Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Yasir Ammar Al-Dojaily, Virginia Commonwealth University School of Medicine, Richmond, USA (2022); Yan Ling Apollonia Tay, University of Otago, Adjunct A/Prof Amanda Oakley, Dermatologist (March 2020); Dr Louise Reiche, Dermatologist; Dr Helen Gordon, Medical Editor (June 2020).
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Demographics
Causes
Spread
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Prevention
Outcome
Submit your photo of COVID-19-related skin conditions
Please note that DermNet’s page is a summary about COVID-19 and may quickly become outdated.
Refer to Government websites for up-to-date information about COVID-19.

CDC*

New Zealand Government^
*Credit: CDC COVID-19 website
^Credit: New Zealand Government Unite against COVID-19 website (March 2020)
COVID-19 (coronavirus disease 2019) is a contagious viral disease caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
COVID-19 was first reported in December 2019 after a cluster of pneumonia cases in
Wuhan, China. It subsequently spread worldwide, prompting the World Health Organization (WHO) to declare a global pandemic on 11 March 2020.
The SARS-CoV-2 virus is transmitted from person to person through respiratory droplets. Common symptoms of COVID-19 resemble those of the common cold, including fever, cough, runny nose, and muscle aches. Approximately 1 in 3 of those infected are asymptomatic, and the majority of symptomatic patients experience mild to moderate disease. In severe cases of COVID-19, respiratory failure, organ failure, and altered mental status can occur, and the disease can be fatal. Vaccination and general infection prevention measures have been widely employed to curb contagion.
COVID-19 affects people of all ages. As of 31 August 2022, over 580,000,000 cases of COVID-19 have been reported worldwide with over 6,400,000 deaths.
Transmission of COVID-19 primarily occurs through exposure to contaminated respiratory droplets from infected persons. Some people may be at higher risk of severe disease such as the elderly, immunocompromised patients, and those with certain comorbidities such as:
Vaccination against COVID-19 has been shown to protect people from contracting the disease and from severe symptoms when infected.
COVID-19 is caused by SARS-CoV-2, an enveloped, positive-strand RNA virus. SARS-CoV-2 is a member of the Coronavirus family, which contains many other human viruses including those responsible for Middle Eastern Respiratory Syndrome (MERS), Severe Acute Respiratory Syndrome (SARS), and partly the common cold. SARS-CoV-2 is highly genetically similar to a bat-borne coronavirus, leading to suspicion that COVID-19 originated zoonotically.
The infection cycle for COVID-19 begins with the attachment of the virus to the surface of human cells. This is initiated by the binding of viral spike protein to the angiotensin-converting enzyme 2 (ACE2) receptor. The virus subsequently enters the cell and begins replicating using host cell machinery. Eventually, the virus escapes the host cell and infects other cells.
Since the discovery of SARS-CoV-2, multiple variants of concern have been identified:
The SARS-CoV-2 virus is found in droplets spread by an infected individual coughing, sneezing, talking, or touching items. The droplets may land on surfaces such as door handles, computer keyboards, and tabletops. The virus remains infectious for several days on smooth surfaces but for shorter periods on paper, wood, or cloth.
An uninfected individual may touch an invisible droplet then touch their face, transmitting the virus through the mucous membranes of their mouth, nose, and eyes, resulting in infection.
Patients are often infectious for a few days before becoming unwell, when unwell, and for some time after clinical recovery from COVID-19.
Infected people without symptoms are also infectious, although their rate of spreading the infection is about half of those with symptoms; this group is thought to contribute to the spread of the SARS-CoV-2 virus tenfold worldwide. In countries with rapid community spread, restrictions on movement and crowds are required to prevent a logarithmic increase in cases.
The severity of COVID-19 is variable. Approximately 80% of patients have mild symptoms or are asymptomatic. The incubation period is generally within 14 days of exposure; for most, the onset is 4–5 days. Those with shortness of breath can rapidly deteriorate, and therefore should be admitted to hospital for assessment and management.
