Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1998. Revised and updated August 2015. Updated by Janet Dennis, November 2018. Technical Editor: Mary Elaine Luther, Medical Student, Ross University, Barbados. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. January 2020.
Introduction
Demographics
Clinical features
Causes
Investigations
Treatment
Intertrigo describes a rash in the flexures, such as behind the ears, in the folds of the neck, under the arms, under a protruding abdomen, in the groin, between the buttocks, in the finger webs, or in the toe spaces. Although intertrigo can affect only one skin fold, intertrigo commonly involves multiple sites. Intertrigo is a sign of inflammation or infection.
Intertrigo can affect males or females of any age. Intertrigo is particularly common in people who are overweight or obese (see metabolic syndrome).
Other contributing factors are:
In infants, napkin dermatitis is a type of intertrigo that primarily occurs due to skin exposure to sweat, urine, and faeces in the diaper area.
Toe-web intertrigo is associated with closed-toe or tight-fitting shoes. Lymphoedema is also a cause for toe-web intertrigo.
Intertrigo can be acute (recent onset), relapsing (recurrent), or chronic (present for more than six weeks). The exact appearance and behaviour depend on the underlying cause(s).
The skin affected by intertrigo is inflamed, reddened, and uncomfortable. The affected skin can become moist and macerated, leading to fissuring (cracks) and peeling.
Intertrigo with secondary bacterial infection (eg, pseudomonas) can cause a foul odour.
Intertrigo is due to genetic and environmental factors.
The microbiome (microorganisms normally resident on the skin) on flexural skin includes Corynebacterium, other bacteria, and yeasts. Microbiome overgrowth in warm moist environments can cause intertrigo.
Intertrigo is classified into infectious and inflammatory origins, but they often overlap.
Thrush: Candida albicans
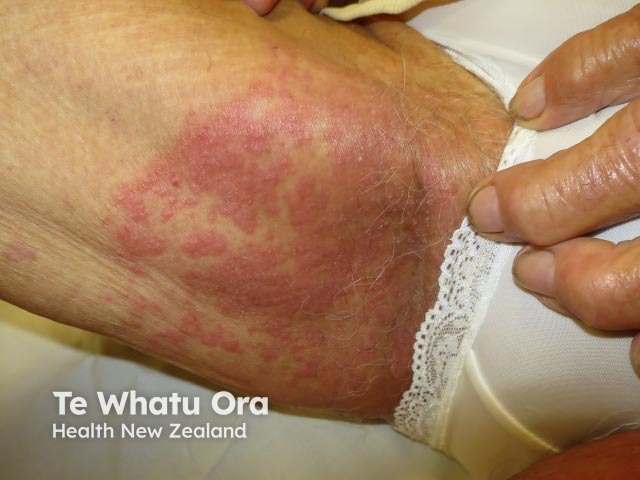
Intertrigo due to candida infection
