Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: April, 2026
Authors: Dr Amy Stanway, Department of Dermatology, Waikato Hospital, Hamilton, New Zealand, 2004. Copy edited by Gus Mitchell. DermNet Update October 2021
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Guttate psoriasis is a form of acute psoriasis described as a shower of small, pink-red, scaly ‘raindrops’ that has fallen over the body.
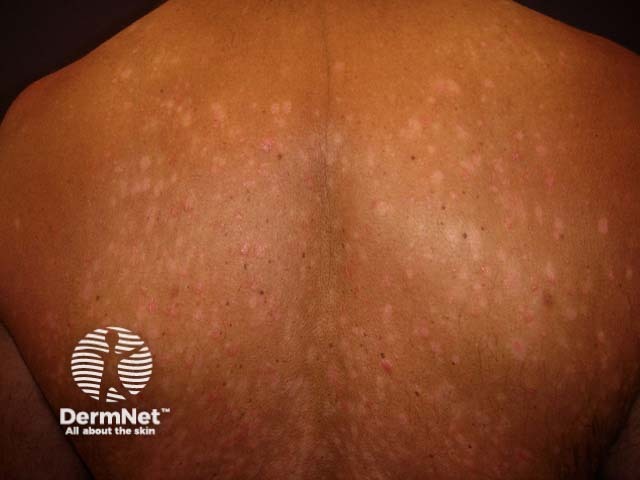
Guttate psoriasis
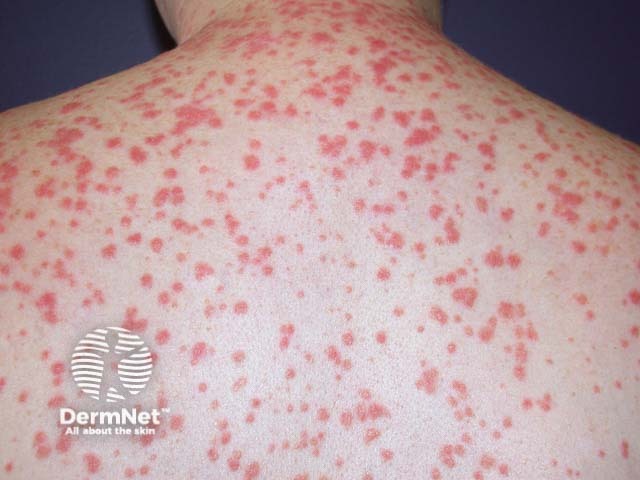
Guttate psoriasis
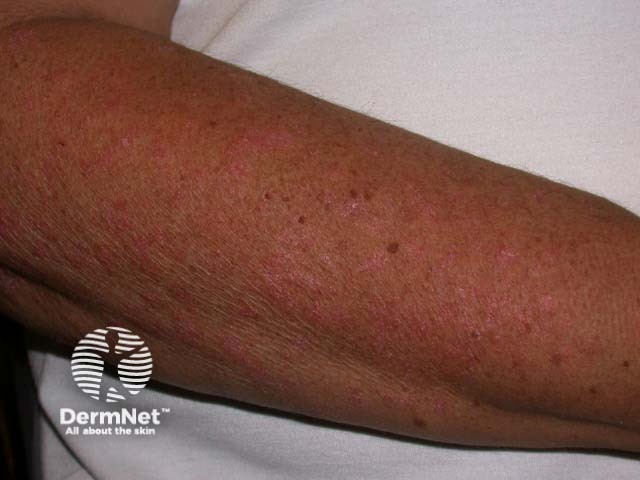
Guttate psoriasis
Guttate psoriasis tends to affect children and young adults; it is the second most common form of psoriasis in children after chronic plaque psoriasis. Both sexes and all races can develop guttate psoriasis. It is often the first presentation of psoriasis for an individual, but can also be seen in those with known chronic psoriasis.
Guttate psoriasis typically develops 1–2 weeks after a streptococcal infection of the upper respiratory tract, particularly tonsillitis, or other sites such as perianal streptococcal dermatitis. Beta-haemolytic streptococci can directly stimulate skin-homing T-cell proliferation in the tonsils.