The most common symptoms of COVID-19 are:
Less common symptoms include:
Rashes have been described in all types of patients with COVID-19; approximately 20% report rashes as the only clinical sign of COVID-19. It is unclear if cutaneous manifestations are associated with COVID-19 severity. The most common cutaneous manifestations include:
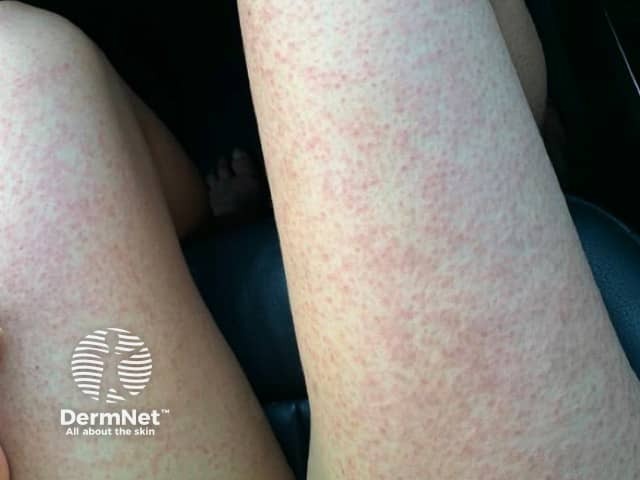
An exanthem
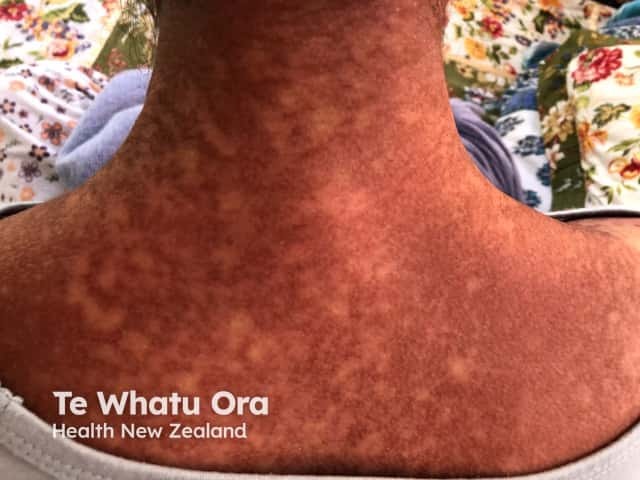
An extensive morbilliform exanthem
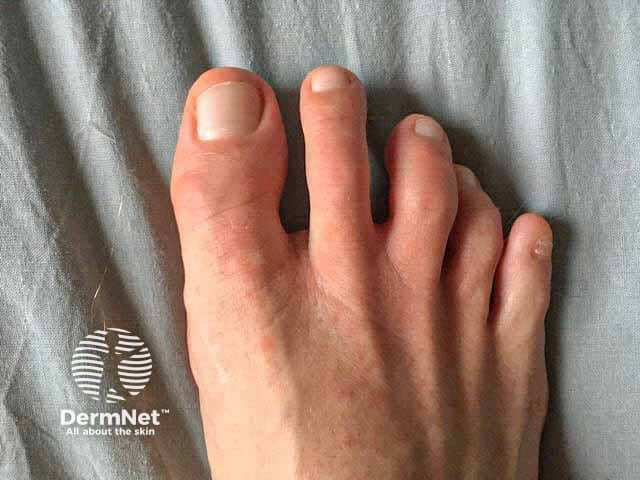
Chilblain-like COVID toes
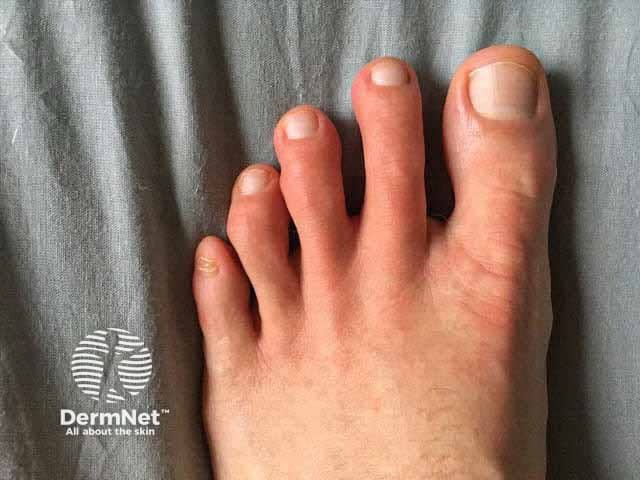
Chilblain-like COVID toes

Palmar erythema
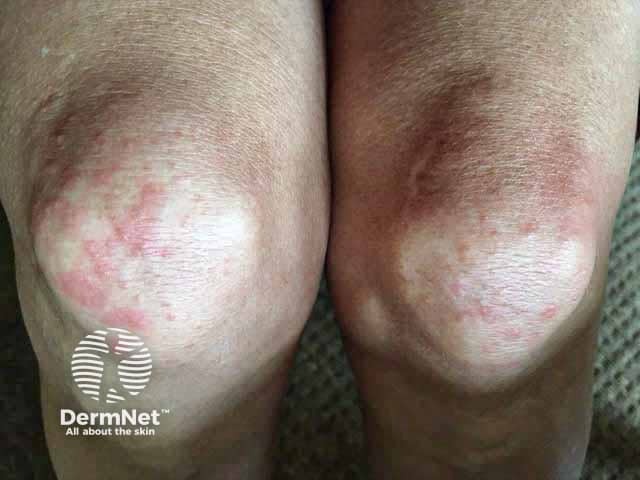
Vesicular lesions on the knees
Cutaneous manifestations of COVID-19 may present differently in darker skin types:
Complications include hypoxic respiratory failure (acute respiratory distress syndrome or ARDS) that may require intensive care. There have been increasing reports of ‘long COVID’ where symptoms last for 6 weeks or longer. Other potentially fatal complications include:
COVID-19 can be diagnosed using nasopharyngeal swabs.
Real-time reverse-transcriptase polymerase chain reaction (rRT-PCR) tests detect the SARS-CoV-2 virus. Rapid antigen testing (RAT) for the detection of viral proteins can be performed in the office or at home as a point-of-care test. However, it is less sensitive than PCR testing. RATs offer the most utility if performed within a week of symptom onset.
Other viruses can be tested in a similar manner including the influenza virus and respiratory syncytial virus (RSV). Antibody blood tests indicate whether someone has previously been exposed to SARS-CoV-2 and has mounted an immune response.
Breathless patients should have their oxygen saturations checked and monitored. Levels of oxygen saturation <94% on air are considered a marker of severity.
