What is keratosis pilaris?
Keratosis pilaris is a very common, dry skin condition caused by keratin accumulation in the hair follicles.
The Latin term keratosis means ‘scaly skin’, and pilaris means ‘hair’. Keratosis pilaris usually starts in childhood but becomes more obvious during the teenage years and adulthood. It is harmless and is not infectious.
Keratosis pilaris
Who gets keratosis pilaris?
Keratosis pilaris is typically seen in children and young adults. It affects 50–70% of teenagers and 40% of adults. It has been associated with other skin diseases such as atopic eczema and ichthyosis.
What causes keratosis pilaris?
Keratosis pilaris occurs due to abnormal keratinisation of the upper portion lining of the hair follicle. The keratin fills the follicle instead of exfoliating.
The cause of keratosis pilaris is not fully understood, but it is thought to have a genetic association with autosomal dominant inheritance. Correlations have been made with mutations in filaggrin (a key protein in skin barrier function).
Keratosis pilaris tends to be prominent in the winter months and is likely due to the reduced moisture content of the air.
What are the clinical features of keratosis pilaris?
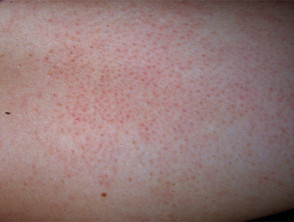
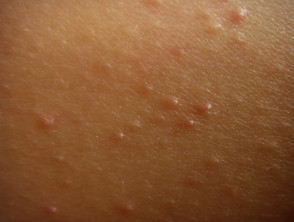
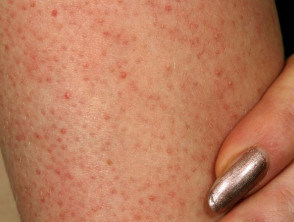
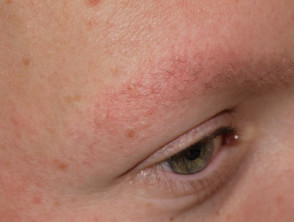
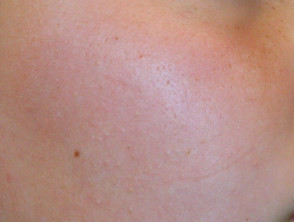
Patients may complain about the ‘goosebump’ or ‘chicken skin’ appearance of their skin. These small bumps can be skin-coloured, red, or brown. The skin can feel rough, dry, and can occasionally be itchy. Redness can also be found around many of the small bumps.
Keratosis pilaris most commonly presents on the extensor surfaces of the upper arms and thighs. The buttocks, trunk, chest, face, and distal extremities can also be involved.
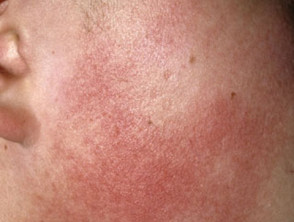
Keratosis pilaris may occasionally be associated with redness and pigmentation of the skin of the cheeks (erythromelanosis folllicularis facei et coli and keratosis pilaris rouge), loss of eyebrow hair (ulerythema ophryogenes), and small atrophic areas over the cheeks (atrophoderma vermiculatum).
Keratosis pilaris
How do clinical features vary in differing types of skin?
The bumps are usually the colour of the patient’s skin. However, they can present as red areas on white skin or brown/black on darker skin.
What are the complications of keratosis pilaris?
- Atrophy
- Scarring with hair loss
How is keratosis pilaris diagnosed?
Keratosis pilaris is a clinical diagnosis. Evaluation of the lesion can aid diagnosis:
- Dermoscopy: reveals abnormalities of the hair shafts — thin, short, coiled, or embedded in the stratum corneum. Scaling and erythema may also be present.
- Punch biopsy: reveals epidermal hyperkeratosis, hypergranulosis, plugged hair follicles, and mild superficial perivascular lymphocytic inflammation.
What is the differential diagnosis for keratosis pilaris?
- Atopic dermatitis
- Folliculitis
- Milia
- Lichen nitidus
- Lichen spinulosus
- Phrynoderma due to nutritional deficiencies
What is the treatment for keratosis pilaris?
General measures
- Use of an exfoliating sponge or scrub in the shower or bath
Specific measures
- Moisturising cream that contains urea, salicylic acid, lactic acid or alpha hydroxy acids (they either moisturise or help loosen the adherent scale in the follicles)
- Topical retinoids
- Short courses of moderate potency topical steroids can be used for itch
- Pulse dye laser treatment or intense pulsed light to help with erythema
- Laser-assisted hair removal for ingrown hairs
What is the outcome for keratosis pilaris?
There is no cure for keratosis pilaris, however, it often clears up during adult life. This is because adults tend to be better at managing the skin condition with the measures discussed above. Any atrophy or scarring with hair loss may be permanent.