Erythrasma: Corynebacterium minutissimum
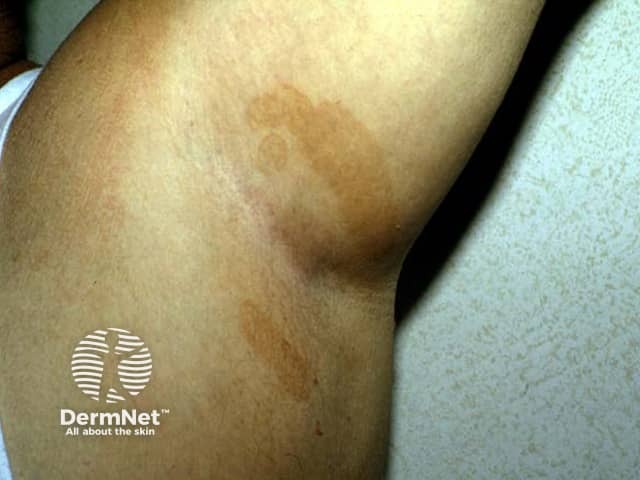
Axillary erythrasma
Tinea: Trichophyton rubrum + T. interdigitale
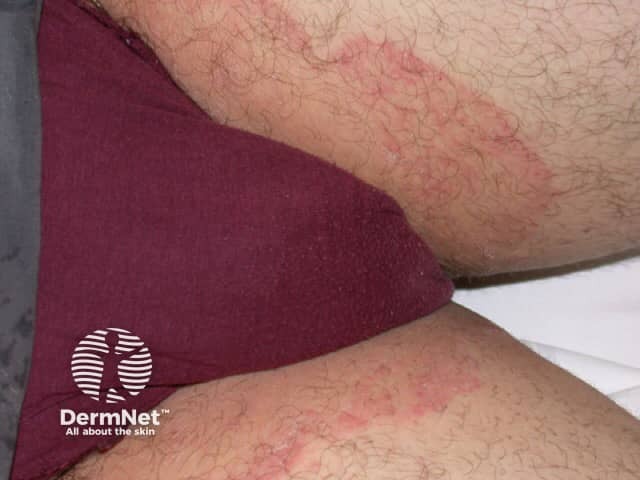
Tinea cruris
Impetigo: Staphylococcus aureus and Streptococcus pyogenes
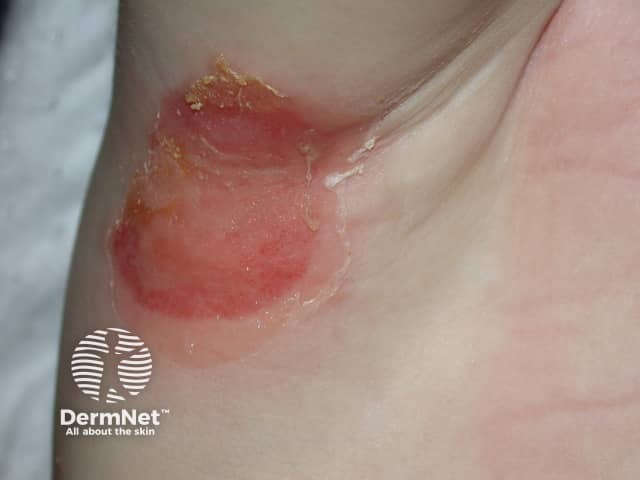
Bullous impetigo
Boils: Staphylococcus aureus
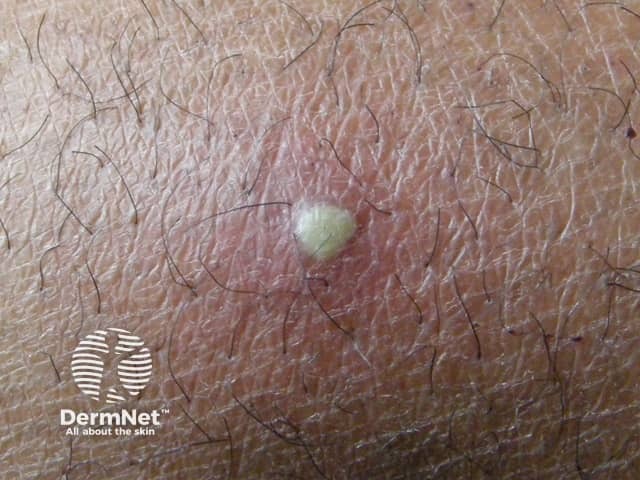
Boil
Folliculitis: Staphylococcus aureus
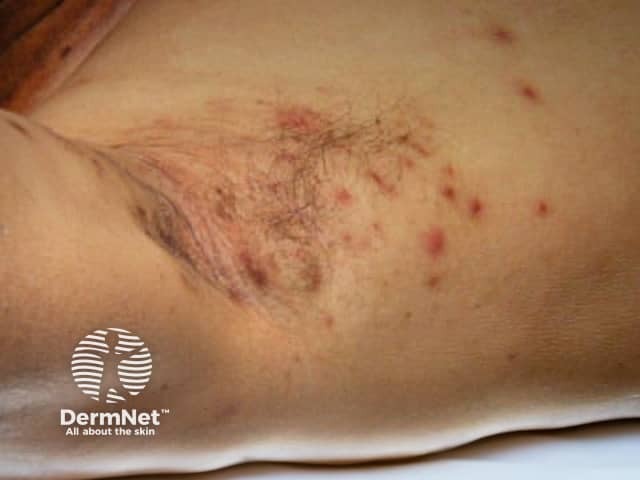
Folliculitis in axilla
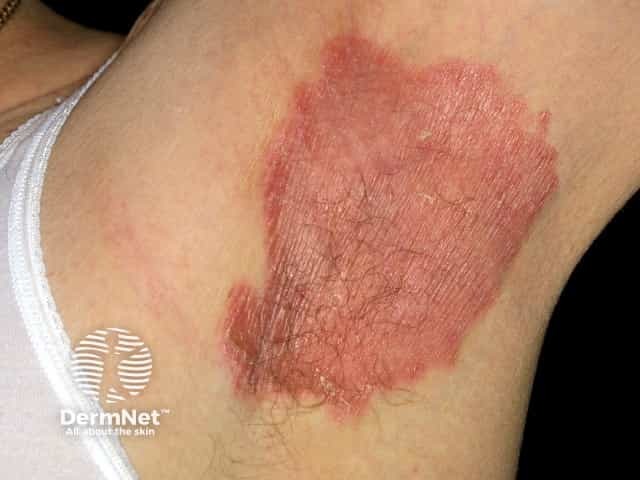
Flexural psoriasis
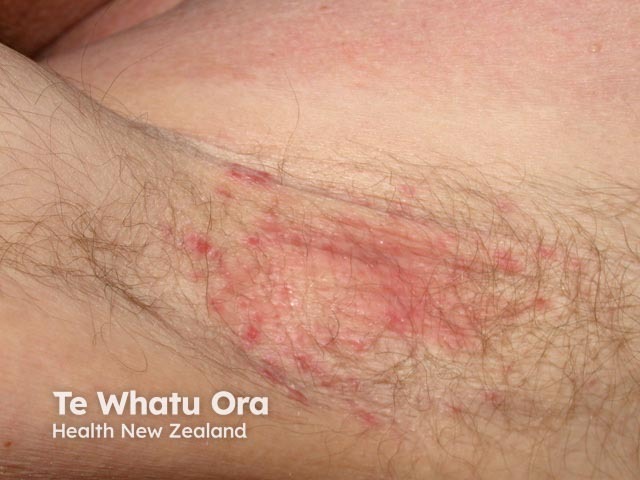
Intertrigo due to seborrhoeic dermatitis
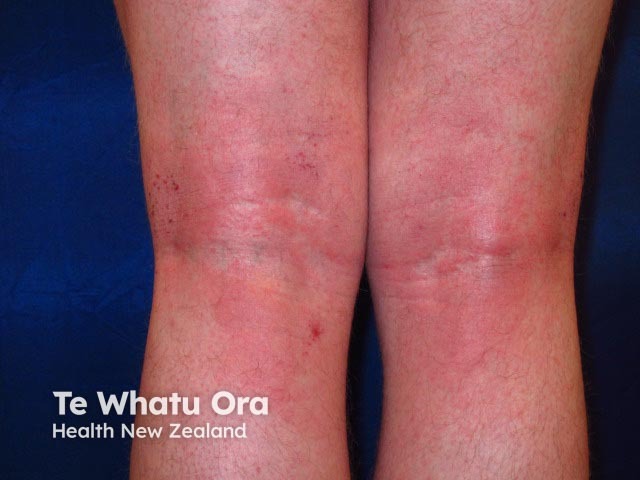
