifestation of systemic vasculitis then treatment of the systemic disorder is required.
Vasculitis limited to the skin has a good prognosis with most cases resolving within a period of weeks to months. The vasculitis may recur at variable intervals after the initial episode.
The prognosis of systemic vasculitis is dependent upon the severity of involvement of other organs. If vasculitis affects the kidneys, lungs or brain it can be life-threatening.