Guttate psoriasis has been reported to follow SARS-CoV-2 infection (COVID-19) and other viral infections such as coxsackievirus. [see Enteroviral infections]
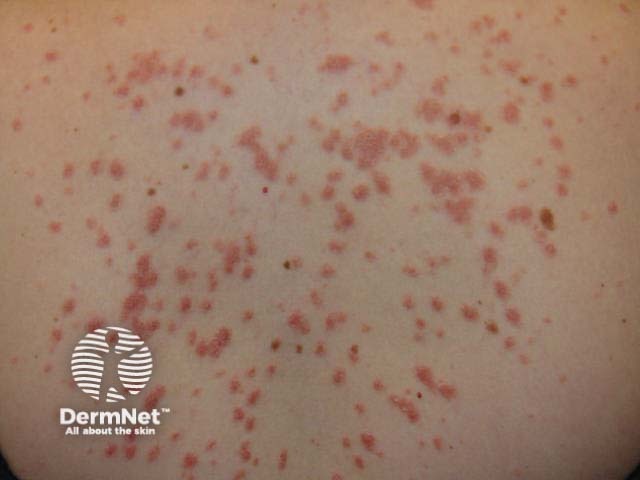
Guttate psoriasis
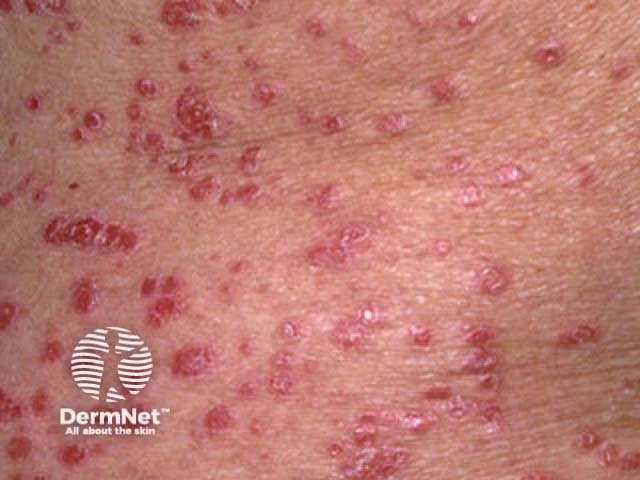
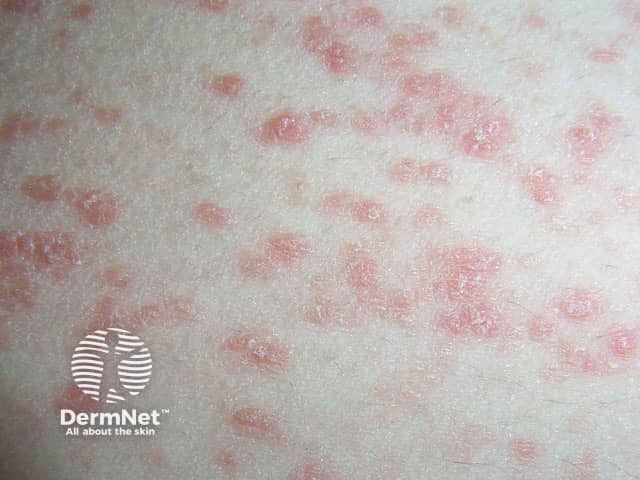
See also Guttate psoriasis images
These dermoscopy features are diagnostic and are seen in all skin types.
Guttate psoriasis is a clinical diagnosis, aided by dermoscopy, which can be confirmed on skin biopsy.
Examination and investigations should include a search for streptococcal infection.
Tests may include:
Recent opinion has questioned whether introduction of advanced therapy may alter the long term course of guttate psoriasis. Both ixekizumab and secikinumab induce rapid control of guttate psoriasis. Long-term follow-up is required to ascertain if this reduces the risk of chronic plaque psoriasis developing.
Guttate psoriasis often clears within 3-4 months, even without treatment. Patients with proven streptococcal infection triggering the guttate psoriasis have a good prognosis. However, it may recur with another episode of streptococcal infection.
Guttate psoriasis may become persistent and progress to chronic plaque psoriasis. In a study of over 190,000 patients with guttate psoriasis, 12.5% subsequently developed chronic plaque chronic psoriasis, with half of these cases occurring within one year of their initial presentation of guttate psoriasis.