Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Piera Neill, The University of Auckland; Honorary Associate Professor Paul Jarrett, Dermatologist, Middlemore Hospital and Department of Medicine, The University of Auckland, New Zealand (2022)
Previous contributors: Hon A/Prof Amanda Oakley, Dermatologist (2014); Vanessa Ngan (2003)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction Demographics Causes Clinical features Variation in skin types Complications Diagnosis Differential diagnoses Treatment Outcome
Generalised pustular psoriasis (GPP) is a rare, severe form of pustular psoriasis. It is characterised by recurrent flares of widespread sterile pustules with erythematous, painful skin. GPP can be associated with systemic inflammation including fevers and/or hepatic, gastrointestinal, musculoskeletal, renal, or pulmonary involvement.
It is also known as von Zumbusch psoriasis.
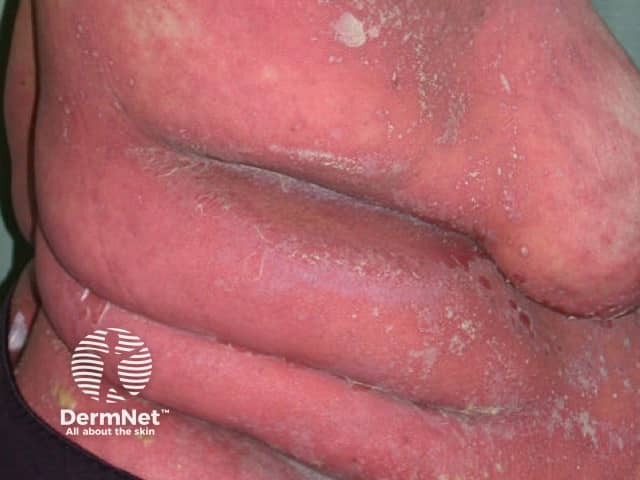
Generalised pustular psoriasis
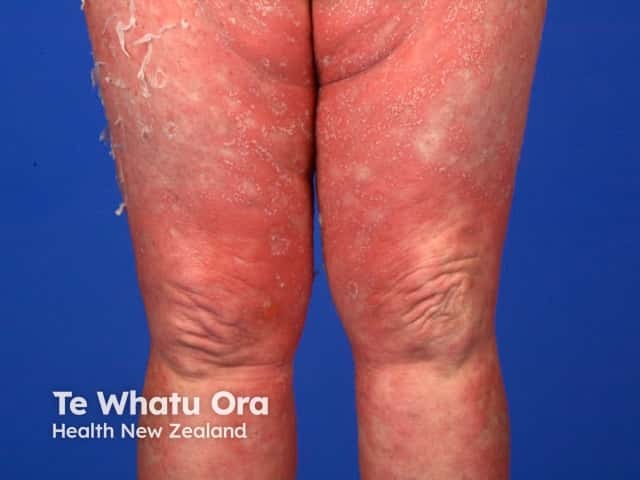
Generalised pustular psoriasis
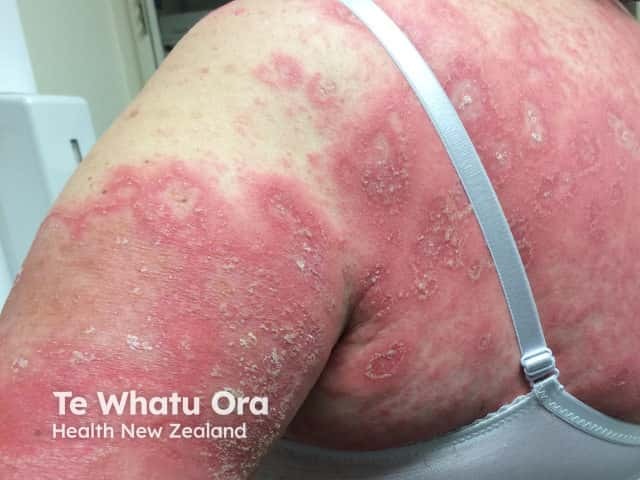
Generalised pustular psoriasis
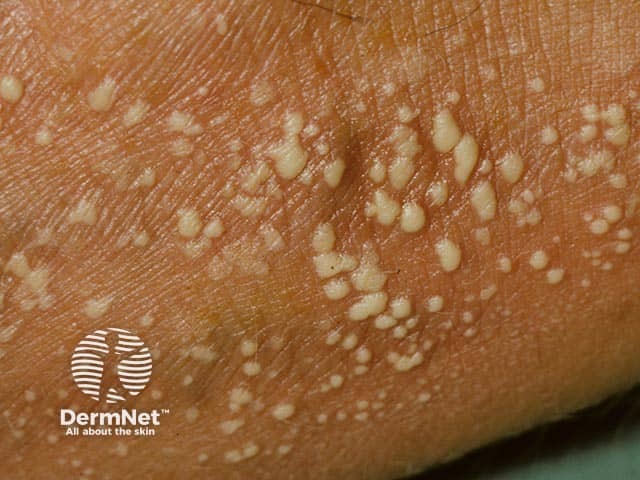
Pustular psoriasis on a limb in skin of colour
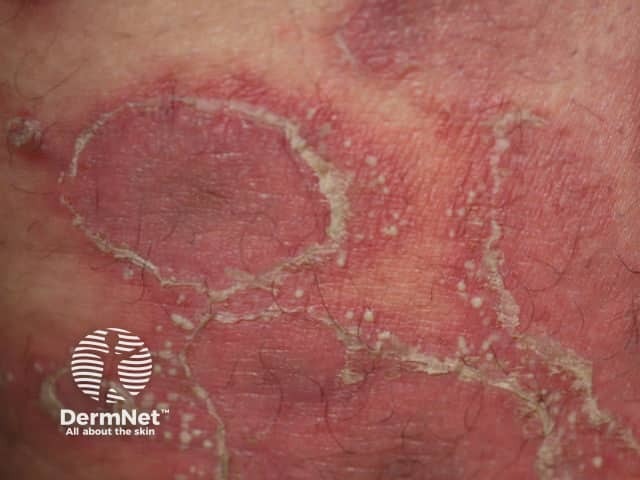
Generalised pustular psoriasis
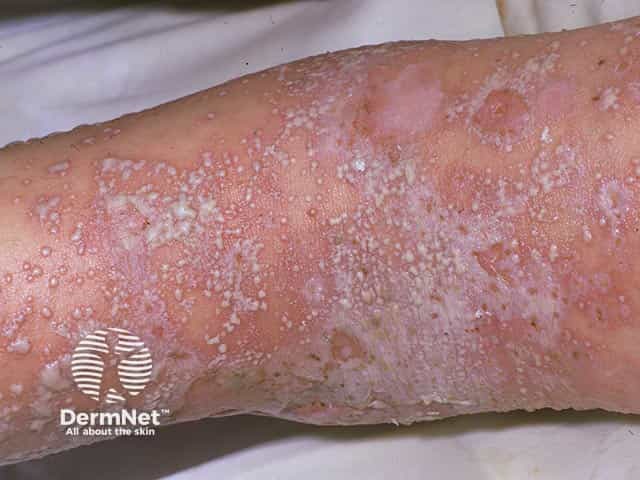
Superficial pustules in generalised pustular psoriasis
GPP can appear in any age group, although is most common in adults between 40–50 years old and is unusual in children. The age of onset is often earlier in patients with a family history of psoriasis, or with a homozygous interleukin 36 (IL-36) receptor antagonist (IL36RN) gene mutation.
Females are generally more likely to be affected, although, for paediatric onset between 3–16 years of age, a male predominance has been reported.
GPP can also affect pregnant women, which is termed impetigo herpetiformis, and is associated with increased maternal and fetal morbidity.
Although GPP is distinct from plaque psoriasis, the two conditions are strongly associated with one another, making concurrent or previous plaque psoriasis a significant risk factor for developing GPP.
The exact pathogenic mechanisms are not fully established. However, GPP is associated with a combination of genetic and environmental risk factors.
Several genetic mutations are associated with GPP, including homozygous and heterozygous mutations in genes involved in the regulation of immune and inflammatory pathways, such as:
