Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Yan Ling Apollonia Tay, Medical Student, University of Otago, Wellington, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. April 2020.
Introduction
Demographics
Examples
How to use
Side effects and risks
Healthcare workers and COVID-19
Personal protective equipment (PPE) generally consists of wearable items designed to shield users from environmental hazards. These hazards may be physical, chemical, biological, radiological, or nuclear in nature. PPE can be used in a variety of situations and configurations depending on the type of exposure.
A commonly held misconception is that PPE will fully protect users from harm. There will always be an element of risk when working in a hazardous environment. The purpose of properly used PPE is to reduce this risk of harm.

Ames hazmat suit

Occupational Safety Equipment
PPE is particularly used in the workplace due to exposure to occupational hazards. Occupations that require this hazard protection can include:
Certain forms of PPE such as gloves, dust masks, and hearing protection devices may also be used at home.
Different types of PPE have been designed to protect specific parts of the body.
A hazmat suit can provide comprehensive full-body protection.
Helmets and hair coverings are worn on the head.
Face shields, goggles, and masks are used to protect the eyes and face.
A face shield can be used to protect the user from injury or infection.
Goggles prevent foreign bodies or hazardous liquids from entering the wearer's eyes.
A face mask or respirator can prevent dust and infectious particles from being inhaled.
An apron, gown, or coverall can be used for body protection.
Gloves made of a wide range of materials can be used as a protective barrier to shield a wearer from hazards.
Boots made of different materials are used to protect the feet.
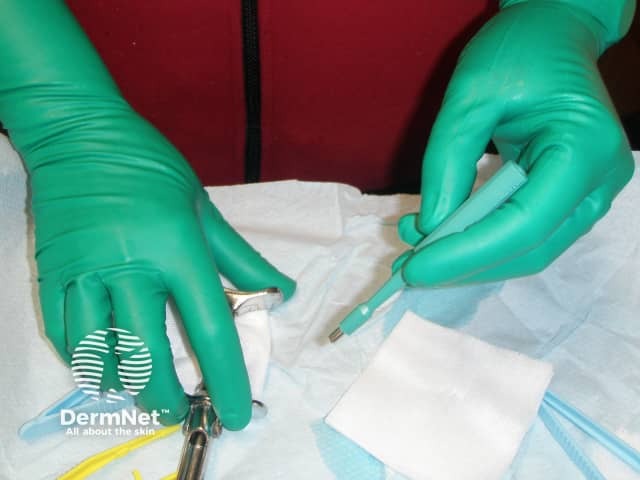
Green gloves in surgery
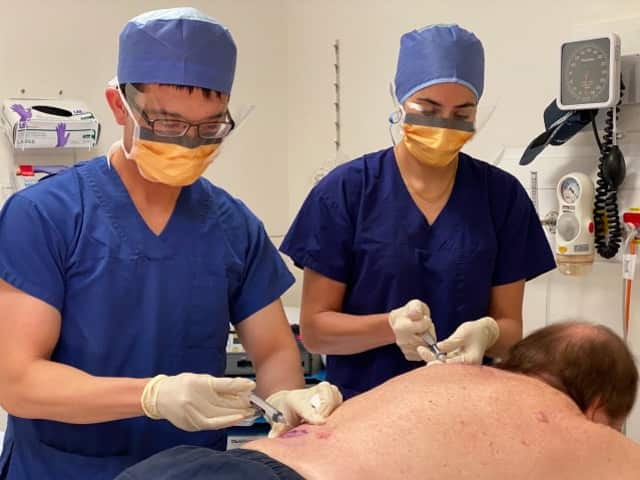
Personal protective equipment during minor skin surgery
PPE needs to be selected and sized carefully to best reduce exposure to specific hazards [3]. Professional organisations usually have specific guidelines for PPE selection within particular workplace settings.
PPE needs to be put on (donned) and removed (doffed) according to proper protocol [4].
Studies in healthcare workers have shown that the rate of contamination is reduced if the worker had completed a structured PPE training course [5]. Hence, PPE education sessions are highly recommended for all users. There is also evidence that supervised PPE use can decrease the rate of PPE protocol deviations and improve the quality of protection [6].
While PPE is extremely useful, some people may experience an unwanted side effect from PPE use, such as [7]:
Up to 99% of cutaneous side effects caused by occupational PPE are due to gloves, especially in healthcare workers [8]. Non-glove related dermatoses are more common in manufacturing [7].
Overheating due to PPE is very common [9]. PPE may cause an increase in body temperature by preventing heat from being lost via sweat evaporation [10]. Heavier forms of PPE may also increase body heat production due to the increased work of carrying the PPE.
Sweat loss and dehydration from overheating can cause heat-related illness, ranging from a mild heat rash (miliaria) to a life-threatening heat stroke [11]. Cooling measures should be undertaken immediately if there are any signs of heat illness [11].
Most contact dermatitis due to PPE is classified as irritant contact dermatitis, where the dermatitis is dose-related rather than due to the development of a hypersensitivity type of immune reaction. Examples of irritant reactions associated with PPE include:
Type I and type IV hypersensitivity reactions may develop to specific materials or chemicals used to make PPE.
Allergens causing allergic contact dermatitis due to PPE include [8, 12]:
Once an allergen is identified, contact with it should be avoided where possible.
Facial ulcers and acne have been reported in those who wear goggles or a mask for a long period of time due to pressure effects.
An ulcer is an open defect in the skin barrier. Prolonged pressure on the skin from a mask or a pair of goggles can cause a disruption in blood supply and subsequently, the death of overlying skin. This results in the formation of a pressure ulcer.
Acne mechanica is a complication of acne vulgaris. Pressure and friction on existing acne vulgaris can cause micro-abrasions that exacerbate inflammation [13]. The pustules may become deeper and more enlarged with continued pressure [14].
Irritant contact dermatitis occurs when the skin is directly exposed to soap and water, alcohol (in a sanitiser), or a harsh physical or chemical irritant. The irritant damages the skin barrier, enabling other irritants to enter the skin. This leads to local inflammation, pain, and itching.
Damaged skin is also more likely to develop a secondary bacterial infection [14]. Hence, measures should be taken to prevent skin damage such as removing the source of irritation and limiting the number of hours spent in PPE [13–15].
Regular face washing with a gentle cleanser may help with acne mechanica [14]. A lubricant or moisturiser may be applied at pressure areas [13].
The Center for Disease Control (CDC) recommends the following personal protective equipment for use in high-risk situations:
PPE is only protective if used correctly, particularly when donning and doffing the equipment. A buddy system is recommended to monitor the procedure as well as education and frequent practice to reduce the risk of self-contamination. Decontamination of gloves prior to doffing may further reduce the infection risk. PPE is the least effective tool in the CDC Hierarchy of Controls model to minimise the risk of infection for healthcare workers.