Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2003. Updated: Dr Harriet Bell, House Officer, Auckland City Hospital, Auckland, New Zealand. Copy edited by Gus Mitchell. November 2020.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Tinea corporis is a superficial fungal infection of the skin that can affect any part of the body, excluding the hands and feet, scalp, face and beard, groin, and nails. It is commonly called ‘ringworm’ as it presents with characteristic ring-shaped lesions.
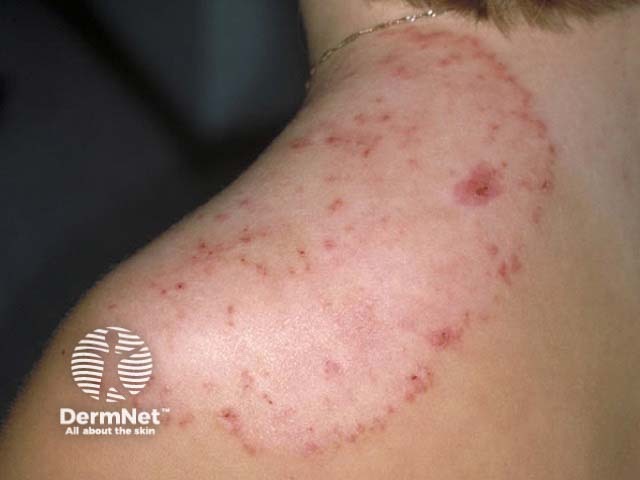
Tinea corporis
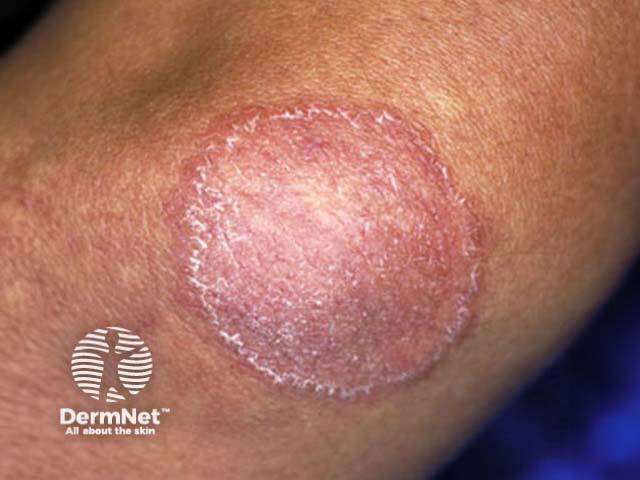
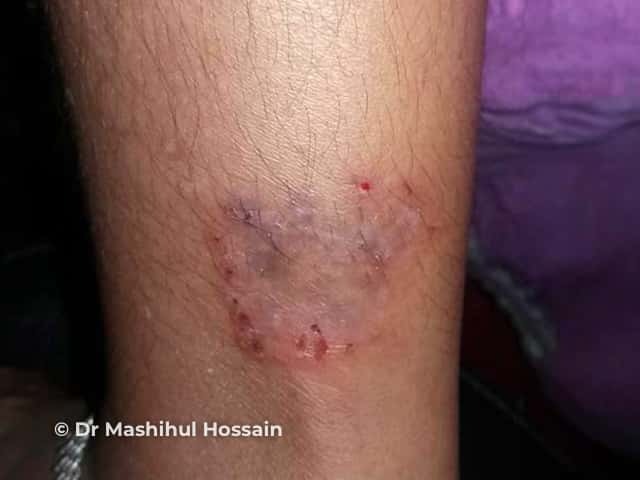
Tinea corporis is found in most parts of the world, but particularly in hot humid climates. It is most commonly seen in children and young adults, however all age groups can be infected including newborns.
Medical risk factors include:
Environmental risk factors include:
A genetic predisposition has been postulated, particularly for tinea imbricata.
Tinea corporis is predominantly caused by dermatophyte fungi of the genera Trichophyton and Microsporum. The anthropophilic species T. rubrum is the most common causative agent of tinea corporis worldwide including New Zealand. Other species that may cause tinea corporis include:
Tinea corporis is spread by the shedding of fungal spores from infected skin. Transmission is facilitated by a warm, moist environment and the sharing of fomites including bedding, towels, and clothing. Dermatophyte infection elsewhere on the skin, such as tinea pedis, can also be transferred. The incubation period is 1–3 weeks. The dermatophyte invades and spreads in the stratum corneum, but is unable to penetrate deeper layers in healthy skin.
