Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Esther Wang, Medical Student and Professor Dedee Murrell, Head, Department of Dermatology, St George Hospital, Sydney, Australia. A/Prof Amanda Oakley, Dermatologist, NZ 2018. Updated: Dr Musfira Shakeel, Salford Royal Foundation Trust, United Kingdom. Copy edited by Gus Mitchell. May 2022.
Introduction Demographics Clinical features Causes Differential diagnoses Diagnosis Treatment
IgA pemphigus (or immunoglobulin A pemphigus) is an autoimmune blistering disorder. It is also called intercellular IgA dermatosis among other names.
IgA pemphigus has two major subtypes:
However, a new classification describes five subtypes of IgA pemphigus; these being:
It has been associated with malignancies (multiple myeloma) and several chronic conditions (monoclonal IgA gammopathy, human immunodeficiency virus infection, Sjögren's syndrome, rheumatoid arthritis, and Crohn's disease).
IgA pemphigus is very rare. It can occur in any age group, but is more commonly seen in middle aged adults and may have a female predominance.
The clinical features of IgA pemphigus include blisters, pustules, erythema, erosions and vegetating lesions.
IgA pemphigus appears to favour the trunk, upper and lower extremities, axillae, and groin. Mucosal involvement is infrequent.
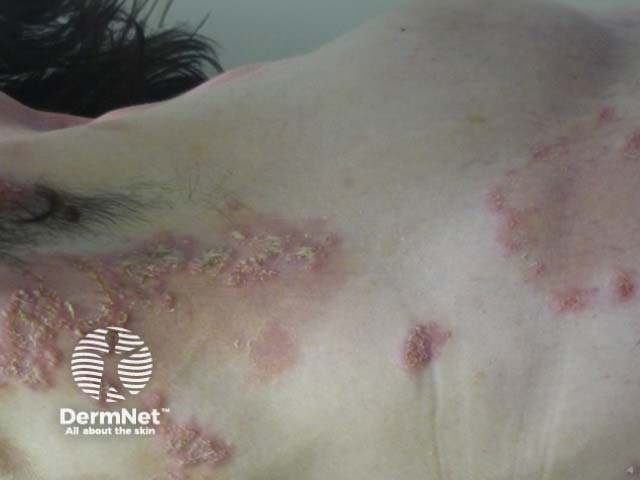
IgA pemphigus
The exact cause of IgA pemphigus is unclear.
Other conditions that should be considered in the differential diagnosis include:
A blistering autoimmune disease or autoinflammatory pustular disease may be suspected clinically from the clinical features, often after the eruption has failed to clear with antibiotics.
The diagnosis of IgA pemphigus requires a skin biopsy for histology and direct immunofluorescent testing.
Indirect immunofluorescence testing of serum can show IgA anti-keratinocyte cell-surface antibodies. Immunoglobulin G (IgG) anti-keratinocyte cell-surface antibodies have also been reported.
IgA pemphigus is usually treated with a combination of systemic steroids (anti-inflammatory effects) and dapsone which is thought to reduce neutrophil infiltration. This combination treatment is more effective than the use of steroids alone.
Since few cases of IgA pemphigus have been described, the most effective treatment is unknown. Other medications worth considering include:
In comparison to other forms of pemphigus, IgA pemphigus presents with a milder disease and carries a better prognosis. When managed appropriately, it mostly heals with no scarring.
Patients should be counselled about potential side effects of steroids and dapsone. IgA associated with other medical conditions should be managed in a multidisciplinary manner, hence it is important to thoroughly investigate potential underlying triggers/associations, especially in elderly patients.