What is chronic plaque psoriasis?
Chronic plaque psoriasis is the most common form of psoriasis, accounting for more than 80% of cases. It is a chronic relapsing and remitting condition that presents as symmetrical, well-demarcated, erythematous thickened plaques with overlying silver scales.
Appearance can vary depending on skin colour, ranging from pink on lighter skin to brown, purple, or grey on darker skin. It commonly affects the extensor surfaces (elbows and knees), scalp, trunk, and gluteal fold, but may arise on any part of the body. Plaques may coalesce to involve extensive areas of the skin, especially on the trunk and limbs.
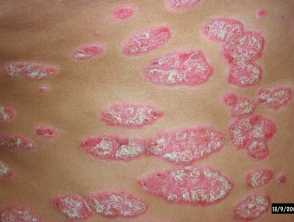
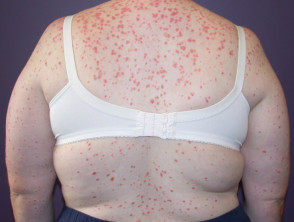
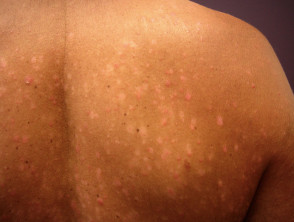
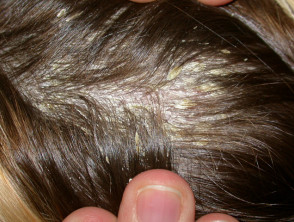
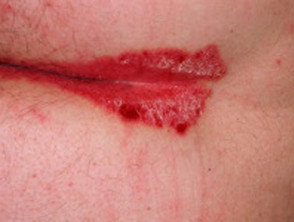
Well-defined scaly plaque psoriasis on the knee Large plaque psoriasis lesions on the trunk - pink, well-defined with overlying thick scale Small plaque psoriasis on the trunk Small plaque psoriasis on the trunk in skin of colour - there is postinflammatory hypopigmentation Well-defined scaly patches of psoriasis in the scalp Flexural psoriasis in the natal cleft - note the absence of scale where the skin surfaces are exposed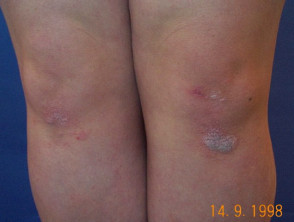
Who gets chronic plaque psoriasis?
Psoriasis affects approximately 125 million people worldwide. It can affect all ages and has no clear sex predilection. Its prevalence ranges from 0–1.4% in children and ranges from 0.5% of adults in Asia to as high as 8% of adults in Norway.
Chronic plaque psoriasis often presents as ‘large plaque’ or ‘small plaque’ psoriasis.
- Large plaque psoriasis commonly has an early age of onset (<40 years) and is often associated with a family history of psoriasis.
- Small plaque psoriasis may arise at any age but often arises in those over 40 years of age. Family history is less common.
What causes chronic plaque psoriasis?
Genetic, environmental, and behavioural factors contribute to psoriasis development, with genetics being the largest risk factor.
Multiple genetic alleles and susceptibility loci that confer risks have been identified, including (but not limited to):
- HLA-Cw6
- HLA-DQ*02:01
- CCHCR1
- CYP1A1
- PSORS1-9.
The human leukocyte antigen (HLA) Cw6 allele is associated with early onset and severe unstable disease.
In susceptible individuals, environmental and behavioural factors such as infections (including streptococcal infections and HIV), smoking, medications (eg, lithium, antimalarials, beta-blockers, terbinafine), skin trauma, and stress can exacerbate psoriasis. Studies have found that psoriasis is more prevalent in Caucasians and in countries at higher latitudes. Psoriasis typically worsens over winter and improves during summer, suggesting that ultraviolet index plays a role, although a small proportion of sufferers experience light-induced exacerbations (photosensitive psoriasis).
The pathogenesis of psoriasis is due to excessive activation of the innate and adaptive immune system. The interaction between T lymphocytes, dendritic cells, neutrophils, and cytokines such as interleukin (IL) 23, IL-17 and tumour necrosis factor (TNF) initiate and perpetuate inflammation. This results in keratinocyte proliferation and immune cell infiltration into lesional skin.