Tinea corporis initially presents as a solitary circular red patch with a raised scaly leading edge. A lesion spreads out from the centre forming a ring-shape with central hypopigmentation and a peripheral scaly red rim (ringworm). The border can be papular or pustular. Itch is common. With time, multiple lesions can develop which may coalesce to form a polycyclic pattern. The distribution of lesions is typically asymmetrical.
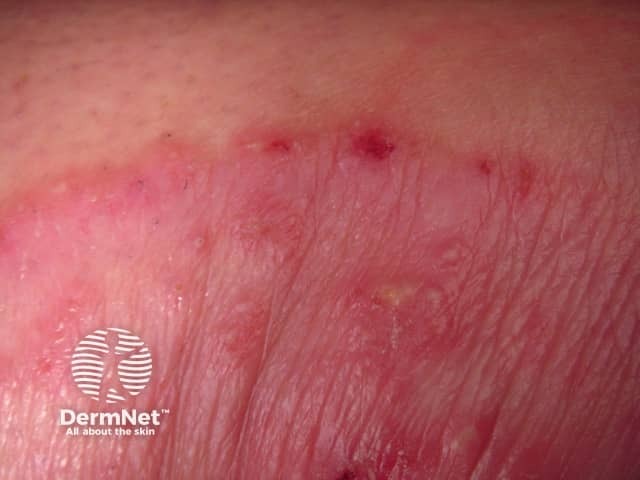
Sharp red scaly margin of tinea corporis
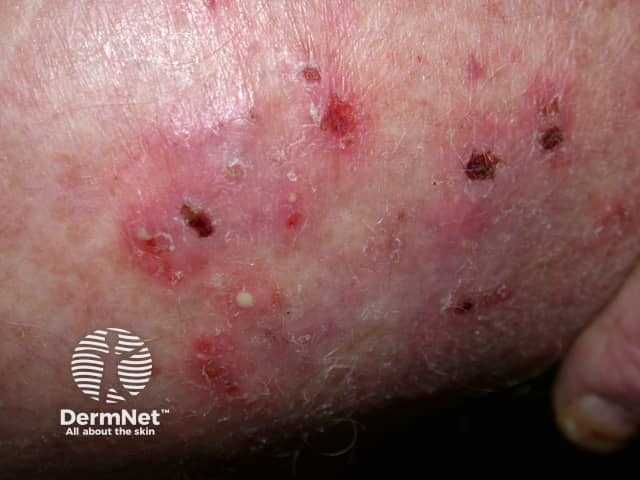
Papules and pustules of tinea corporis
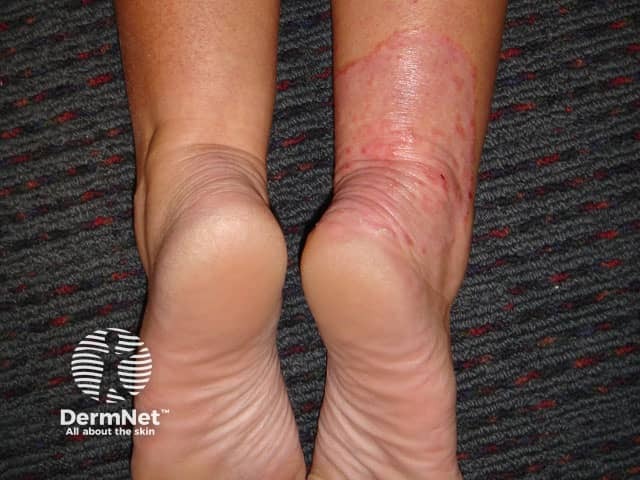
Asymmetry of tinea corporis
See also Tinea corporis images
Clinical variants of tinea corporis can include the following types.