Additional tests can support diagnosis and evaluate severity of COVID-19, including:
As SARS-CoV-2 is excreted in the faeces of infected people, testing of sewage plants has become routine in some countries with low rates of infection. It can inform health authorities of the viral presence in the local community.
Individual patient suitability will include considering factors such as renal function, disease severity, concomitant medication, antiviral availability and accessibility, and duration of disease prior to treatment.
COVID-19 can be prevented. Many countries have enforced a ‘lockdown’ and have required people to stay at home. Consult your local guidelines for current recommendations.
Keeping a minimum distance between yourself and others to prevent physical contact and possible contamination is an essential step in preventing the spread of the virus.
See also: COVID-19 immunisation and immunomodulators/biologic agents and skin reactions to COVID-19 vaccines.
The outcome for COVID-19 depends on the severity of the illness. Typically, those with mild symptoms will recover within 2 weeks, however, severe cases can take three to six weeks or sometimes longer. Some are describing variable and often debilitating symptoms for months after contracting the infection (‘long COVID’) and this is under active investigation.
Death from COVID-19 has been reported in young, healthy people, although this is not common. Mortality from COVID-19 is highest in older people, especially those over 70 years. Mortality is higher in those with comorbidities associated with severe disease. ICU admission carries a poorer prognosis. National case fatality rates for COVID-19 range between 0.1–5.2% globally.
In New Zealand, refer to: