Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2006. DermNet Update January 2021. Copy edited by Gus Mitchell.
Introduction Demographics Causes Clinical features Cutaneous features Rheumatoid arthritis-specific skin manifestations Cutaneous adverse effects of treatment Outcome
Rheumatoid arthritis is a chronic systemic inflammatory autoimmune disease characterised by a symmetric destructive polyarthritis and extra-articular manifestations including skin changes.
Skin changes of rheumatoid arthritis can be classified as:
Rheumatoid arthritis predominantly affects females (3:1) with an increased risk for those with a first-degree relative affected. The prevalence is estimated to be 1%. Rheumatoid arthritis affects all races. The peak age of onset is 35–50 years. Extra-articular involvement develops in approximately 40%, and skin changes in 30%.
Rheumatoid arthritis is multifactorial in origin. Although regarded as autoimmune with anti-citrullinated protein antibodies (ACPA) and rheumatoid factor (RF), genetic and environmental factors are also important in the pathogenesis. In ACPA-positive disease the most significant association is mapped to the HLA-DRB4 gene. ACPA are found in 60% of patients with rheumatoid arthritis (seropositive).
Rheumatoid arthritis initially affects the small joints, such as those in the hands, but in later stages can affect any joint. It presents as episodic flares of symmetrical synovitis (swelling, redness, pain of joints), morning stiffness, and enthesitis. Untreated, it progresses to irreversible joint destruction with loss of cartilage and bone.
Dermatoses may link with rheumatoid arthritis, but can also occur in association with other conditions.
These are skin conditions that occur only in association with rheumatoid arthritis.
Rheumatoid nodules are the most common extra-articular manifestation of rheumatoid arthritis, affecting 35–40% of patients, particularly Caucasian males. Approximately 90% are positive for rheumatoid factor. They present as solitary or multiple skin-coloured nodules on sites of recurrent pressure or trauma such as the forearm, elbow, fingers, heels, and back, and range in size up to several centimetres across.
Rheumatoid nodules are generally asymptomatic. Complications can include infection, ulceration, and gangrene. Histology is characteristic [see Rheumatoid nodule pathology].
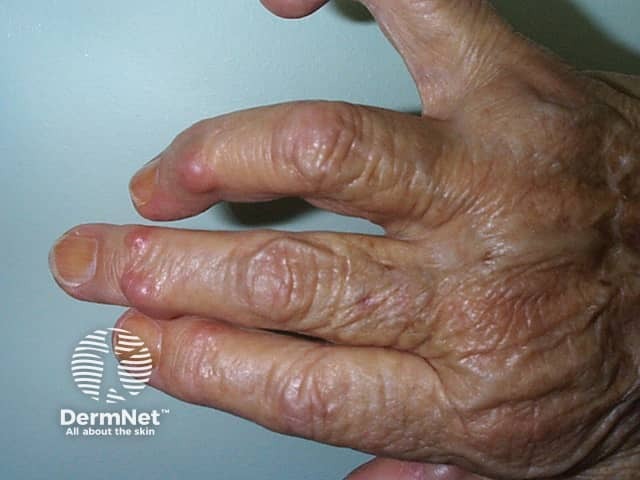
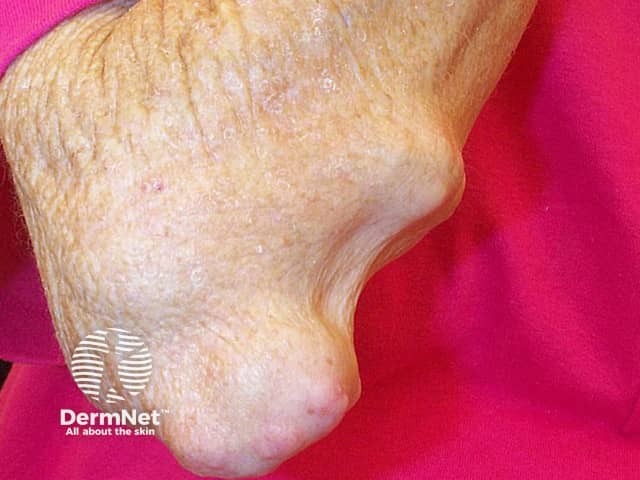
Rheumatoid nodules
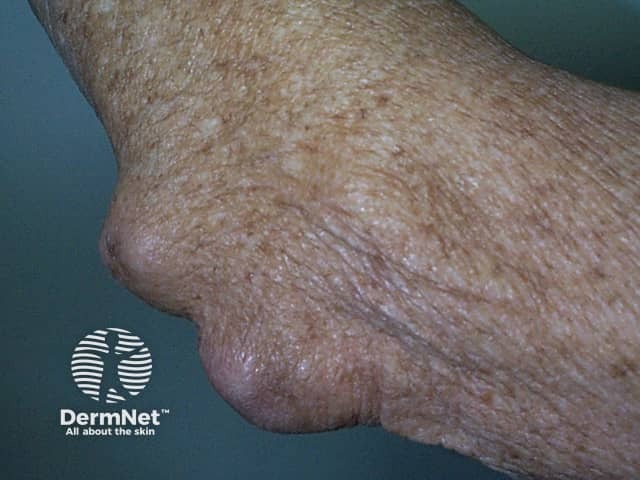
Rheumatoid nodulosis affects males 30–50 years of age with recurrent joint symptoms, hand and foot intraosseous cystic changes, mild or absent systemic symptoms of rheumatoid arthritis, positive rheumatoid factor, and a clinically benign course of multiple self-limiting rheumatoid nodules. Classic erosive rheumatoid arthritis can develop.
