Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amy Stanway, Department of Dermatology, Waikato Hospital, Hamilton, New Zealand, 2001. Reviewed and updated by Dr Jannet Gomez, Postgraduate Student in Clinical Dermatology, Queen Mary University London, United Kingdom; Chief Editor, Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, July 2016.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Management
Cellulitis is a common bacterial skin infection of the lower dermis and subcutaneous tissue. It results in a localised area of red, painful, swollen skin, and systemic symptoms. Left untreated, cellulitis can be life-threatening.
Similar symptoms are experienced with the more superficial infection, erysipelas, so cellulitis and erysipelas are often considered together.
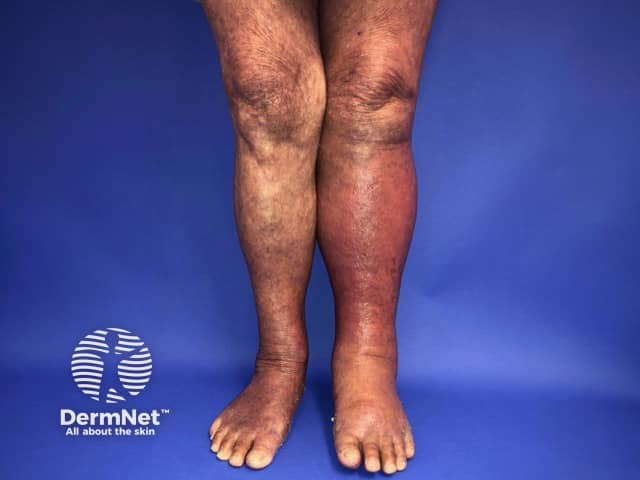
Cellulitis of the left leg

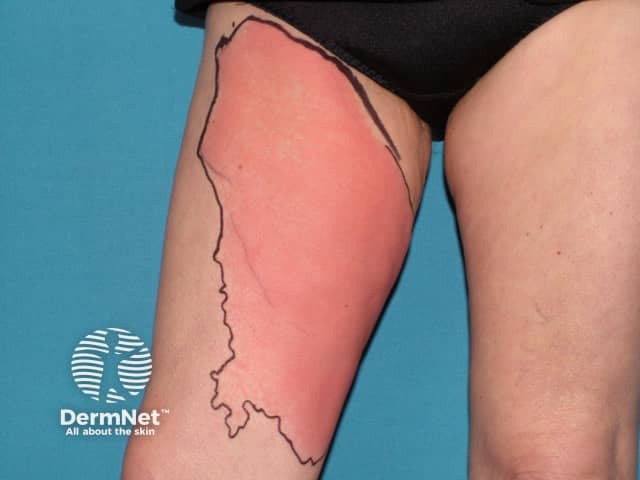
Cellulitis affects people of all ages and races.
Risk factors for cellulitis include:
Many people falsely attribute an episode of cellulitis to an unseen spider bite. Documented spider bites have not led to cellulitis.
The most common bacteria causing cellulitis are Streptococcus pyogenes (two-thirds of cases) and Staphylococcus aureus (one third). Rare causes of cellulitis include:
Other forms of skin injury that may increase bacterial exposure and cellulitis infection include surgical wounds and insect bites.
Cellulitis is generally not contagious as it affects the deeper layers of the skin.
Cellulitis can affect any site, but most often affects the limbs
The first sign of the illness is often feeling unwell, with fever, chills and shakes (rigors). This is due to bacteria in the bloodstream (bacteraemia). Systemic symptoms are soon followed by the development of a localised area of painful, red, swollen skin. Other signs include:
Cellulitis may be associated with lymphangitis and lymphadenitis, which are due to bacteria within lymph vessels and local lymph glands. A red line tracks from the site of infection to nearby tender, swollen lymph glands.
After successful treatment, the skin may flake or peel off as it heals. This can be itchy.
Severe or rapidly progressive cellulitis may lead to complications that require prompt treatment:
Sepsis is recognised by fever, malaise, loss of appetite, nausea, lethargy, headache, aching muscles and joints. The serious infection leads to hypotension (low blood pressure, collapse), reduced capillary circulation, heart failure, diarrhoea, gastrointestinal bleeding, renal failure and loss of consciousness.
The diagnosis of cellulitis is primarily based on clinical features including a physical exam. Investigations may reveal:
Imaging may be performed. For example:
Cellulitis is often diagnosed when another inflammatory skin disease is actually responsible for redness and swelling. Conditions causing 'pseudocellulitis' include:
Cellulitis is potentially serious. The patient should rest and elevate the affected limb. The edge of the involved area of swelling should be marked to monitor progression/regression of the infection.
Knowledge of local organisms and resistance patterns is essential in selecting appropriate antibiotics. The management of cellulitis is becoming more complicated due to rising rates of methicillin-resistant Staphylococcus aureus (MRSA) and macrolide- or erythromycin-resistant Streptococcus pyogenes.
If there are no signs of systemic illness or extensive infection, patients with mild cellulitis can be treated with oral antibiotics at home, for a minimum of 5–10 days. In some cases, antibiotics are continued until all signs of infection have cleared (redness, pain and swelling), sometimes for several months. Treatment should also include:
More severe cellulitis and systemic symptoms should be treated with fluids, intravenous antibiotics and oxygen. The choice of antibiotics depends on local protocols based on prevalent organisms and their resistance patterns and may be altered according to culture/susceptibility reports.
Sometimes oral probenecid is added to maintain antibiotic levels in the blood.
Treatment may be switched to oral antibiotics when the fever has settled, cellulitis has regressed, and CRP is reducing.
Patients with recurrent cellulitis should:
Patients with 2 or more episodes of cellulitis may benefit from chronic suppressive antibiotic treatment with low-dose penicillin V or erythromycin, for one to two years.