Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Reactions Autoimmune/autoinflammatory
Author: Brian Wu, MD candidate, Keck School of Medicine, Los Angeles, USA. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editor: Maria McGivern. June 2017.
Introduction - psoriasis
Introduction
Demographics
Causes
Clinical features
Diagnosis
Treatment
Outcome
Psoriasis is a common chronic skin condition characterised by symmetrically distributed, well-defined scaly plaques. The most common type of psoriasis is chronic plaque psoriasis, which often starts in early adult life.
In some people, psoriasis is drug-induced or drug-aggravated.
These forms of psoriasis differ from psoriasiform drug eruption, a group of papular drug eruptions characterised histologically by epidermal hyperplasia and hypergranulosis.
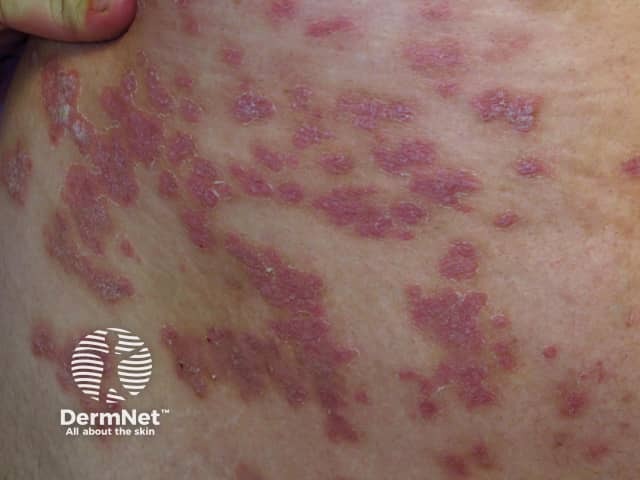
Psoriasis induced by lithium
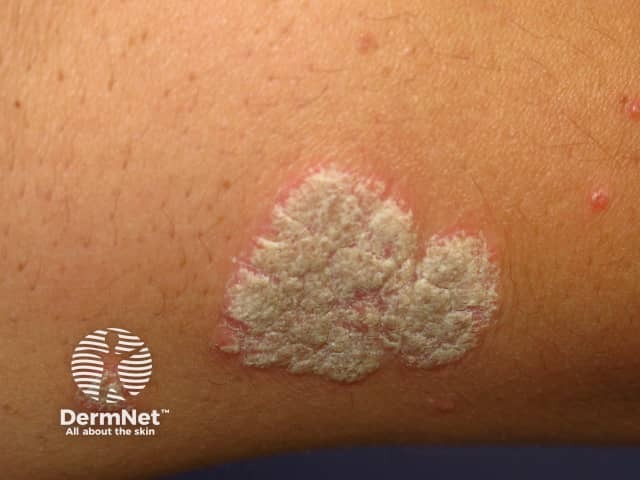
Psoriasis induced by lithium
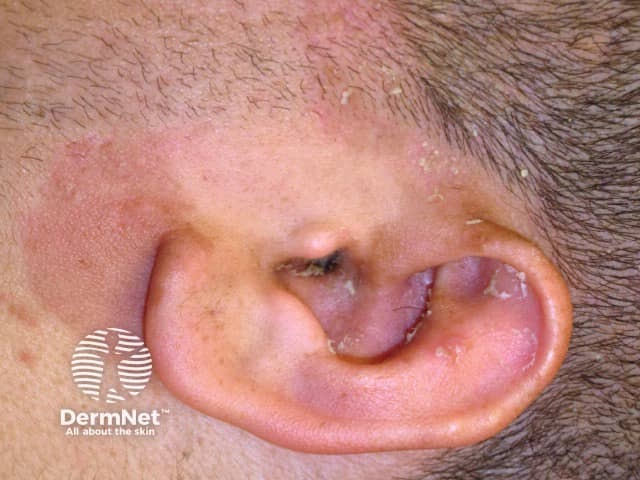
Psoriasis induced by lithium
As with psoriasis that is not induced by a drug, drug-induced psoriasis occurs more frequently in patients with a history of:
Other risk factors for psoriasis include:
The most common drugs to induce or aggravate psoriasis are:
Other common triggers for psoriatic exacerbations include trauma, sunburn, streptococcal infection, human immunodeficiency virus (HIV) infection and emotional stress.
Immunotherapy-related psoriasiform reactions can also occur.
Drug-induced or drug-aggravated psoriasis may induce:
Acute generalised exanthematous pustulosis (AGEP) is a severe drug-induced eruption that closely resembles generalised pustular psoriasis.
Palmoplantar pustulosis can also be drug-induced, often by tumour necrosis factor inhibitors. Although closely related, palmoplantar pustulosis is no longer classified as a type of psoriasis. It nearly always occurs in smokers.
Diagnosis of drug-induced psoriasis can be challenging when patients are on multiple medications. The onset of psoriatic symptoms can be months or years after the drug has been started. Careful patient history is essential in any patient that presents with new-onset psoriasis and must include their current medications. The possibility of other triggers for psoriasis, apart from drugs, should also be taken into consideration.
The standard of care in the case of drug-induced psoriasis is to discontinue the offending drug. However, this is not always possible; for example, in a patient with severe depression that is well controlled by lithium where other options have been ineffective or contraindicated.
Treatments for psoriasis include:
While some cases of drug-induced psoriasis can resolve within weeks of stopping the causative medicine, in other cases, it can take much longer to resolve or not resolve completely.