Genetic screening for GPP may potentially be available in future.
Use of (or tapering/stopping) various medications may be associated with GPP, such as:
The varying clinical presentation of GPP between differing skin types is not well documented, mainly due to the rarity of the disease. Erythema can be under-recognised in skin of colour, and therefore the severity of inflammation can be underestimated.
Complications of acute skin failure include:
Other potential complications of GPP:
Such complications can be fatal. Death can result from cardiorespiratory failure during the acute eruptive phase of generalised pustular psoriasis, so it is essential to treat it as early as possible. Older patients are at particularly high risk.
Maternal GPP can result in foetal abnormalities, preterm birth, placental insufficiency, and neonatal death.
GPP can be a diagnostic challenge due to its rarity, its heterogeneous cutaneous and extracutaneous symptomatology, its similarity to other conditions such as acute generalised exanthematous pustulosis, and the lack of standardised international diagnostic criteria.
According to the 2018 Japanese guidelines, a definitive diagnosis of GPP can be made in patients with all four of the following features:
GPP would be diagnosed if all four of the above features were present and would be suspected in patients with features 2 and 3.
Abnormal laboratory tests may include:
Skin biopsy may show:
Diagnostic criteria were also described in the 2017 European Rare and Severe Psoriasis Expert Network (ERASPEN) which can be found here.
GPP is severe, and complications can be life-threatening. It should be treated promptly and usually hospitalisation is needed. Intensive care support may be necessary.
GPP is an incurable condition, with an unpredictable and variable course.
Although treatment aims to prevent and reduce the frequency and duration of flares, most patients have recurrent disease. The time interval between flares ranges from weeks to years, and the severity of flares is also fluctuant. There may or may not be complete regression of lesions after flares, and symptoms have been reported to persist between flares in ~80% of cases.
Data on mortality rates are limited, but have been reported between 3–7%. Older patients likely have a poorer prognosis than younger patients due to comorbidities and systemic complications.