Introduction
Skin and soft tissue infections are a common complication of injecting recreational drugs. Cutaneous abscesses and cellulitis are common presentations in people who inject drugs (PWID), while necrotising fasciitis is a medical emergency.
Who gets skin infections among people who inject drugs?
The practice of injecting subdermally, subcutaneously (‘skin popping’), or intramuscularly (‘muscle popping’) when veins are inaccessible is an important risk factor for developing skin infections. Women are at an increased risk as they may have more difficult venous access. Skin or muscle popping is sometimes done deliberately to cause slower drug absorption and more long-lasting effects.
Other risk factors for skin infections include:
- The use of non-sterile or dirty needles, and sharing equipment
- Injecting a combination of heroin and cocaine (‘speedball’), a potent vasoconstrictor and xylazine
- Drawing blood into the syringe before intravenous injection of the drug (‘booting’ or ‘kicking’)
- Malnutrition
- Infection with HIV
- Other immune disorders that increase susceptibility to infections, such as diabetes.
What causes skin infections in people who inject drugs?
The exact mechanism of infection is related to tissue trauma, ischaemia, and bacterial inoculation. Repeated injections at a single site damage the skin and surrounding tissue, making them more susceptible to infection. The drugs and diluents can increase tissue damage by potentially causing ischaemia, necrosis, vasospasm, and thrombosis.
Infectious pathogens may originate from the skin surface, contaminated needles, or saliva if the injection needle is licked before the injection is administered.
The most common pathogens for bacterial infections include:
- Staphylococcus aureus
- Streptococcus pyogenes and other types of streptococcus
- Organisms originating from the oral flora, such as the Streptococcus anginosus group (SAG; formerly called Streptococcus milleri); and anaerobes such as Veillonella, Fusobacterium, Prevotella species, and Eikenella corrodens.
Uncommon pathogens include:
- Clostridium tetani (which causes tetanus)
- Clostridium botulinum (which causes wound botulism)
- Clostridium sordellii
- Clostridium novyi
- Bacillus cereus
- Bacillus anthracis.
What are the clinical features of skin infections in people who inject drugs?
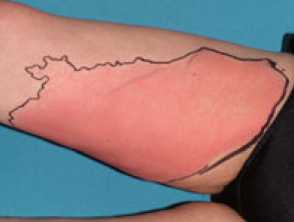
Skin infections present classically with swelling, erythema, warmth, and tenderness. Appearances in intravenous drug users can be atypical, because the skin, venous, and lymphatic systems are damaged by frequent trauma and consequent low-grade infection. This may result in lymphoedema, lymphadenopathy, hyperpigmentation, and scarring.
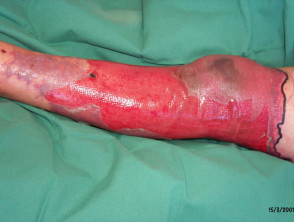
Signs of severe infection include:
- Skin necrosis
- Bullae (which can be haemorrhagic)
- Crepitus
- Fever.
Infections usually affect the arms or legs as these are the sites used most frequently for injection, particularly the antecubital fossa of the non-dominant arm. Unusual sites may be involved (eg, abdomen, back, groin, scrotum, legs, and neck) due to injections in the jugular (neck) or femoral (groin) veins.
Types of infections that may be present include:
- Abscesses (most common) — usually caused by Staph. aureus, although in PWID can contain a mixture of aerobic and anaerobic bacteria; these polymicrobial abscesses often have a foul odour
- Cellulitis — usually caused by Group A streptococci or Staphylococcus aureus
- Skin ulcers — common in IV drug use; generally shallow with hardened edges; can heal with good wound care and oral antibiotics but occasionally require skin grafting
- Necrotising fasciitis — rare but life-threatening, often arising from an injection site on the left arm; treatment requires surgical debridement and antibiotics.
Much rarer infectious complications of intravenous drug use that have characteristic skin findings include:
- Botulism due to Clostridium botulinum toxin, with progressive cranial nerve paralysis
- Tetanus due to Clostridium tetani, resulting in seizures and muscle spasms
- Invasive or widespread fungal infections (candida)
- Heart valve infection (endocarditis) — skin stigmata may include Osler nodes and Janeway lesions and splinter haemorrhages
- HIV infection and AIDS
- Liver disease (eg, secondary to hepatitis B virus or hepatitis C virus).
How do clinical features vary in differing types of skin?
Erythema may be less evident in darker skin types, and the affected skin may appear more dusky or violaceous.
What are the potential complications of skin infections in people who inject drugs?
- Pyomyositis
- Focal or generalised tetanus
- Wound botulism
- Chronic venous insufficiency due to repeated vein injury
- Chronic cutaneous or venous ulcers
- Gangrene
- Sepsis
- Potential sequelae including amputation, chronic pain, and psychosocial effects of chronic wounds
- Endocarditis
- Septic emboli
- Death
How are skin infections in people who inject drugs diagnosed?
Diagnosis is usually made clinically, although laboratory tests and imaging can be useful to confirm the diagnosis and clarify specific aetiologies.
Distinguishing between necrotising and non-necrotising infections can be challenging, and deeper abscesses can sometimes masquerade as cellulitis. Ultrasound, CT, or MRI scans can be helpful in assessing cases further for deep tissue involvement, and potentially guiding therapeutic aspiration. X-rays can help identify underlying osteomyelitis.
Consider sending samples (eg, swabs or aspirates) for microscopy, cultures, and sensitivities; and blood cultures if febrile and there is concern of septicaemia. Inflammatory markers such as white cell count, neutrophil count, and C-reactive protein may be elevated. See also: Laboratory tests for bacterial infections.
What is the differential diagnosis for skin infections in people who inject drugs?
Potential differential diagnoses are broad and, depending on clinical presentation, may include:
- Contact dermatitis
- Drug reactions (see: adverse cutaneous reactions to drugs and drug eruptions)
- Envenomations or insect bites
- Herpes zoster infection/shingles
- Blood vessel problems (eg, venous thrombophlebitis, deep venous thrombosis, vasculitis, mycotic aneurysm)
- Arthritis (eg, septic arthritis, gouty arthritis, or pseudogout)
- Bursitis
- Psoriasis
- Eosinophilic cellulitis (Wells syndrome)
- Carcinoma erysipeloides
- Sweet syndrome (acute febrile neutrophilic dermatosis)
See also: Cellulitis mimics
What is the treatment for skin infections in people who inject drugs?
Treatment of skin and soft tissue infections usually involves empiric antibiotic therapy (consider adjusting if culture and sensitivities are available), +/- an appropriate therapeutic procedure (eg, incision and drainage of an abscess, or surgical debridement).
How do you prevent skin infections in people who inject drugs?
Education around harm reduction — measures and advice to reduce infections include:
- Avoid sharing and reusing needles, syringes, and other equipment
- Use sterile needles and syringes
- Safe disposal of equipment (eg, sharps bins)
- Needle exchange programmes
- Aseptic injection technique
- Clean skin before injecting
- Regular hand hygiene
- Reduce frequency of drug use by injection (eg, through support and treatment options for drug addiction, including opioid substitution programmes).
What is the outcome for skin infections in people who inject drugs?
Both bloodborne viral infections and skin and soft tissue infections increase morbidity and mortality in people who inject drugs. Education about safe injection practices is important. Early diagnosis and appropriate medical care and treatment of infections can help to alleviate symptoms and improve outcomes.