Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Original page created in 2003. Updated by Dr Thomas Stewart, General Practitioner, Sydney, Australia. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. April 2018.
Introduction
Causes
Demographics
Clinical features
Diagnosis
Differential diagnoses
Treatment
Prevention
Tinea pedis is a foot infection due to a dermatophyte fungus. It is the most common dermatophyte infection and is particularly prevalent in hot, tropical, urban environments.
The three most common dermatophyte fungi causing tinea pedis are:
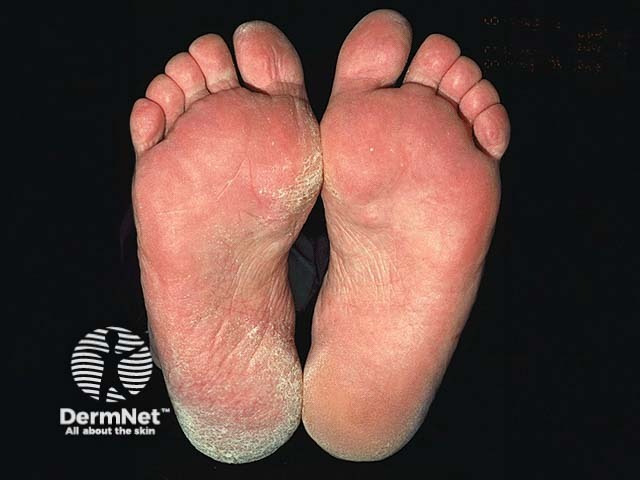
Moccasin tinea pedis
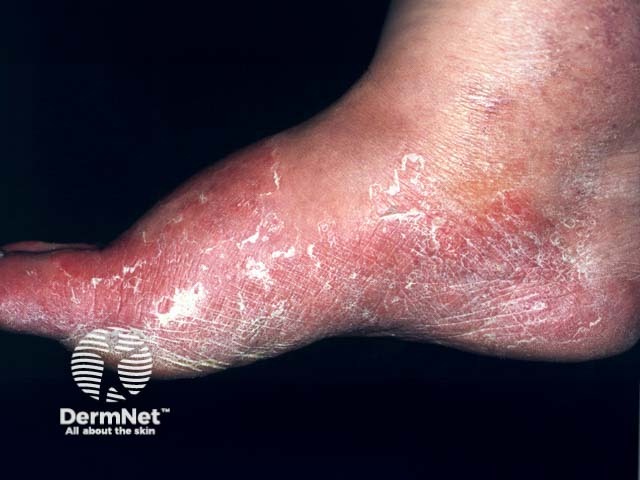
Tinea pedis
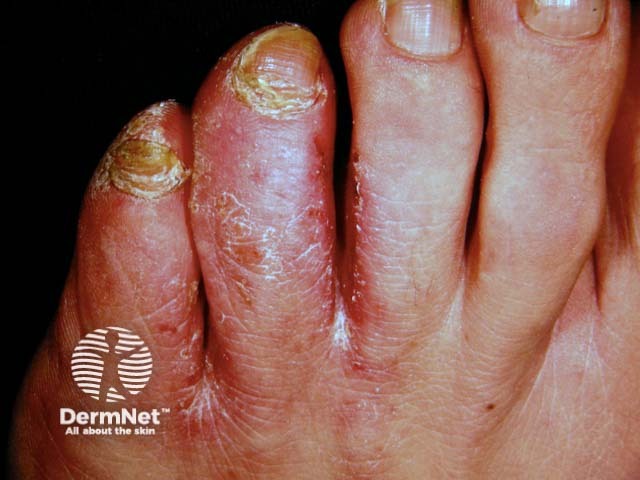
Tinea pedis
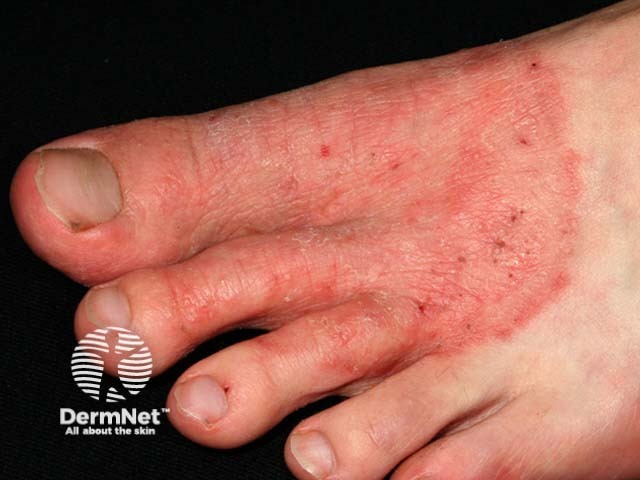
Tinea pedis
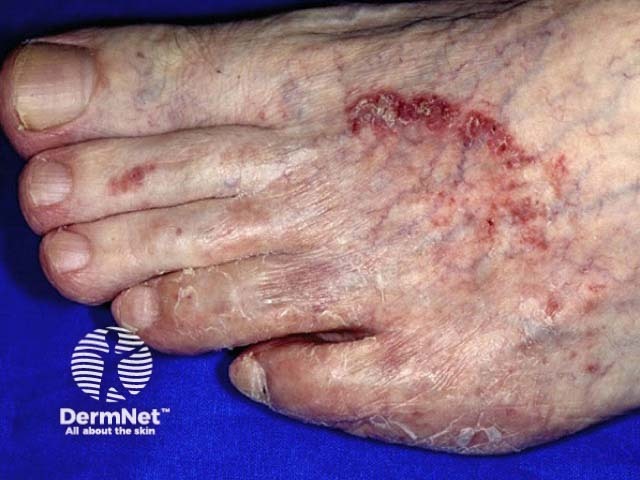
Tinea pedis
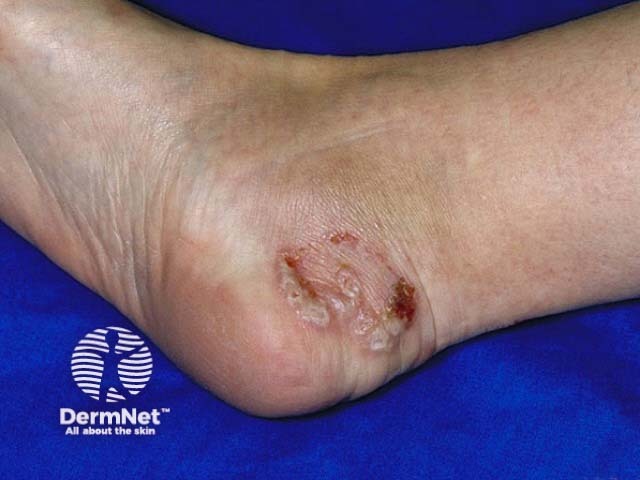
Tinea pedis
See more images of tinea pedis ...
Tinea pedis usually occurs in males and adolescents/young adults, but can also affect females, children and older people. Infection is usually acquired by direct contact with the causative organism, for example using a shared towel, or by walking barefoot in a public change room.
Other risk factors include:
Tinea pedis tends to be asymmetrical, and may be unilateral. It usually presents in one of three ways:
It can also uncommonly cause oozing and ulceration between the toes (ulcerative type), or pustules (these are more common in tinea pedis due to T. interdigitale than that due to T. rubrum).
The diagnosis of tinea pedis can be made clinically in most cases, based on the characteristic clinical features. Other typical sites, such as toenails, groin, and palms of the hands, should be examined for fungal infection, which may support a diagnosis of tinea pedis.
Diagnosis is confirmed by skin scrapings, which are sent for microscopy in potassium hydroxide (when segmented hyphae may be observed) and culture (mycology). Culture may not be necessary if typical fungal elements are observed on microscopy.
The differential diagnosis of tinea pedis includes:
These inflammatory disorders are more likely to be symmetrical and bilateral. Mycology is negative.
General measures should be first-line, including meticulous drying of feet, especially between the toes, avoidance of occlusive footwear, and the use of barrier protection (sandals) in communal facilities. Finger socks can help separate the toes, reducing humidity and help clear infection.
Topical antifungal therapy once or twice daily is usually sufficient. These include azoles, allylamines, butenafine, ciclopirox, and tolnaftate. A typical course is 2 to 4 weeks, but single dose regimes can be successful for mild infection [1,2].
For those who do not respond to topical therapy, an oral antifungal agent may be needed for a few weeks. These include:
Patients with the hyperkeratotic variant of tinea pedis may benefit from the addition of a topical keratolytic cream containing salicylic acid or urea [5].
To minimise recurrence of tinea pedis:
If treatment of tinea pedis is unsuccessful, consider reinfection, coexistent untreated fungal nail infection, reinfection due to untreated family member, or an alternative diagnosis.