What is oral cancer?
There are several types of oral cancers, but over 90% are squamous cell carcinomas. Worldwide, oral cancer is one of the ten most common sites of cancer. People all over the world are affected but it appears to occur most frequently in developing countries particularly India, Pakistan and Bangladesh. In fact, in some parts of India, oral cancer accounts for more than 50% of all cancer.
Who gets oral cancer and why?
Oral cancer usually occurs in people over the age of 40. It is twice as common in men as in women.
Risk factors for developing oral cancer include:
- Smoking: 75% of those diagnosed with oral cancer are tobacco users. The higher the tar yield the greater the risk
- Smoking and alcohol consumption: tobacco and heavy drinking act together to significantly increase the risk (greater than the sum of 2 effects independently)
- Poor oral health
- Infective agents, particularly the wart virus human papillomavirus types 16 and 18, have been implicated in some oral cancers
- The inflammatory disease, erosive oral lichen planus.
What are the signs and symptoms?
Many oral cancers are only detected when they are well advanced. Often in the early stages, the cancer is painless and may go unnoticed. This has led to a high mortality rate compared to cancers of other sites. Thus, the early recognition of signs and symptoms of oral cancer is very important. These include:
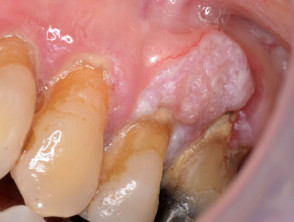
- A white patch (leukoplakia) and/or red patch (erythroplasia) on the gums, tongue, or lining of the mouth
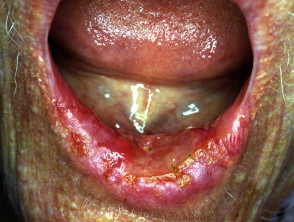
- A small sore or indurated ulcer that looks like a common aphthous ulcer that fails to heal
- A lump or mass that can be felt on the lip or in the mouth or throat
- Unusual bleeding, pain, or numbness in the mouth
- Difficulty or pain with chewing or swallowing
- A persistently sore throat, or a feeling that something is caught in the throat
- Swelling of the jaw that causes dentures to fit poorly or become uncomfortable
- A change in the voice or hoarseness that lasts for a long time
- Pain in the ear
Oral cancer
The most common sites of oral cancer are the lower lip, tongue and the floor of the mouth, although any part of the mouth may be affected. Between 30 and 80% of patients with oral cancer also have secondary lesions (metastases) in the cervical lymph nodes at presentation. At a later stage, cancer may spread to regional lymph nodes, lungs, liver or bones.
Diagnosis and staging of oral cancer
Biopsy of the lesion is performed to get an accurate diagnosis. Dr Philippe Abimelec's video shows how this is done.
After an initial diagnosis of oral cancer, the stage of cancer will be determined. This will define the size of the tumour, how deeply the tumour has invaded tissues at the site of origin, and the extent of any invasion into surrounding organs or lymph nodes. Determining a cancer's stage is an important factor as it directs treatment planning. The 1993 American Joint Committee on Cancer TMN classification and staging of oral cancer is commonly used.
| Classification of oral cancer | ||
|---|---|---|
| Primary tumour | T0 | No primary tumour |
| Tis | Carcinoma in situ | |
| T1 | Tumour 2 cm or less | |
| T2 | Tumour 4 cm or less | |
| T3 | Tumour >4 cm | |
| T4 | Tumour >4 cm and deep invasion into muscle, bone, deep structures | |
| Lymphatic node involvement | N0 | No nodes |
| N1 | Single homolateral node <3 cm | |
| N2 | Node(s) homolateral <6 cm | |
| N3 | Nodes(s) >6 cm and/or bilateral | |
| Tumour metastasis | M0 | No metastasis |
| M1 | Metastasis noted | |
| Staging of oral cancer | |
|---|---|
| Stage I | T1, N0, M0 |
| Stage II | T2, N0, M0 |
| Stage III | T3, N0, M0 T1, T2, T3, N1, M0 |
| Stage IV | T4, N0, M0 Any T, N2 or N3, M0 Any T, any N, any M |
What is the treatment of oral cancer?
Treatment of oral cancer depends on the type of cancer and the stage of the cancer. In general, diagnosis and treatment during the early stages of cancer have a much better outcome. Oral cancer squamous cell carcinoma is generally treated by surgery and/or radiation therapy. Chemotherapy may also be used, particularly in patients with confirmed metastases to other tissues and organs.
Oral health needs are addressed prior to cancer therapy. This is to minimise oral disease and post-therapeutic complications. It appears that up to 97% of patients require oral healthcare before treatment of cancer can begin. Some of the complications that may occur post-cancer treatment are radiotherapy- or chemotherapy-induced mucositis (inflamed mouth), oral ulceration, bleeding, infections, pain, xerostomia (dry mouth) and caries (holes in the teeth).
Surgery is aimed at removing the primary tumour and some of the surrounding normal tissue to make sure the cancer has been completely removed. If done during the early stages of cancer there is usually little or no post-treatment disfigurement. Surgery performed at later stages may also require reconstruction of parts of the mouth or face.