Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Vanessa Ngan, Staff Writer, 2003; Updated: Casey P Schukow, Medical Student, Michigan State University College of Osteopathic Medicine, Detroit MI, United States of America; Dr Martin Keefe, Dermatologist, Christchurch, New Zealand. Copy edited by Gus Mitchell. June 2021
Introduction
Introduction β-carotene
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Carotenoderma is the yellow-orange discolouration of the skin due to carotenaemia (American spelling: carotenemia), a condition in which the blood level of β-carotene is elevated above the normal range.
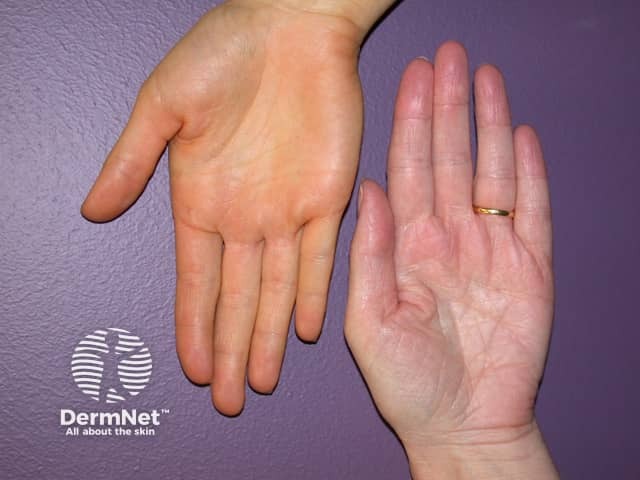
Normal palm colour and carotenoderma
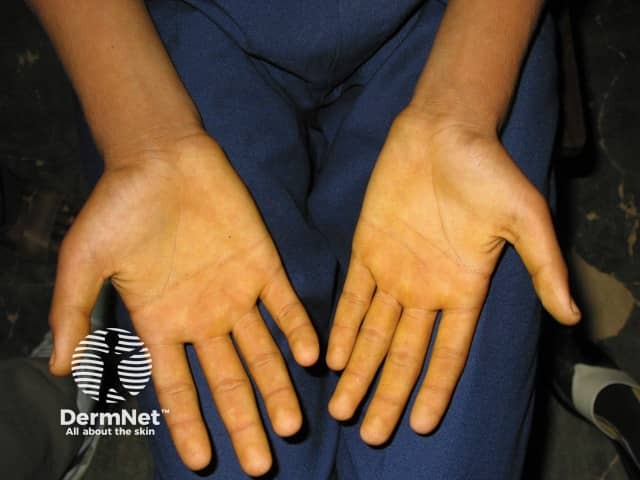
Orange-yellow palms of carotenoderma
β-carotene and other carotenoids (eg alpha-carotene, lycopene, canthaxanthin, lutein) are a normal part of our diet. They contribute to the normal colour of our skin and help protect us from sunburn.
Carotenoids are precursors of vitamin A (retinol). Carotene is mainly absorbed in the proximal small intestine and most is converted into vitamin A in the mucosa: the remainder enters the portal circulation and is carried to the liver. Pancreatic lipase enzymes, bile salts, fat, and thyroid hormone aid conversion of carotenoids to vitamin A. Carotenoids are cleared from the body in sweat, sebum, urine, and faeces.
β-carotene has been touted as an antioxidant and free-radical scavenger, potentially useful for photoprotection in patients with erythropoietic protoporphyria and congenital erythropoietic porphyria.
Carotenoderma can affect all ages, both sexes, and all races, although it may be more common in some groups due to a diet high in β-carotene.
Groups particularly affected include:
Carotenoderma is due to carotenaemia.

Pumpkin

Sweet potato

Broccoli
Carotenoderma presents as a yellow-orange hue to the skin.
Of note, the sclerae of the eyes and mucous membranes, which lack a stratum corneum, are unaffected by carotenaemia. Yellow sclerae indicate jaundice.
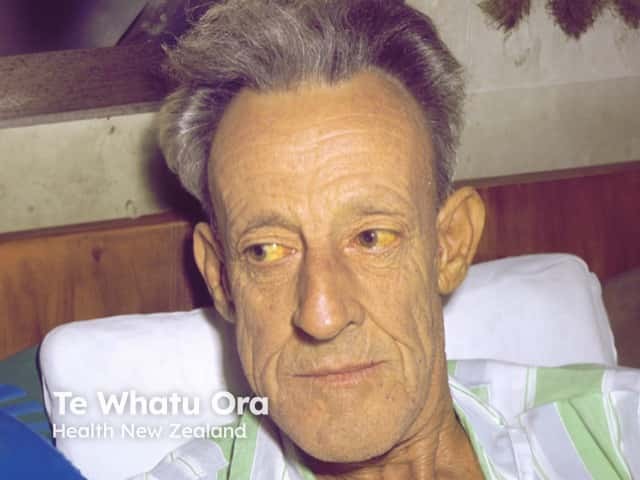
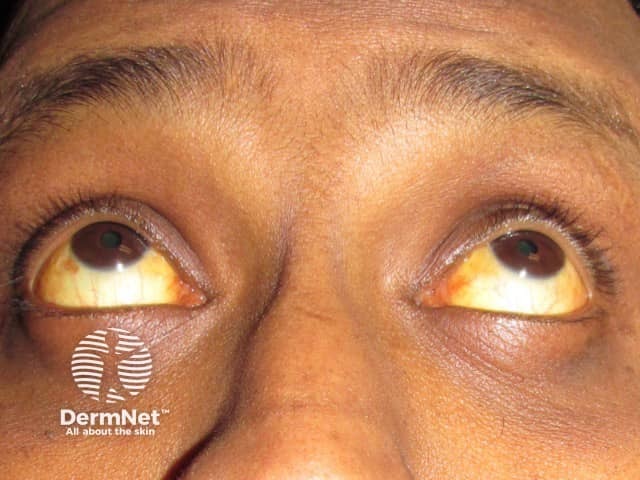
Jaundice
Yellow discolouration of the palms and soles is more easily seen in lighter Fitzpatrick skin types but may be subtle. Darker Fitzpatrick skin types may show yellowing of the palms and soles with associated lightening of other areas such as the face.
Carotenoderma is a benign condition. The skin colour should return to normal but may take several months due to accumulation of β-carotene in tissue.