Accelerated nodulosis presents as a rapid onset of multiple small nodules particularly on the hands and feet in treated rheumatoid arthritis patients. It has been reported to affect 8–11% of patients taking methotrexate, and less commonly other treatments including leflunomide, azathioprine, and tumour necrosis factor inhibitors, particularly etanercept. Histology is the same as in rheumatoid nodules.
Rheumatoid vasculitis is an unusual complication of long-standing severe rheumatoid arthritis, typically involving small to medium sized vessels in any organ of the body. In the skin, rheumatoid vasculitis can present as palpable purpura, nailfold infarcts, digital necrosis, ulcers, and urticarial vasculitis. Biopsy shows a necrotising arteritis.
Bywaters lesions are a specific manifestation of rheumatoid vasculitis presenting as painless purpuric papules less than 1mm in diameter in the fingertip pulp or around the fingernails. They are not associated with systemic vasculitis.
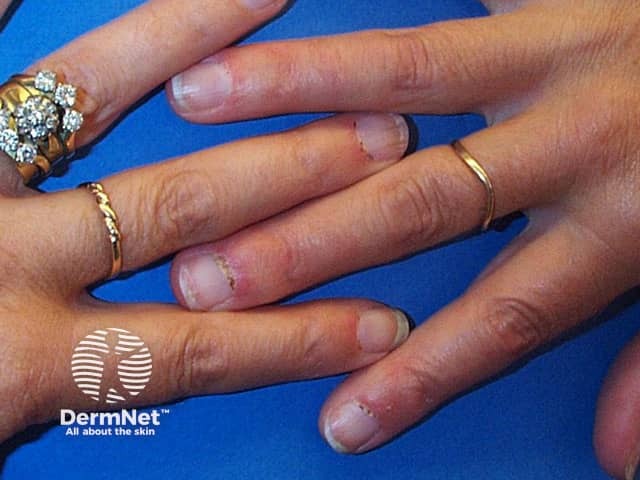
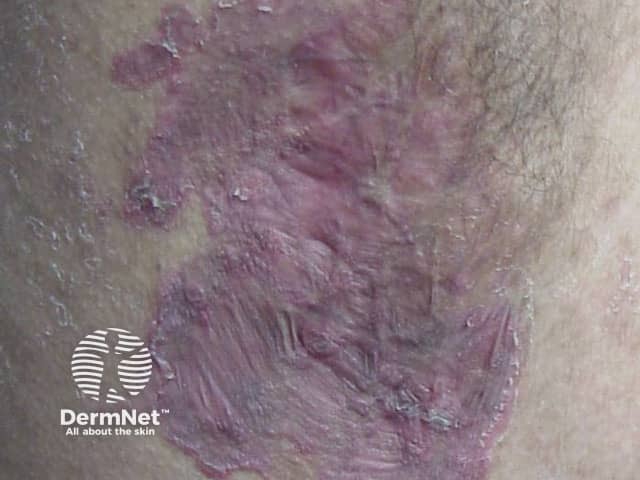
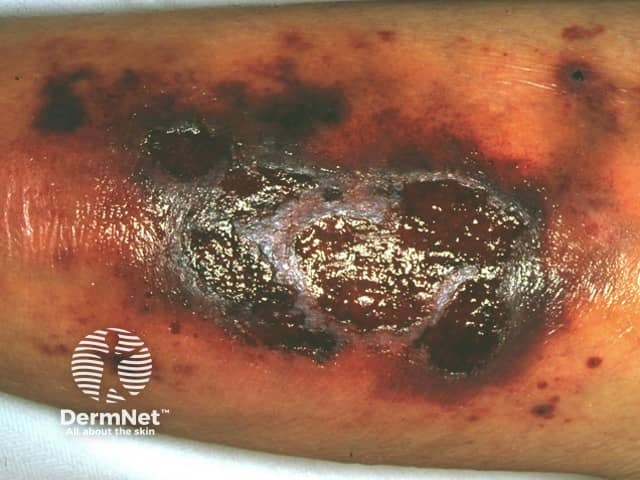
Necrotising vasculitis
Rheumatoid neutrophilic dermatitis is a rare extra-articular manifestation of severe long-standing seropositive rheumatoid arthritis presenting as a symmetrical asymptomatic eruption of erythematous papules, nodules, and plaques which may show an annular distribution on the extremities. Less commonly, lesions may blister or ulcerate. It is associated with a flare in arthritis activity, and resolves with treatment of the arthritis. Biopsy shows a neutrophilic leukocytoclastic dermatosis without vasculitis.
