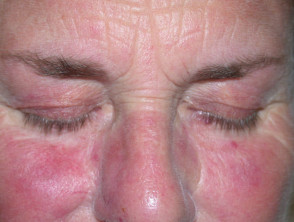
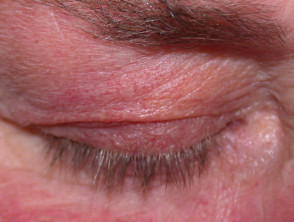
What is telangiectasia?
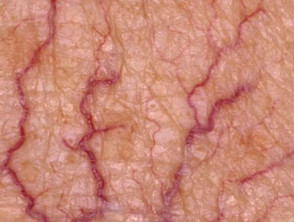
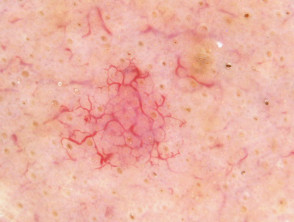
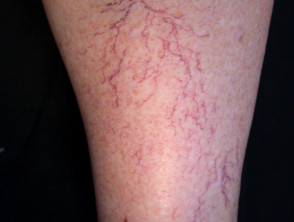
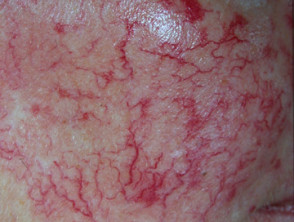
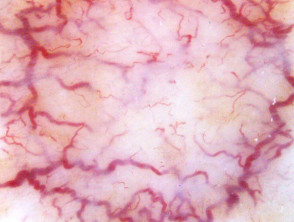
Telangiectasia is a condition in which there are visible small linear red blood vessels (broken capillaries). These are also called telangiectases. Visible small blood vessels that are blue in colour (spider veins) are called venulectasia because venules are involved.
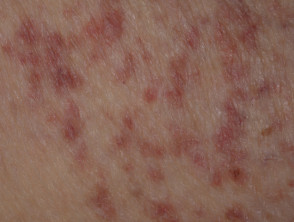
Telangiectasia
What is the differential diagnosis of telangiectasia?
Telangiectases need to be distinguished from other vascular conditions, including blood vessel tumours such as infantile haemangioma and angiomas that arise in adults; and capillary or venous vascular malformations.
Large red blood vessels are arteries and large blue blood vessels are veins. Arteries may be enlarged due to aneurysm formation. Veins enlarged due to the destruction of their valvular system are known as varicose veins.
Classification of telangiectasia
Inherited conditions
- Hereditary haemorrhagic telangiectasia
- Benign hereditary telangiectasia
- Generalised essential telangiectasia
- Unilateral naevoid telangiectasia
- Angioma serpiginosum
- Rothmund Thompson syndrome
- Ataxia-telangiectasia
- Bloom syndrome (congenital telangiectatic erythema)
- Cockayne syndrome
- Cutis marmorata telangiectatica congenita
- Focal dermal hypoplasia (Goltz syndrome)
- Kindler syndrome
Note that telangiectasia may be noted as a normal feature of facial skin in some families.
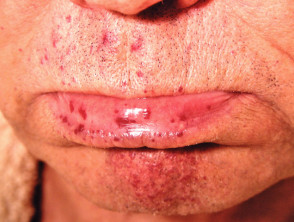
Hereditary telangiectasia
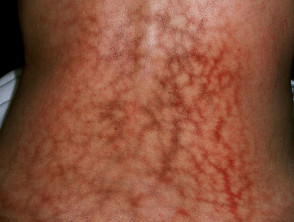
Acquired telangiectasia
- Rosacea
- Sun damaged and aged skin especially in those who smoke
- Spider telangiectasis (also called spider naevus)
- Poikiloderma of Civatte (sun damage affecting the sides of the neck)
- Pregnancy
- Liver disease particularly when associated with alcohol or viral infection
- Cushing syndrome
- Systemic sclerosis especially CRST syndrome (which forms telangiectatic mats)
- Cutaneous lupus erythematosus
- Mixed connective tissue disease
- Dermatomyositis
- Mastocytosis, specifically the variant, telangiectasia macularis eruptiva perstans
- Carcinoid syndrome
- Necrobiosis lipoidica
- Male genital dysaesthesia
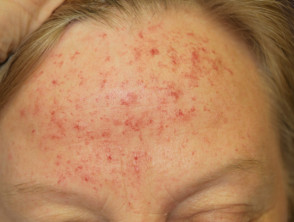
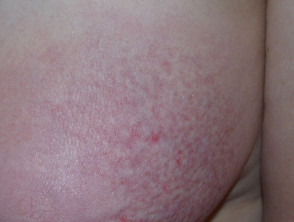
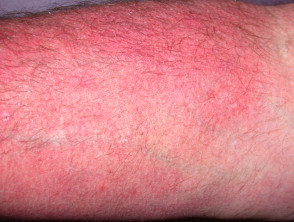
Telangiectasia due to disease
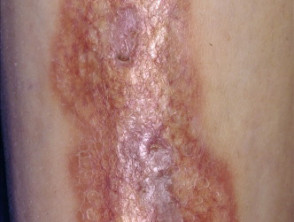
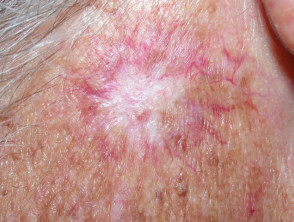
Telangiectasia may follow a cutaneous injury. For example:
- Scarring, including hypertrophic and keloid scars
- Livedoid vasculopathy and atrophie blanche
- Radiation damage
- Erythema ab igne.
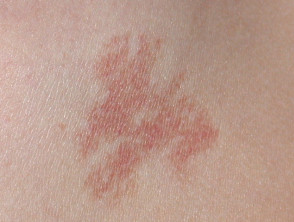
Telangiectasia following injury
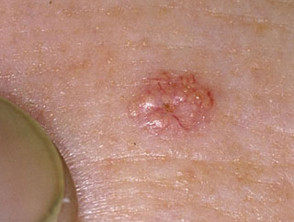
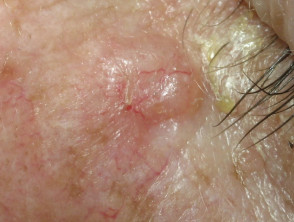
Some tumours are characterised by telangiectasia, such as:
- Sebaceous hyperplasia
- Basal cell carcinoma
- Merkel cell carcinoma
- Kaposi sarcoma
- Cutaneous T-cell lymphoma (CTCL), particularly poikiloderma vasculare variant
- Intravascular B-cell lymphoma.
Telangiectasia in skin tumours
Certain medications may give rise to telangiectasia.
- Vasodilators especially calcium channel blockers; sun-exposed sites are mainly affected
- Long-term systemic corticosteroids
- Long-term topical corticosteroids, including steroid rosacea
- Intralesional triamcinolone injections
Telangiectasia related to topical steroid use
What is the treatment of telangiectasia?
Telangiectases are generally harmless. Treatment may be sought because of bleeding or unsightly appearance. Facial red vein treatment methods include: