Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2003.
Introduction Causes Clinical features Diagnosis Differential diagnoses Treatment
Athlete's foot is a term often used to describe a fungal infection (or dermatophytosis) of the foot (tinea pedis).
It most often results in peeling skin and fissuring between the toes (the toe clefts). The cleft between the fourth and fifth toes is the most frequently affected.
Fungal infection is not the only reason for peeling and fissuring between the toes, and the term athlete's foot is sometimes used to refer to any condition where the toe clefts are inflamed.
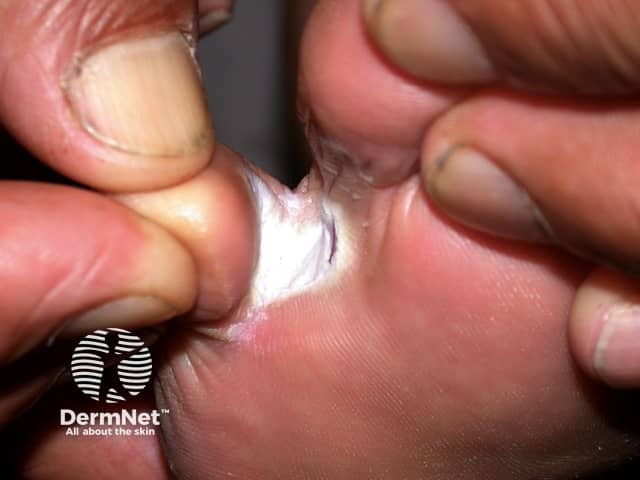
Athlete foot
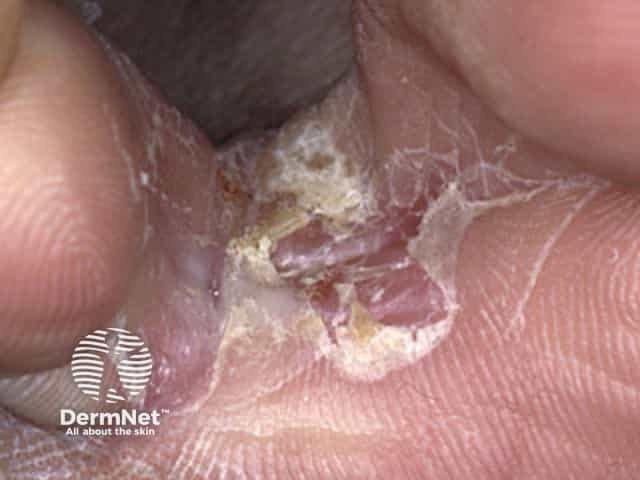
Athlete foot
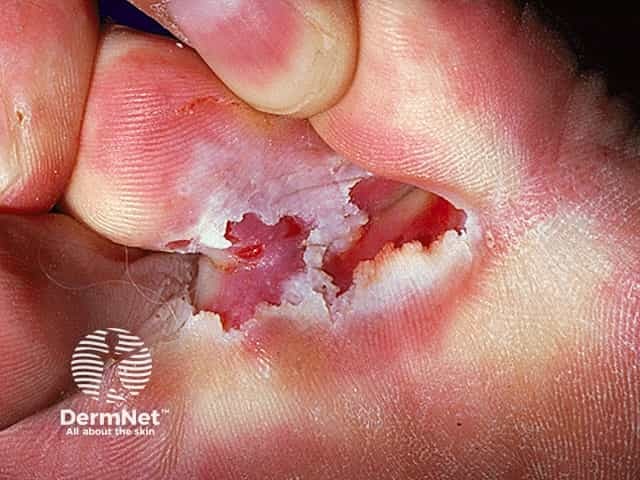
Athlete foot
Athlete's foot is generally due to proliferation of dermatophyte fungi of the genera Trichophyton rubrum, Trichophyton interdigitale, and Epidermophyton floccosum.
Athlete's foot is more common in those who participate in sports because:
The clinical features of athlete's foot may include:
Athlet's foot is generally mild; very inflamed athlete's foot is generally due to secondary bacterial infection.
The diagnosis is usually clinical, as athlete's foot has a characteristic appearance. If resistant to treatment, investigations are undertaken to identify a specific infection.
Athlete's foot is a localised interdigital form of intertrigo.
Apart from tinea pedis, peeling and fissuring between the toes can be due to:
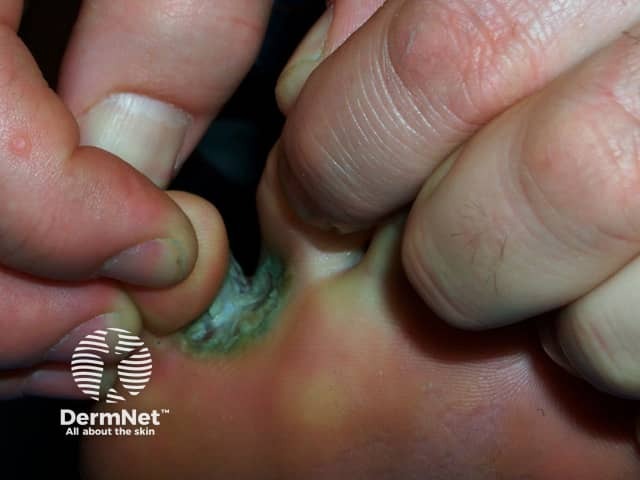
Pseudomonas infection
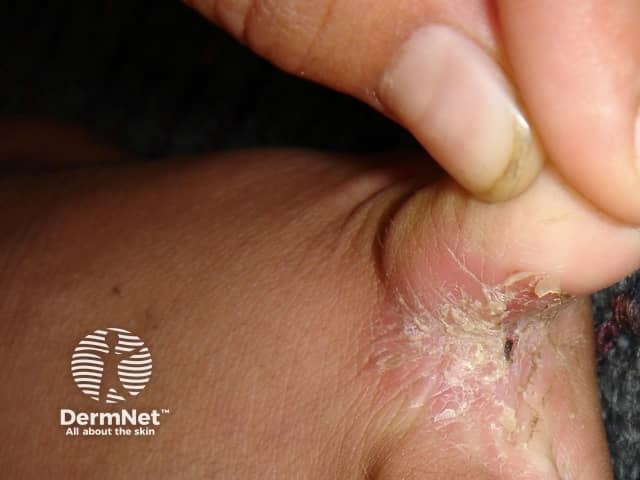
Psoriasis
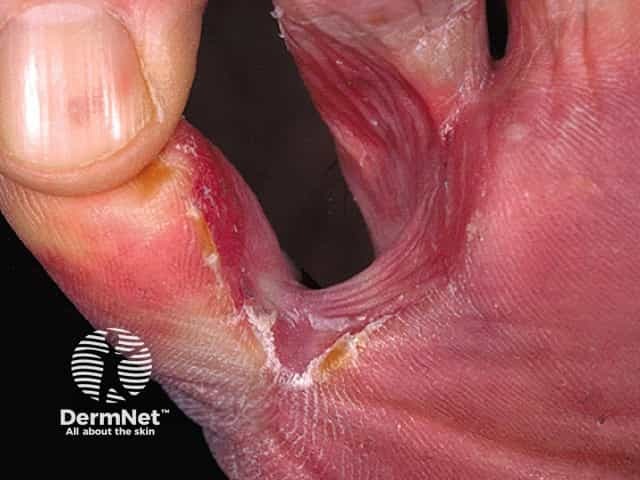
Eczema
Treatment for athlete's foot should begin with general measures.
Whitfield ointment (3% salicylic acid, 6% benzoic acid in petrolatum) is particularly useful, as it removes the surface layer of moist peeling skin (ie, it is keratolytic), and it eliminates bacteria and fungi.
Make sure that other sites of fungal infection are also treated effectively.