Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: April, 2025
Authors: Dr Tatiana Ninkov, Dermatology Resident; Dr Rachael Foster, Dermatologist, Sir Charles Gairdner Hospital, Perth, Australia (2025)
Previous contributors: Hon Assoc Prof Amanda Oakley, Dermatologist, NZ (2014)
Peer reviewed by: Dr Zoe Lee, Flinders Medical Centre, Australia (2025)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Causes
Demographics
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Palmoplantar pustulosis is a benign, chronic, and often relapsing sterile pustular dermatosis affecting the palms and soles. It may occur in patients with psoriasis, however it likely represents a distinct clinical entity. It responds less reliably to biologic treatments effective in psoriasis.
A variant of palmoplantar pustulosis affecting the tips of the digits is called acrodermatitis continua of Hallopeau or acropustulosis.
The exact cause of palmoplantar pustulosis remains unknown. However, environmental factors such as smoking, manual or repetitive trauma, irritants, and friction have been associated with this condition. Aside from these factors, several theories have also been proposed:
Specific chemotactic factors may also contribute or propagate inflammation including increased expression of IL8 and IL17. Increased detection of tumour necrosis factor-alpha (TNF-alpha) and IL-17. IL-22 and interferon-gamma have also been detected. Complement pathway activation has also been noted.
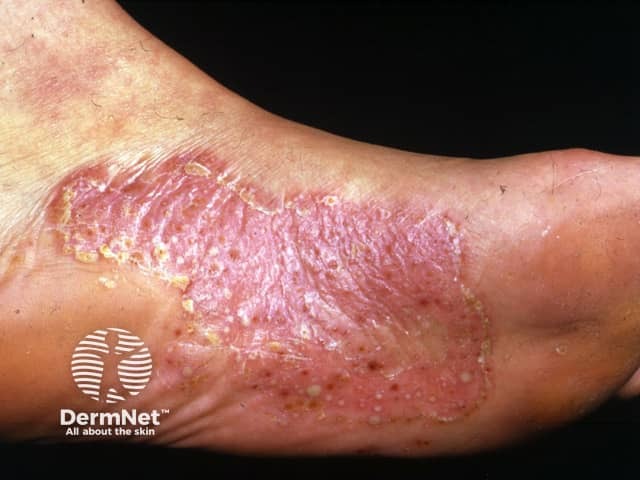
Pustules and rusty dots in a scaly plaque typical of PPP
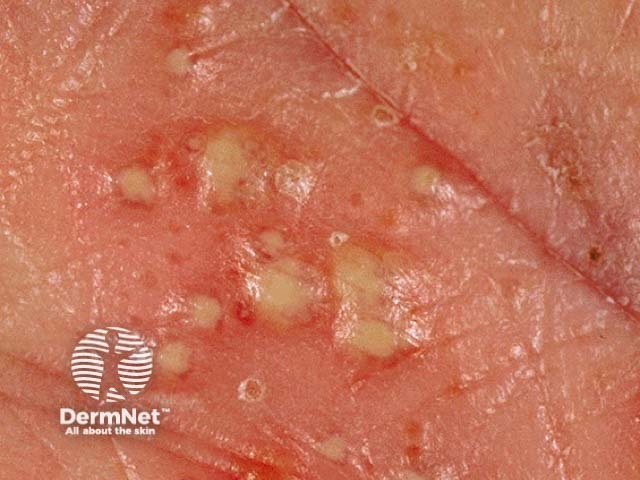
Pustules on the palm due to PPP
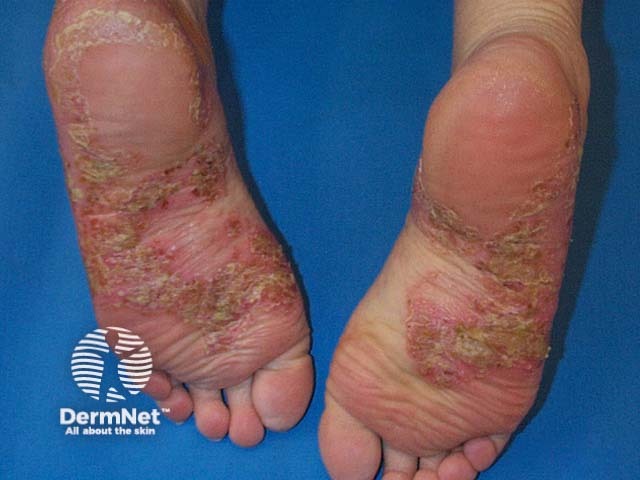
Typical lesions of PPP on the soles - redness, scale, pustules, and rusty red dots
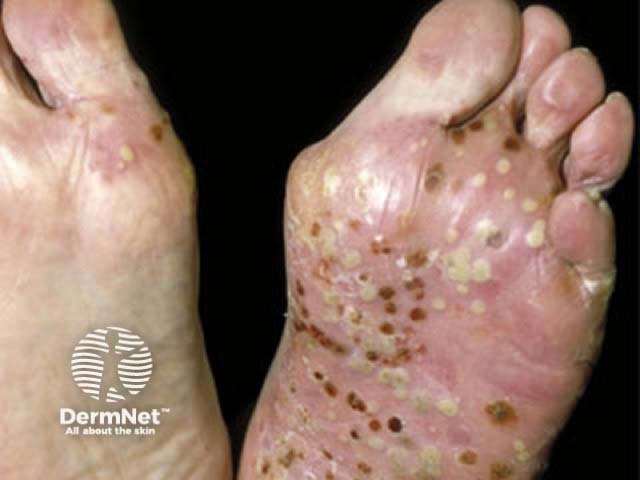
Florid pustules on the feet due to PPP
Palmoplantar pustulosis commonly presents between the ages of 20 and 60 years, with a predilection for females (female-to-male ratio 4:1).