Flexural eczema
Irritants include:
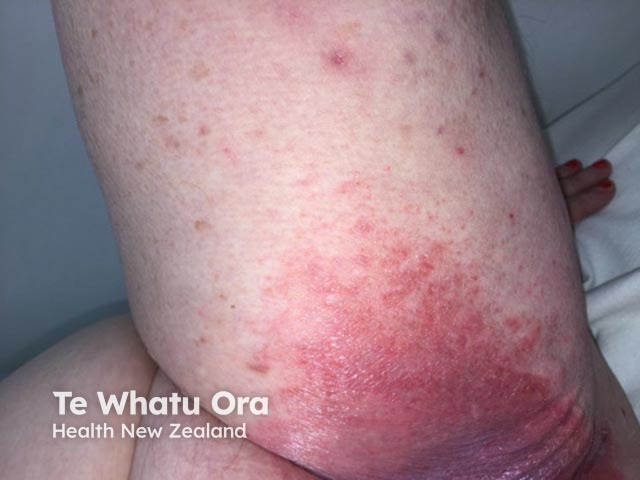
Contact irritant dermatitis due to urine. Napkin dermatitis in adult
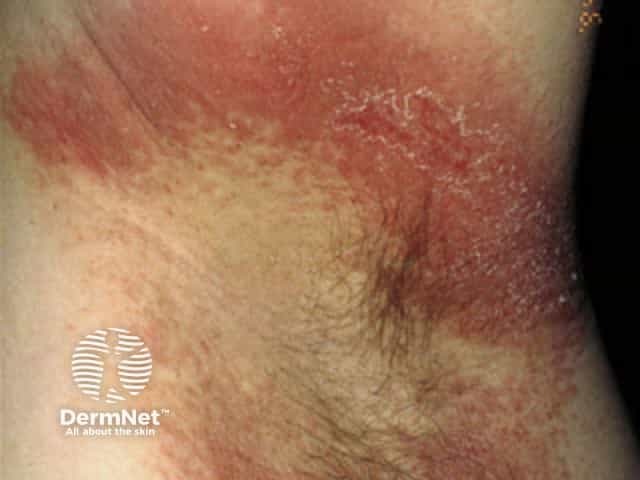
Intertrigo due to contact allergy to benzocaine
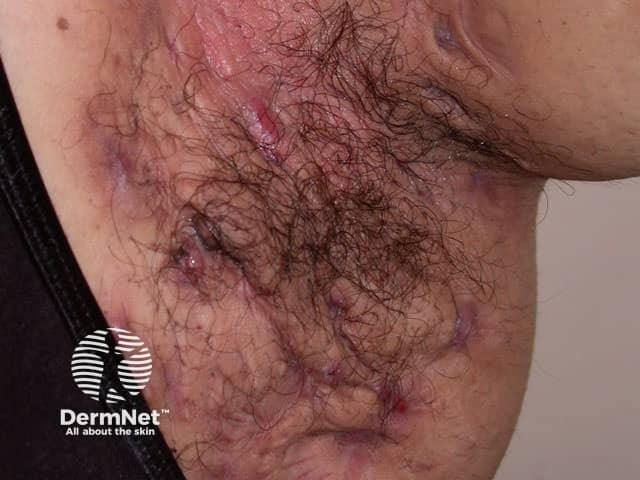
Intertrigo due to hidradenitis suppurativa in axilla
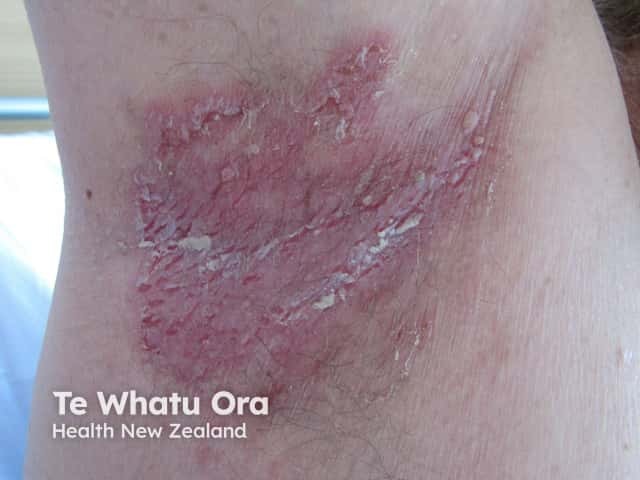
Intertrigo due to Hailey-Hailey disease
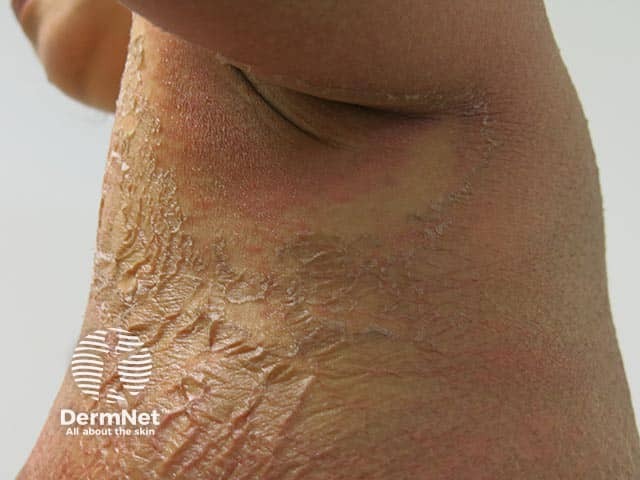
Granular parakeratosis
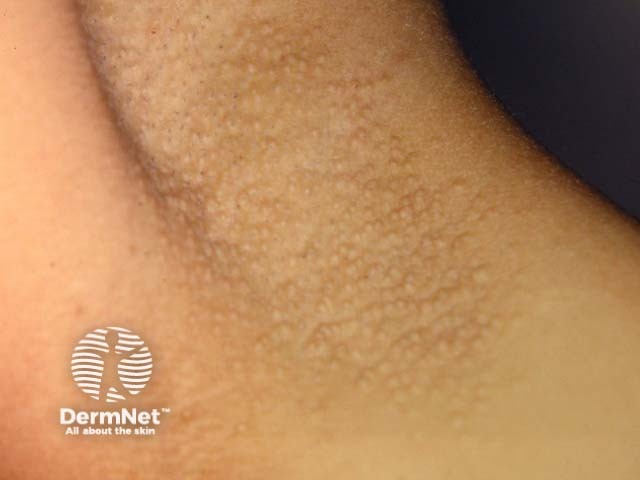
Axillary Fox-Fordyce disease
Toe-web intertrigo
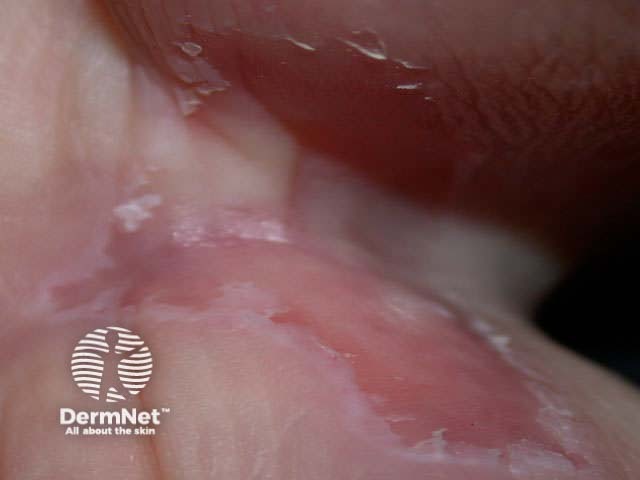
Athlete's foot
Investigations may be necessary to determine the cause of intertrigo.