What are the clinical features of chronic plaque psoriasis?
Patients often give a history of itch, especially during flares. Pain occurs when plaques are thickened and cracked.
Typically plaques are well-demarcated, erythematous, scaly, and often symmetrical.
Chronic plaque psoriasis can affect anywhere on the body, such as:
- Scalp — ranges from fine scaling to thick crusted plaques covering the entire scalp
- Face — commonly affects the hairline, forehead, eyebrows, eyelids, ear canals, and behind the ears
- Extensors and trunk — ranges from small scaly papules to large thick plaques with silvery scales
- Flexural areas — well-defined red patches that lack typical scales due to a moist environment, commonly misdiagnosed as fungal infection
- Genital — bright red, shiny patches without scales; occurs in 1/3 of cases, associated with significant impact on quality of life
- Palms and soles — thick, scaly plaques with painful fissures
- Nails — pitting, onycholysis, ridging, and dystrophy.
The plaques may be localised (eg, to elbows and knees) or generalised (involving the scalp, trunk, and limbs).
Other features:
- Koebner phenomenon — psoriasis induced by trauma.
- Auspitz sign — pinpoint bleeding after scales are lifted off a plaque.
Types of chronic plaque psoriasis
Most cases of plaque psoriasis are described as ‘large plaque’ or ‘small plaque’.
- Large plaque psoriasis: thick, well-demarcated, red plaques with a silvery scale; can be more treatment-resistant.
- Small plaque psoriasis: often presents with numerous lesions a few millimetres to a few centimetres in diameter; commonly responds well to phototherapy.
Other (uncommon) subtypes or descriptions of chronic plaque psoriasis include:
- Annular psoriasis — partial central clearing plaques with ring-shaped appearance, associated with good prognosis
- Elephantine psoriasis — large, thick, chronic plaques, typically affects the lower extremities
- Lichenified psoriasis: chronically rubbed or scratched areas of psoriasis that have become very thickened
- Linear psoriasis — psoriasis along Blaschko lines
- Ostraceous psoriasis — very thickly scaled with varying colour and surface, resembling an oyster shell
- Photosensitive psoriasis: while most patients find ultraviolet light helpful for their psoriasis, a small group experience exacerbations following sun exposure, and may have worse symptoms in the sun-exposed areas of the face, neck, hands, and forearms (they may also have typical plaque psoriasis elsewhere); sun protection is important for symptom management in these cases
- Psoriasis geographica — plaques resembling a land map
- Psoriasis gyrate — confluent plaques with a circinate appearance
- Rupioid psoriasis — circular, limpet-like cone-shaped hyperkeratotic plaques.
How do clinical features vary in differing types of skin?
Plaque appearance can vary depending on skin phototype, for example:
- Pale skin — red or pink with silvery white scales
- Light brown skin — salmon coloured with silvery scales
- Dark brown skin — purple or brown patches with grey scales.
What are the complications of chronic plaque psoriasis?
Patients with psoriasis are more likely to have associated health conditions such as:
- Inflammatory arthritis — present in up to 40% of patients with psoriasis and more prevalent in patients with more extensive disease. The 5 major subtypes are:
- Asymmetric oligoarthritis (most common)
- Arthritis of the distal interphalangeal joints
- Rheumatoid arthritis-like presentation
- Spondylitis and sacroiliitis (see: Spondyloarthropathy)
- Arthritis mutilans (least common).
- Reactive arthritis
- Inflammatory bowel disease — Crohn disease or ulcerative colitis
- Metabolic syndrome — obesity, hypertension, hyperlipidaemia, type 2 diabetes
- Cardiovascular disease — myocardial infarction, stroke (chronic vascular inflammation contributing to atherosclerosis)
- Other skin manifestations — palmoplantar pustulosis, generalised pustulosis, acute generalised exanthematous pustulosis.
- Non-alcoholic fatty liver disease
- Malignancy — cutaneous T-cell lymphoma
- Mood disorders — anxiety, depression, suicidal thoughts (see: Psychological effects of psoriasis).