The majority of patients with palmoplantar pustulosis are cigarette smokers, with 70-90% of patients being current or former smokers. Smoking is also a disease-aggravating factor. It is thought that activated nicotine receptors in the sweat glands stimulate an inflammatory process.
Several associated conditions have been determined:
Other described causes include:
Palmoplantar pustulosis usually presents as crops of sterile pustules localised to the palms and soles. These pustules are 1-10mm in size, often admixed with yellow-brown macules and/or scaly, erythematous plaques. Lichenification and desquamation are also commonly seen.
Pustules are more commonly noted on the thenar and hypothenar eminences and central palm. As well as the instep, medial and lateral borders of the foot and the sides or back of the heel.
Patients complain of varying levels of pruritus, however a more common complaint is of a ‘burning’ sensation. Lesions may also develop into painful fissures, and psoriatic nail changes may be present.
Palmoplantar pustulosis varies in severity and is often chronic, due to its difficult-to-treat nature. Slow spread or extension may occur. Rarely, pustules form snake-like patterns — termed serpiginous palmoplantar pustulosis.
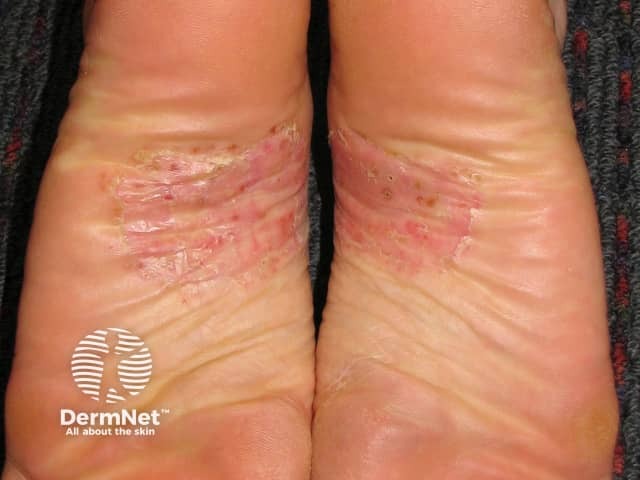
Palmoplantar pustulosis
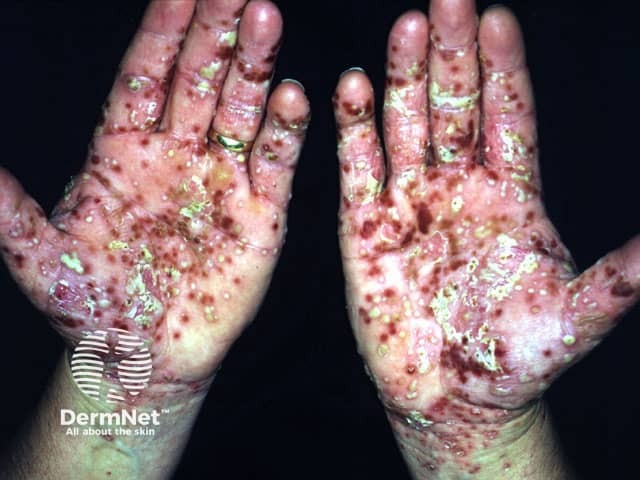
Palmoplantar pustulosis
Palmoplantar pustulosis is generally a clinical diagnosis. Investigations may be helpful for ruling out differential diagnoses or excluding possible complications. This includes:
Management of palmoplantar pustulosis is often difficult and the condition may be refractory to treatment. Options are discussed below.
The disease course of palmoplantar pustulosis is usually prolonged, unpredictable, and can be refractory to treatment. Even if remission is achieved, relapse is common.