Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Kate Quirke, Senior House Officer, Rotorua Hospital, New Zealand. Copy edited by Gus Mitchell. March 2022. Previous author: Hon A/Prof Amanda Oakley, Dermatologist, Waikato Hospital, New Zealand.
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment and prevention
Outcome
Impetigo is a common, superficial, highly contagious bacterial skin infection characterised by pustules and honey-coloured crusted erosions.
It affects the superficial layers of the epidermis and is typically caused by Staphylococcus aureus and Streptococcus pyogenes (Group A beta – haemolytic streptococci (GABHS)). It can be classified into non-bullous (also known as ‘school sores’) and bullous impetigo. Ecthyma is a deep form of impetigo causing deeper erosions of the skin into the dermis.
Secondary infection of wounds or other skin lesions with the same pathogens is called ‘impetiginisation’.
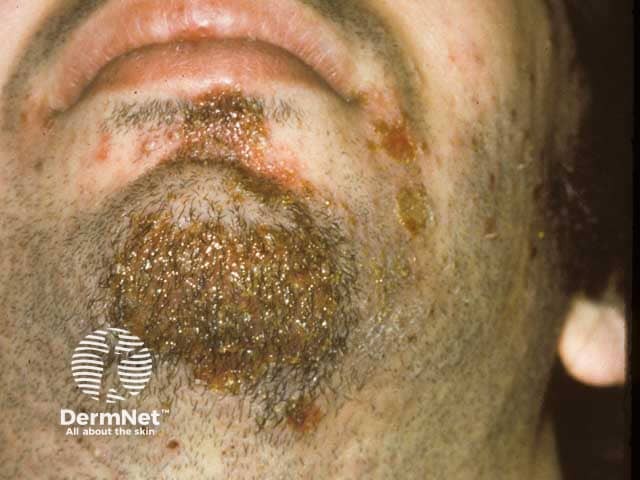
Honey-coloured crusts on the chin in impetigo
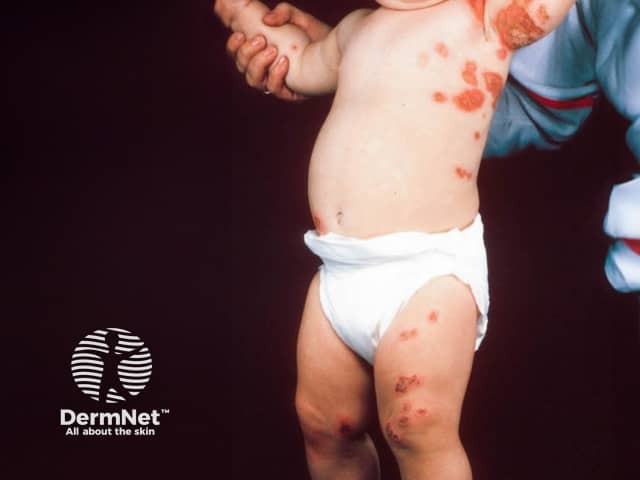
'Kissing lesions' on both sides of the axilla in impetigo
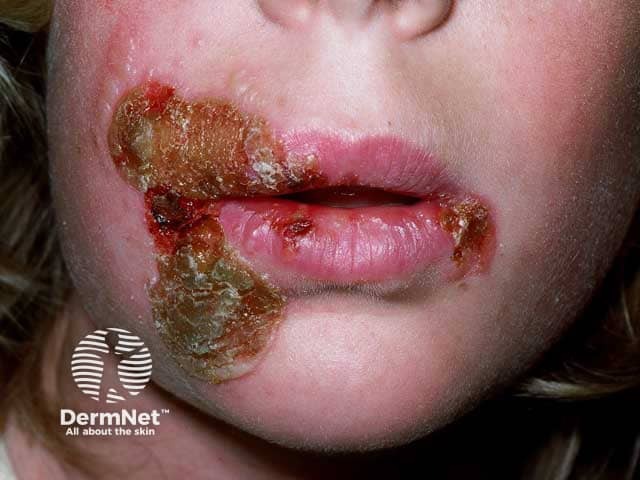
Perioral honey-coloured crusts in impetigo
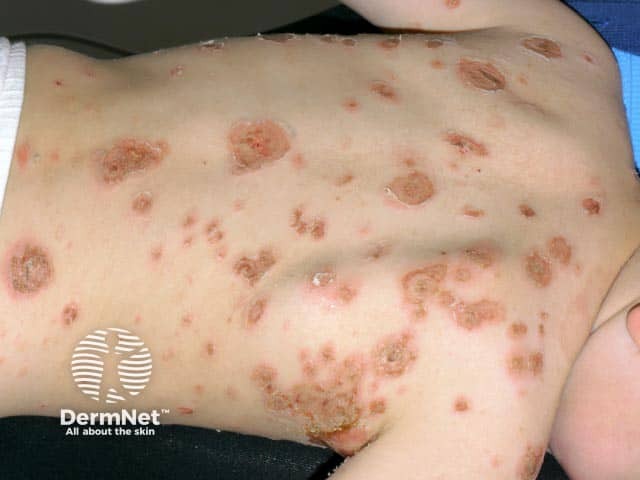
Widespread bullous impetigo over the back
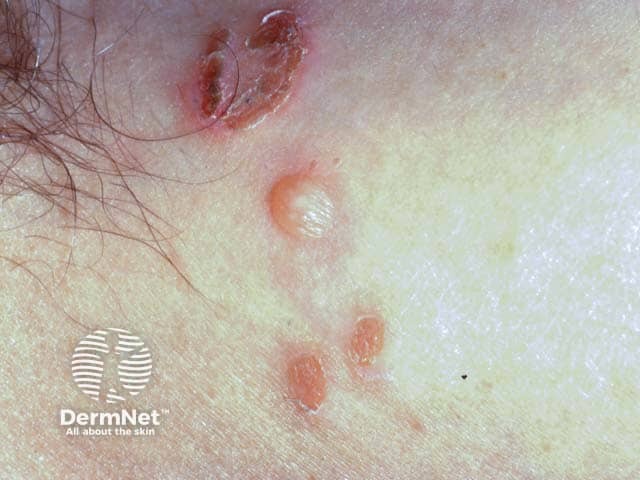
An intact blister and erosions in bullous impetigo
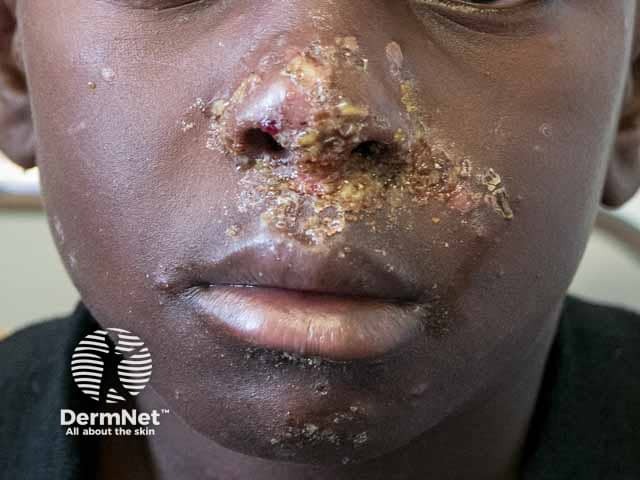
Honey-coloured crusted lesions in facial impetigo
For more images of impetigo, click here.
Impetigo is most common in young children but can occur at any age. It is usually transmitted through direct contact.
Risk factors which may predispose an individual to impetigo include:
Impetigo is caused by Staphylococcus aureus, and less commonly Streptococcus pyogenes.
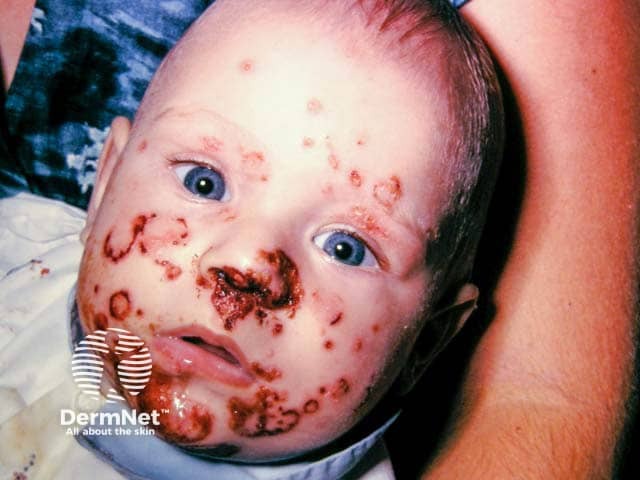
Crusted weepy lesions in facial impetigo
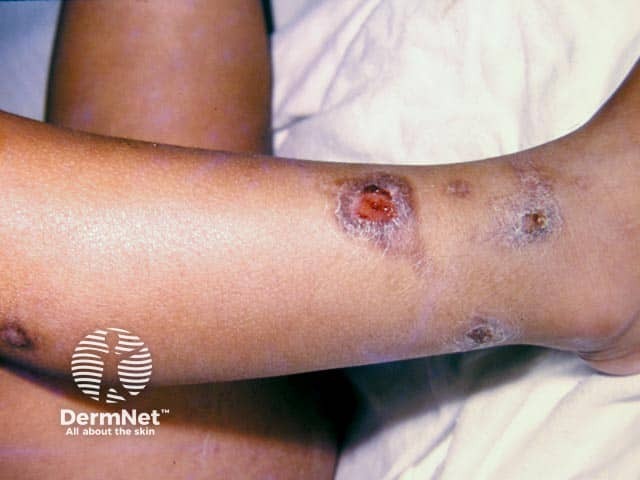
Impetigo on the leg
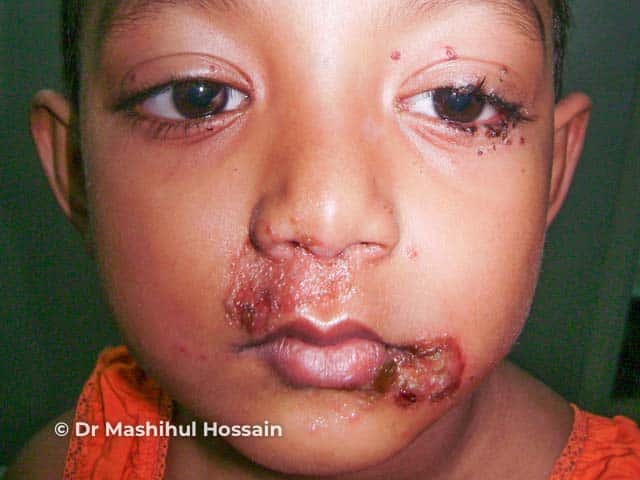
Facial impetigo
The initial erythematous macule in non-bullous impetigo may be more difficult to see on darker skin tones.
Impetigo is usually self-limiting without serious complications. Without treatment, impetigo usually heals in 2–3 weeks; with treatment lesions resolve within 10 days.
Postinflammatory hypopigmentation or hyperpigmentation may occur but scarring is uncommon.