What is sporotrichoid lymphocutaneous infection?
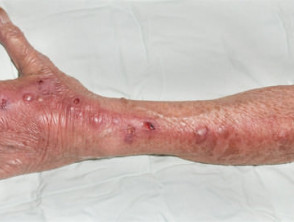
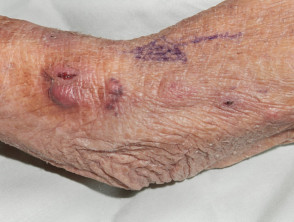
Sporotrichoid lymphocutaneous infection is characterised by the appearance of subcutaneous nodules that progress along dermal and lymphatic vessels. It is also called nodular lymphangitis.
The clinical presentation is often described as sporotrichoid spread. The name 'sporotrichoid' is because the most common infection is sporotrichosis.
Sporotrichoid lymphocutaneous infection
What does sporotrichoid spread look like?
Sporotrichoid spread is mostly observed on an upper limb. The first lesion starts distally, for example, on the hand, wrist or forearm. Subsequent lesions arise proximally, that is, further up the arm, in an irregular, roughly linear, distribution.
Each lesion is an inflamed, irregular, firm nodule, which may suppurate or ulcerate.
What is the cause of sporotrichoid lymphocutaneous infection?
Sporotrichoid lymphocutaneous infection is usually due to an uncommon infection transmitted by primary inoculation through a minor injury or insect bite:
It has also been described with the following infections.
- Fungal infections: coccidioidomycosis, cryptococcosis, blastomycosis, histoplasmosis, Pseudallescheria boydii, Paecilomyces infection
- Bacterial infections: anthrax, Pseudomonas pseudomallei, lepromatous leprosy, lupus vulgaris (cutaneous tuberculosis), Nocardia brasiliensis and N asteroides, Pasteurella tularensis
- Viral infection: Cowpox virus.
Although Staphylococcus aureus and Streptococcus pyogenes are very common causes of bacterial skin infection, they rarely result in sporotrichoid lymphocutaneous infection.
How is the diagnosis of sporotrichoid lymphocutaneous infection made?
Accurate diagnosis requires identification of the causative organism. This may be undertaken by:
- Microscopy and bacterial culture
- Mycological examination and fungal culture
- Skin biopsy for histopathology (which will show granulomas and abscess formation) and special stains to locate and identify the organisms.
How is sporotrichoid lymphocutaneous infection treated?
Treatment depends on the cause, so it is very important to identify the organism before starting a course of antibiotics or oral antifungal medicine. For example:
- Sporotrichosis may be treated by itraconazole or potassium iodide
- Nocardia may be treated with trimethoprim + sulphamethoxazole or minocycline
- Atypical mycobacterial infection may be treated with rifampicin or minocycline
- Leishmania may be treated by stibogluconate or amphotericin.
Other conditions with sporotrichoid spread
Lesions of cutaneous sarcoidosis are also occasionally noted to have sporotrichoid spread.
In-transit metastases are sometimes considered in the differential diagnosis of lymphocutaneous infection, where a secondary tumour – usually melanoma – arises in the skin between the excision site of the primary melanoma and its nearest lymph node.