Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Update: March 2022.
Introduction Demographics Causes Clinical features Complications Diagnosis Treatment Prevention Outlook
Dry skin refers to skin that feels dry to touch. This occurs when the skin is lacking moisture in the outer horny cell layer (stratum corneum) and this results in cracks in the skin surface.
Dry skin is also called xerosis, xeroderma or asteatosis (lack of fat).
Both males and females of all ages can be affected. There is some racial variability in water and lipid content of the skin.
Dry skin that begins later may be seen in people with certain diseases and conditions, such as:
People exposed to a dry environment may experience dry skin, for example:
Dry skin is due to abnormalities in the integrity of the barrier function of the stratum corneum, which is made up of corneocytes.
The inherited forms of ichthyosis are due to loss of function mutations in various genes (listed in parentheses below):
Acquired ichthyosis may be due to:
Dry skin has a dull surface with a rough, scaly quality. The skin is less pliable and cracked. When dryness is severe, the skin may become inflamed and fissured.
Although any site can be dry, affected skin tends to involve the shins more than any other site.
The clinical features of ichthyosis depend on the specific type of ichthyosis.
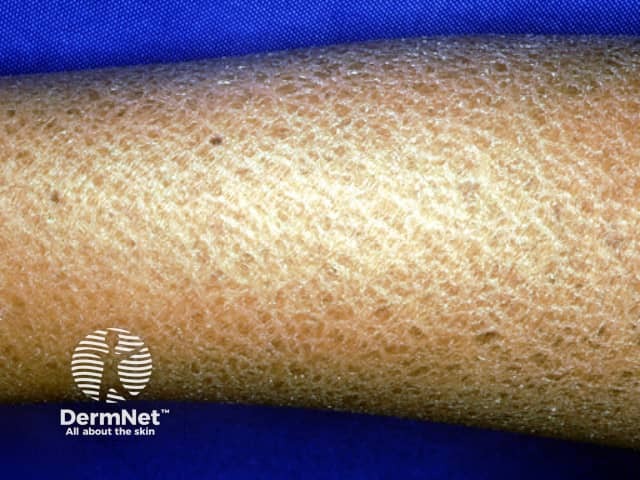
Ichthyosis
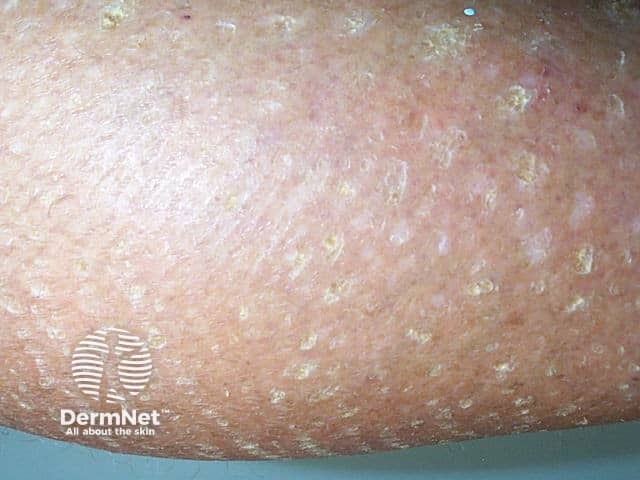
Close-up of ichthyosis
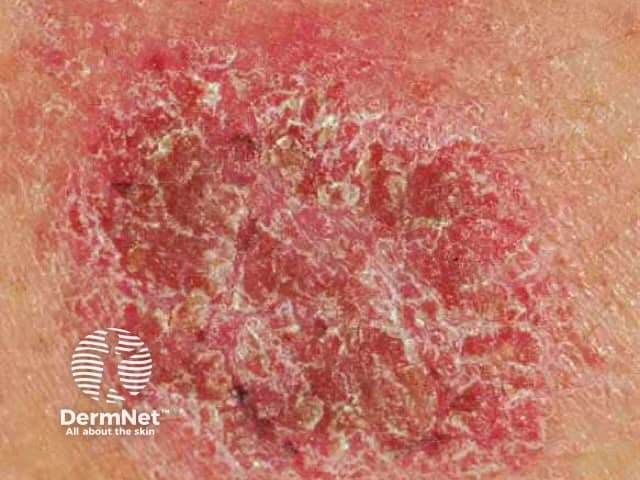
Dermatitis from dry skin
Dry areas of skin may become itchy, indicating a form of eczema/dermatitis has developed, such as:
When the skin of an older person is dry and itchy without a visible rash, it is sometimes called winter itch, 7th age itch, senile pruritus or chronic pruritus of the elderly.
Other complications may include:
The type of dry skin is diagnosed by careful history and examination.
In children:
In adults:
Sometimes a skin biopsy may be requested. There may be additional tests requested to diagnose some types of ichthyosis.
The mainstay of treatment of dry skin and ichthyosis is moisturisers/emollients. They should be applied liberally and often enough to:
When considering which emollient is most suitable, consider:
Emollients generally work best if applied to damp skin, if pH is below 7 (acidic), and if containing humectants such as urea or propylene glycol.
Additional treatments include:
A tendency to dry skin may persist life-long, or it may improve once contributing factors are controlled.