How is chronic plaque psoriasis diagnosed?
Chronic plaque psoriasis is diagnosed based on its clinical features. Categorisation includes localised vs. generalised and large plaque vs. small plaque.
The extent and degree of psoriasis is often assessed by Psoriasis Area and Severity Index (PASI) score.
Dermoscopy of typical plaques may show dotted vessels on a pale red background with uniform white scaling.
Classic histopathological features of plaque psoriasis demonstrate:
- Acanthosis with elongated rete ridges and suprapapillary thinning of the epidermis
- Parakeratosis and neutrophils in stratum corneum
- Dilated capillaries and perivascular lymphocytic infiltration of the dermis.
What is the differential diagnosis for chronic plaque psoriasis?
- Seborrhoeic dermatitis
- Discoid eczema
- Lichen simplex
- Tinea capitis
- Tinea corporis
- Pityriasis rosea
- Pityriasis rubra pilaris
- Cutaneous lymphoma
- Secondary syphilis
What is the treatment for chronic plaque psoriasis?
Treatment goals include symptom management and reducing psychosocial impact.
General measures
- Education on psoriasis.
- Smoking cessation.
- Avoid excessive alcohol.
- Maintain optimal weight.
Specific measures
General considerations when choosing treatment:
- Body site(s) affected and extent and severity of psoriasis
- Impact on quality of life
- Response to previous treatments.
Mild psoriasis is generally treated with topical agents alone, such as:
- Topical corticosteroids
- Vitamin D analogues (eg, calcipotriol)
- Combination calcipotriol/betamethasone dipropionate ointment/gel or foam
- Calcineurin inhibitors
- Salicylic acid: helpful in plaques with thick scale that need to be reduced to enhance penetration of topical medications (eg, scalp psoriasis)
- Coal tar
- Dithranol (rarely used).
If topical therapy is insufficient (eg, in moderate to severe psoriasis), next steps may involve phototherapy, systemic therapy, and biologics.
Most psoriasis centres offer phototherapy, often in combination with topical or systemic agents:
Systemic treatment
Common systemic treatments include:
Other medicines occasionally used:
Biologics or targeted therapies are reserved for severe psoriasis resistant to conventional treatment. They are useful in treating concurrent psoriatic arthritis. These include:
- Tumour necrosis factor inhibitors (anti-TNFα) eg, adalimumab, infliximab, etanercept, and certolizumab
- Interleukin (IL)-12/23 antagonists eg, ustekinumab
- IL-17 antagonists eg, secukinumab, bimekizumab, ixekizumab, and brodalumab
- IL-23 antagonists eg, guselkumab, tildrakizumab, and risankizumab.
Other molecular therapies with evidence for use in psoriasis are:
- Janus kinase (JAK) inhibitors eg, tofacitinib
- Tyrosine kinase (TK) 2 inhibitors eg, deucravacitinib.
A meta-analysis of systemic pharmacological treatment for chronic plaque psoriasis found that compared to placebo, biologic agents infliximab, bimekizumab, ixekizumab, and risankizumab were the most effective in achieving 90% improvement in PASI score from baseline at 6 months follow up in patients with moderate to severe psoriasis.
How do you prevent chronic plaque psoriasis?
There is no way to prevent psoriasis but there are ways to minimise symptoms and reduce flare-ups. This includes:
- Regular use of emollients
- Quitting smoking
- Limiting alcohol intake
- Reducing stress
- Exercise, healthy diet, and maintaining optimal weight/BMI.
What is the outcome for chronic plaque psoriasis?
While there is no cure for psoriasis, the therapeutic advancements in biologics have transformed care for patients with moderate to severe disease, making complete clearance a realistic goal.
However, most patients have mild to moderate psoriasis and unfortunately, there have been a limited number of new therapeutic developments for these patients. Topical treatment remains the mainstay of treatment, and it is hoped that new agents such as tapinarof, the PDE4 inhibitor roflumilast, and small molecule topical JAK inhibitors may be more accessible for patients with moderate disease in the future.