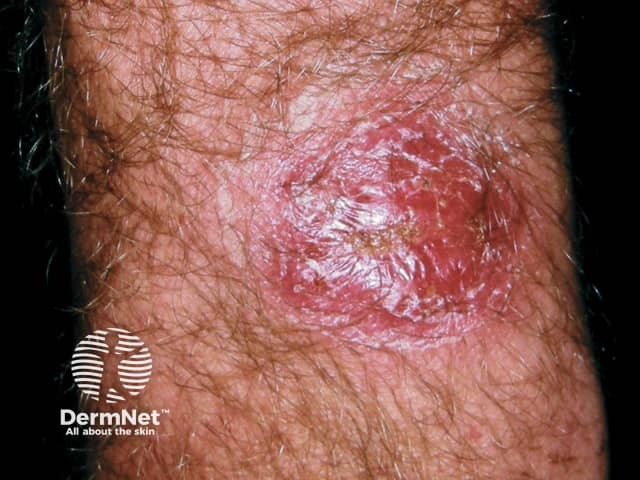
Kerion - inflammatory tinea corporis
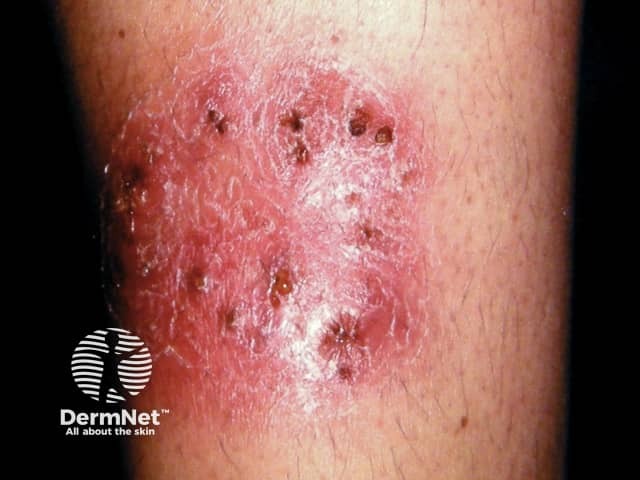
Majocchi granuloma - invasive tinea corporis
Tinea incognito
Tinea corporis is contagious, spreading elsewhere on the skin and to others.
Immunosuppressed patients, such as those with HIV/AIDS, can present with disseminated infection.
Chronic dermatophytosis is T. rubrum infection of at least four body sites following a prolonged fluctuating course and recurrence despite treatment.
Dermatophytide reactions are an allergic rash at a distant site caused by an inflammatory fungal infection.
Secondary bacterial infection with Staph aureus is common in children with atopic dermatitis and tinea corporis.
Tinea corporis should be considered in the setting of a solitary patch or asymmetrical rash and confirmed on mycology to determine the likely source.
Examination should include the entire skin surface, including the scalp and nails, for other sites of involvement.
Dermoscopy may assist the clinical diagnosis with features of erythema, white scaling, peripheral or patchy distribution of blood vessels, tiny follicular papules, brown spots surrounded by white-yellow rings, and wavy or broken hairs.
Skin scrapings taken from the scaly lesion edge and mounted in 10–20% potassium hydroxide can be examined under a light microscope for hyphae and spores. Fungal culture of the skin scrapings provides identification of the causative organism (see Laboratory tests for fungal infection).
Tinea corporis is sometimes diagnosed on skin biopsy, and characteristic histology changes are seen (see Tinea corporis pathology). Histology is typically required for the diagnosis of Majocchi granuloma.
The differential diagnosis for tinea corporis can include:
Skin should be kept clean and dried thoroughly. Loose-fitting light clothing is recommended in hot humid climates. Avoid close contact with infected individuals and the sharing of fomites. Examination of household members and pets for the source of infection and appropriate treatment reduces the risk of re-infection.
Localised tinea corporis may respond to topical antifungal medications such as imidazoles and terbinafine. Application needs to include an adequate margin around the lesion and a prolonged course continuing for at least 1–2 weeks after the visible rash has cleared. However, recurrence is common.
Oral antifungal treatment is usually required if tinea corporis is involving a hair-bearing site, is extensive, or has failed to clear with topical antifungals. Systemic therapy is also required for Majocchi granuloma and tinea imbricate. Recommended oral agents are terbinafine and itraconazole.
With appropriate treatment and good patient compliance, tinea corporis can be cured. However, recurrence or re-infection can occur if treatment has stopped too soon, or the source of infection has not been identified and treated.