What is carotenoderma?
Carotenoderma is the yellow-orange discolouration of the skin due to carotenaemia (American spelling: carotenemia), a condition in which the blood level of β-carotene is elevated above the normal range.
Carotenoderma
What is β-carotene?
β-carotene and other carotenoids (eg alpha-carotene, lycopene, canthaxanthin, lutein) are a normal part of our diet. They contribute to the normal colour of our skin and help protect us from sunburn.
Carotenoids are precursors of vitamin A (retinol). Carotene is mainly absorbed in the proximal small intestine and most is converted into vitamin A in the mucosa: the remainder enters the portal circulation and is carried to the liver. Pancreatic lipase enzymes, bile salts, fat, and thyroid hormone aid conversion of carotenoids to vitamin A. Carotenoids are cleared from the body in sweat, sebum, urine, and faeces.
β-carotene has been touted as an antioxidant and free-radical scavenger, potentially useful for photoprotection in patients with erythropoietic protoporphyria and congenital erythropoietic porphyria.
Who gets carotenoderma?
Carotenoderma can affect all ages, both sexes, and all races, although it may be more common in some groups due to a diet high in β-carotene.
Groups particularly affected include:
- Related to dietary intake
- Young children fed large amounts of commercial infant foods made from fruit and vegetables that are high in β-carotene such as carrot, sweet potato, and pumpkin. Cooking, mashing, and pureeing these foods increases the bioavailability.
- Vegetarians, vegans, and those on other restricted diets high in β-carotene
- Endemic in West Africa due to ingestion of red palm oil.
- Associated medical conditions
- Diabetes mellitus
- Hypothyroidism
- Liver disease
- Kidney disease
- Anorexia nervosa.
What causes carotenoderma?
Carotenoderma is due to carotenaemia.
- Primary carotenaemia is usually due to excessive intake of carotenoid-containing foods or supplements.
- Carotene is found in all pigmented fruits and vegetables. High levels are associated with a deep yellow, orange, or green colour. Examples of fruit and vegetables with a high β-carotene content include mango, papaya, pumpkin (squash), carrot, and sweet potato. The green colour of chlorophyll may mask the underlying yellow, such as in broccoli.
- Dairy products such as butter, cheese, and milk
Carotene-rich foods
- Secondary carotenaemia due to medical conditions mostly have in common reduced conversion of β-carotene to retinol and/or hyperlipidaemia. There is a linear relationship between β-carotene levels and β-lipoprotein levels.
- Metabolic carotenaemia is due to defective conversion of β-carotene to vitamin A and may be familial.
What are the clinical features of carotenoderma?
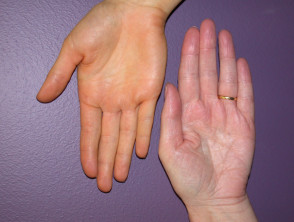
Carotenoderma presents as a yellow-orange hue to the skin.
- Initially seen as yellow discolouration of the nose, nasolabial folds, palms, and soles before gradually spreading over the whole body
- Carotene present in sebum and sweat deposits in the fat-soluble stratum corneum so the yellow skin colour is particularly seen where sweating is marked, and on the palms and soles due to the thickness of the stratum corneum
- Best seen under artificial light
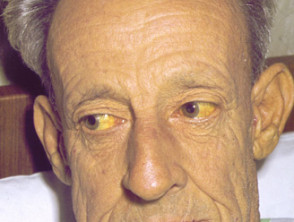
Of note, the sclerae of the eyes and mucous membranes, which lack a stratum corneum, are unaffected by carotenaemia. Yellow sclerae indicate jaundice.
Jaundice
How do clinical features vary in differing types of skin?
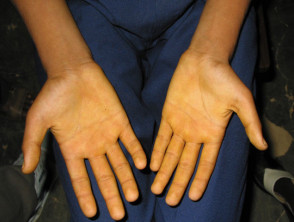
Yellow discolouration of the palms and soles is more easily seen in lighter Fitzpatrick skin types but may be subtle. Darker Fitzpatrick skin types may show yellowing of the palms and soles with associated lightening of other areas such as the face.
What are the complications of carotenaemia?
- Vitamin A toxicity is not usually associated with carotenaemia, even if vast amounts of carotenoids are consumed, because conversion of carotene to vitamin A is a slow process.
- Canthaxanthin, a toxic carotenoid metabolite still available as a non-prescription “tanning” pill, may cause retinopathy in excess amounts. However, reports suggest the retinopathy to be reversible with no long-term sequelae.
- Amenorrhoea may be associated, perhaps due to malnutrition or lack of red meat in a vegetarian diet high in carotene.
How is carotenoderma diagnosed?
- Patient history and physical examination are usually sufficient to make the diagnosis of carotenoderma which may be confirmed, if considered necessary, by high serum carotene levels with normal liver function and normal or slightly elevated levels of vitamin A. However, reference ranges are variable so interpretation can be difficult.
- Skin biopsy is not usually required but may show a pemphigus vulgaris-like pattern on direct immunofluorescence staining.
- If there is no history of excess carotenoid ingestion or physical examination suggests an underlying medical condition, the patient should be investigated appropriately.
What is the differential diagnosis for carotenoderma?
- Jaundice
- Ingestion or percutaneous absorption of drugs or chemicals, such as quinacrine, dinitrophenol, saffron, tetryl and picric acids, canthaxanthin, acroflavine
- Lycopenaemia presents with orange-yellow skin discolouration due to ingestion of large amounts of tomatoes or other fruits that contain lycopene
- Fake tan
What is the treatment for carotenoderma?
- Treatment of carotenoderma is usually just a matter of reducing carotene intake by dietary modification
- Patients with secondary carotenaemia should be treated for the underlying medical condition.
What is the outcome for carotenoderma?
Carotenoderma is a benign condition. The skin colour should return to normal but may take several months due to accumulation of β-carotene in tissue.