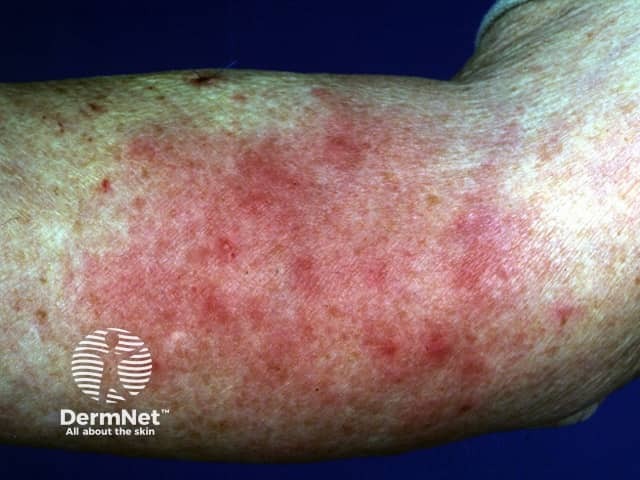
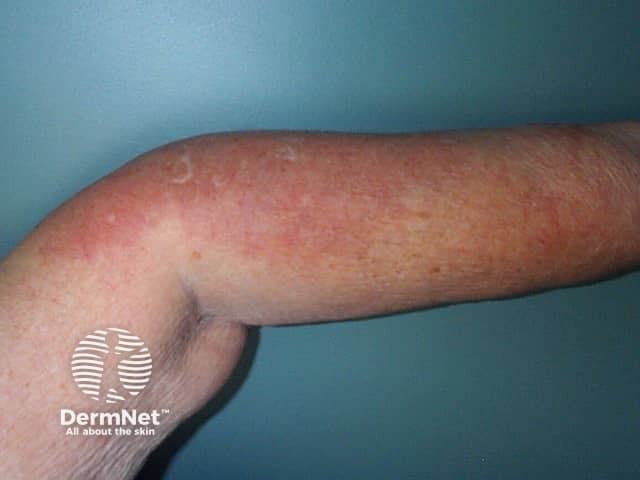
Neutrophilic dermatosis associated with rheumatoid arthritis
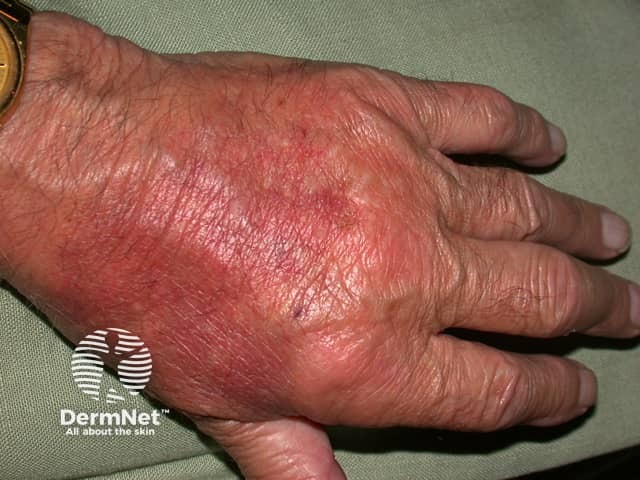
Neutrophilic dermatosis associated with rheumatoid arthritis
The treatment of rheumatoid arthritis can cause side effects involving the skin.
