Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amy Stanway, Dermatology Registrar, Waikato Hospital, Hamilton, New Zealand, 2004.
Erythroderma is a generalised redness of the skin. It is a very severe skin condition that can be fatal. It can be the result of many inflammatory skin conditions, drugs and malignancies but in a third of cases it is due to psoriasis.
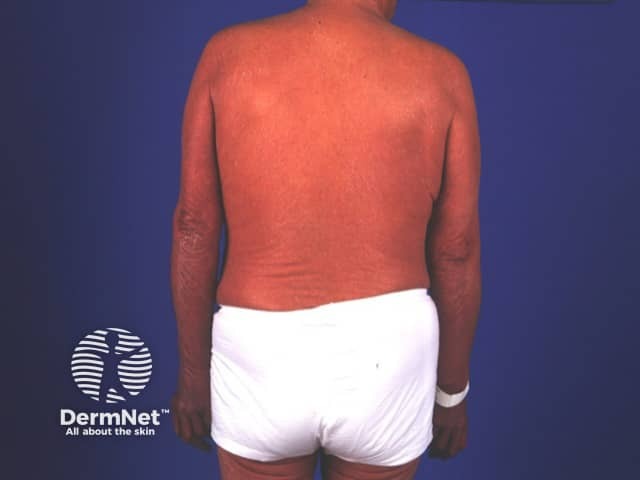
Erythrodermic psoriasis
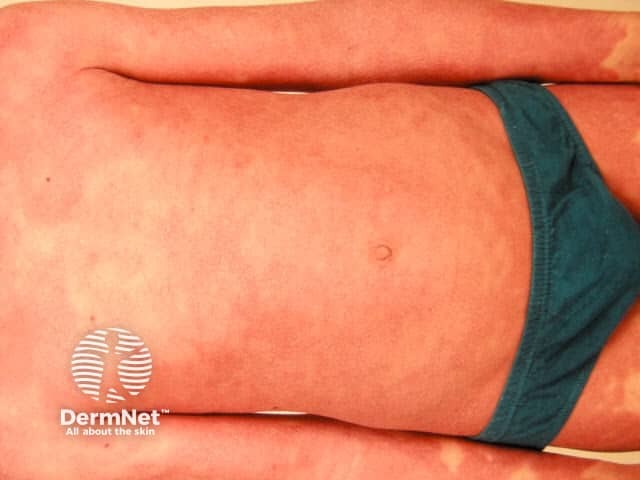
Erythrodermic psoriasis

Erythrodermic psoriasis
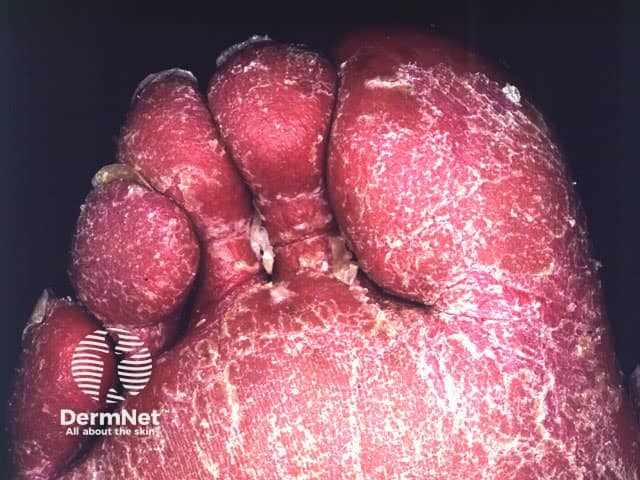
Erythrodermic psoriasis
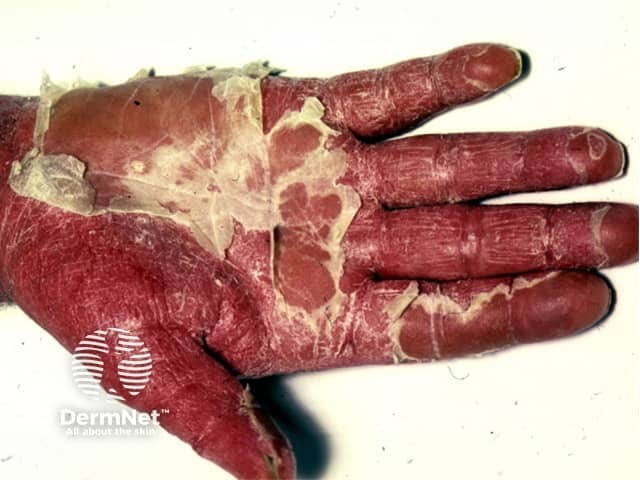
Erythrodermic psoriasis
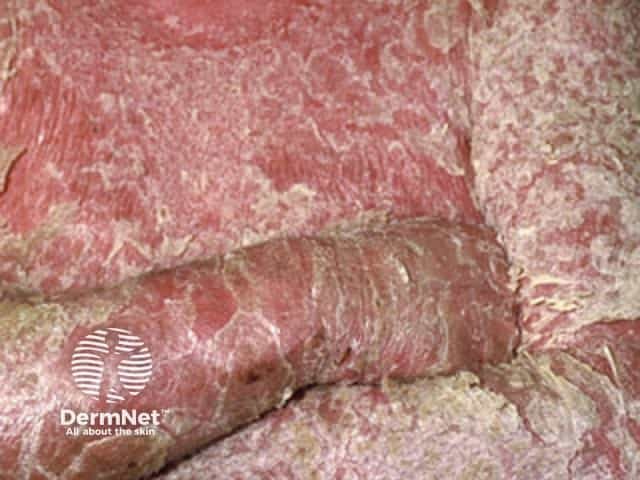
Erythrodermic psoriasis
Erythrodermic psoriasis may be precipitated by:
Erythrodermic psoriasis usually occurs in the setting of known worsening or unstable psoriasis but may uncommonly be the first presentation of psoriasis. Onset can occur acutely over a few days or weeks, or gradually evolve over several months from pre-existing psoriasis.
Features are those of any form of erythroderma (red dry skin all over the body).
Complications include:
Treatment of erythrodermic psoriasis can be difficult. Management includes:
Oral corticosteroids should be avoided if possible because withdrawal risks worsening of the erythrodermic state and may cause generalised pustular psoriasis. However, sometimes they are the only treatment that helps.
Topical tar preparations and phototherapy should also be avoided in the early treatment of erythrodermic psoriasis as they may worsen the condition.