Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Infections Diagnosis and testing
Last Reviewed: March, 2024
Author: Hon A/Prof Amanda Oakley, Dermatologist, New Zealand (2003); updated by Dr Ian Coulson, Dermatologist, United Kingdom (2024).
Edited by the DermNet content department.
Introduction
Specimen collection
Direct microscopy
Culture
Blood tests
Molecular biology techniques
Skin, hair and nail tissue are collected for microscopy and culture (mycology) to establish or confirm the diagnosis of a fungal infection.
Exposing the site to long-wavelength ultraviolet radiation (Wood lamp) can help identify some fungal infections of hair (tinea capitis) because the infected hair fluoresces green.
Specimens for fungal microscopy and culture are transported to the laboratory in a sterile container or a black paper envelope. They include:
A swab should also be taken from pustules in case of secondary bacterial infection.
The material is examined by microscopy by one or more of these methods:
Microscopy can identify a dermatophyte by the presence of:
Fungal elements are sometimes difficult to find, especially if the tissue is very inflamed, so a negative result does not rule out fungal infection.
A yeast infection can be identified by the presence of:
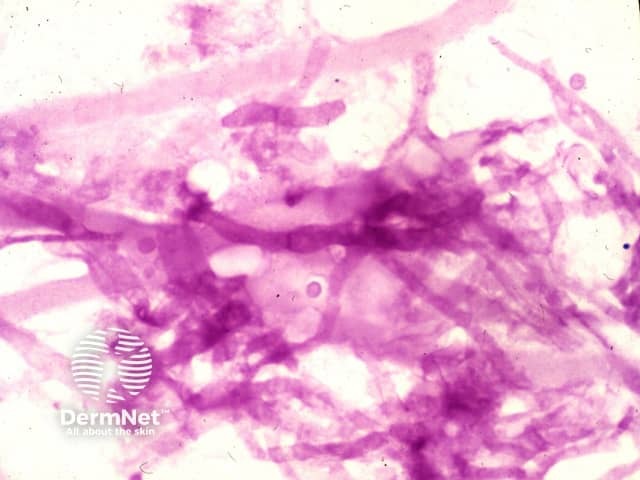
PAS stain of aspergillus seen in a skin biopsy
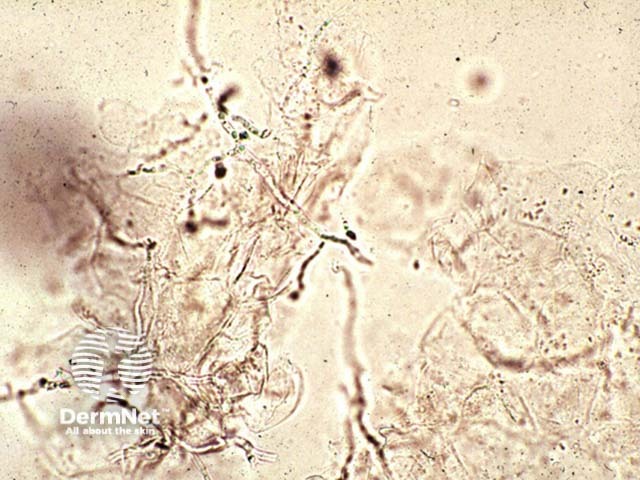
KOH of M. canis
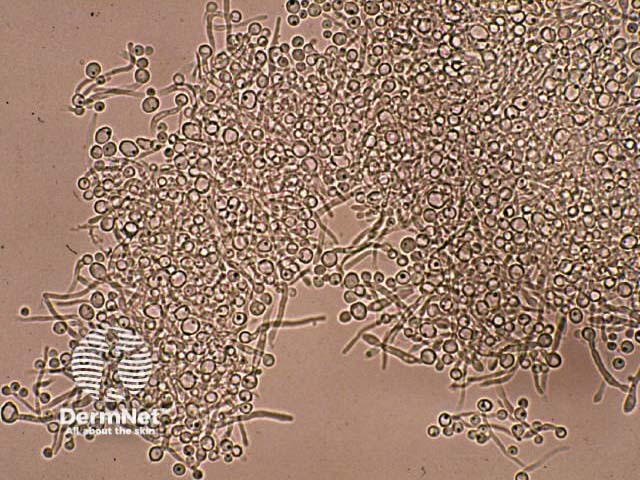
KOH of candida
Culture identifies which organism is responsible for the infection:
Growing the fungus in culture may take several weeks, incubated at 25–30ºC. The specimen is inoculated into a medium such as Sabouraud's dextrose agar containing cycloheximide and chloramphenicol. The cycloheximide is left out if a mould requires identification.
A negative culture may arise because:
The culture of yeasts and moulds may be due to harmless colonisation rather than infection; this is common in an underlying skin disease such as psoriasis.

Trichophyton rubrum culture on agar slope
Blood tests are not useful for the diagnosis of superficial fungal infections. In subcutaneous and systemic mycoses, several tests may be helpful.
Molecular testing by the PCR technique has become widespread in recent years and has a higher sensitivity than either culture or direct microscopy.
Results are often available in 24 hrs, and give fungal species identification that it useful both therapeutically and epidemiologically.