Disease modifying antirheumatic drugs (DMARD) used in the treatment of rheumatoid arthritis include methotrexate, azathioprine, leflunamide, ciclosporin, and hydroxychloroquine. Skin side effects are well documented.
There are many new and emerging treatments for rheumatoid arthritis including biological treatments, Janus kinase inhibitors, rituximab (anti-CD20), tocilizumab (anti-interleukin 6) with their associated cutaneous side effects. Tumour necrosis factor inhibitors are biologic agents used widely for treatment-resistant rheumatoid arthritis. Many cutaneous side effects have been reported with their use in rheumatoid arthritis including psoriasis, dermatitis, leukocytoclastic vasculitis, lichenoid drug eruptions, and non-infectious cutaneous granulomatous reactions, such as disseminated granuloma annulare, sarcoidosis-like lesions, and interstitial granulomatous dermatitis.
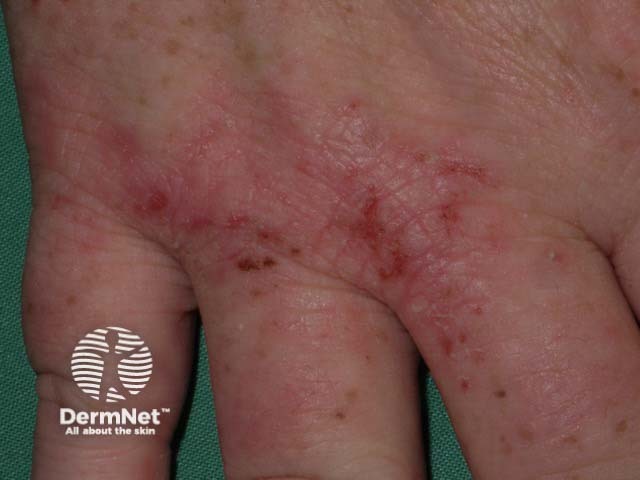
Hand dermatitis
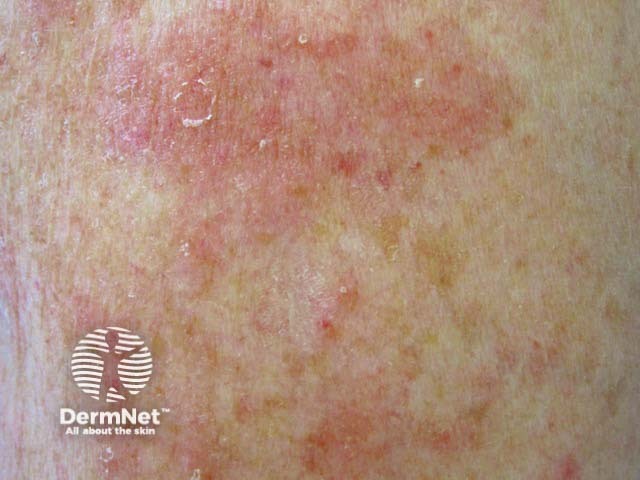
Nummular dermatitis
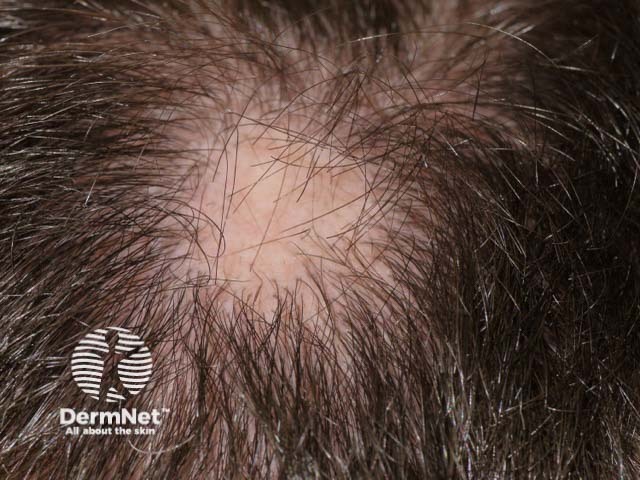
Alopecia areata
Extra-articular manifestations of rheumatoid arthritis often involve the skin particularly in patients with more severe disease. Some skin signs appear early in the disease course, others only in chronic long-standing rheumatoid arthritis; some are benign and self-limiting, while others may be a sign of serious systemic disease that can affect life-expectancy.
For female patients with rheumatoid arthritis and positive Ro/La autoantibodies, there is a 10% risk of a baby having neonatal lupus erythematosus.
Inadequately treated rheumatoid arthritis can result in disability and impact quality of life.