Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Dr Tristen Ng, Royal Perth Hospital, Western Australia (2023)
Previous contributors: Vanessa Ngan, Staff Writer (2003)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction Demographics Causes Clinical features Diagnosis Variation in skin types Complications Differential diagnoses Treatment Prevention Outcome
Pressure ulcers are skin and soft tissue injuries sustained from prolonged pressure. Specifically, they involve a breakdown of the skin, subcutaneous tissues and sometimes even deeper structures (tendons, muscle, bone) caused by cumulative pressure and are often related to pre-existing health conditions or injuries.
Pressure ulcers are also known as pressure sores, decubitus ulcers, or bed sores. They are often found on bony areas of the body with a thin soft tissue covering.
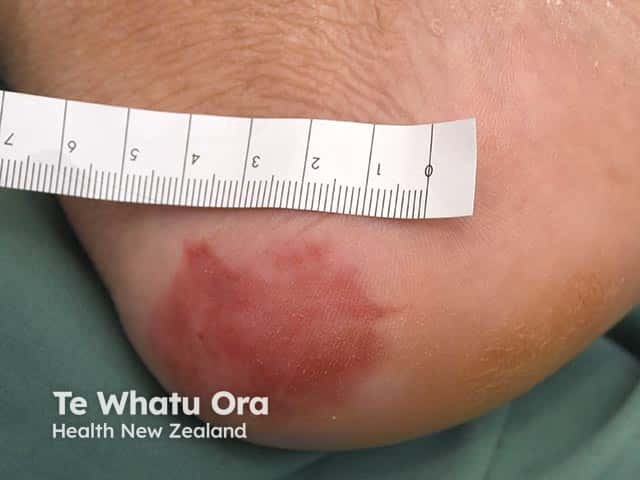
Incipient pressure ulcer on the heel - patient was paraplegic after a spinal injury (PU-patient4)
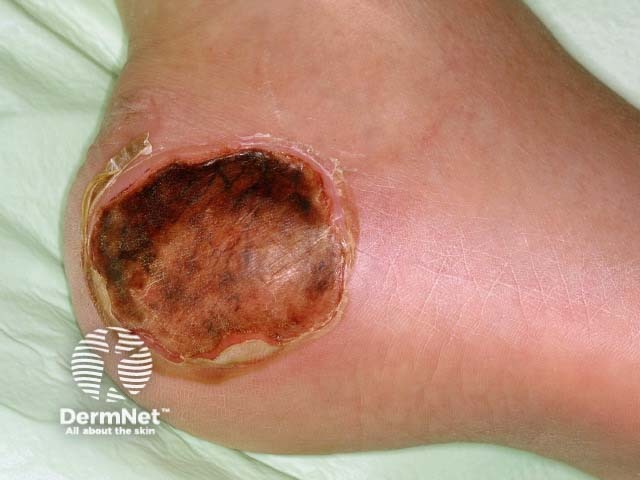
Pressure sore
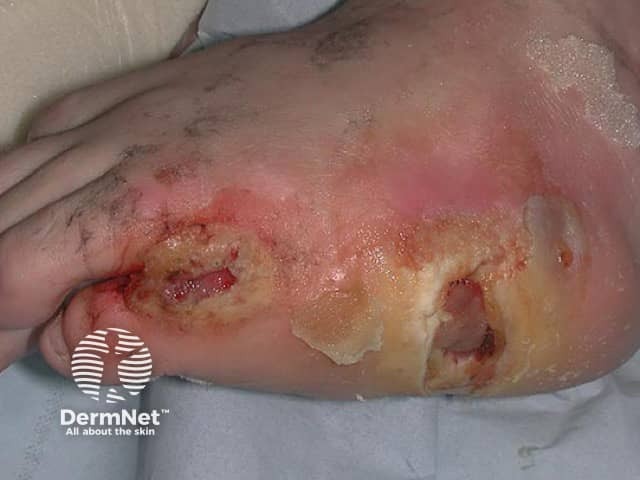
Chronic pressure ulceration due to immobility and anaesthesia due to spina bifida
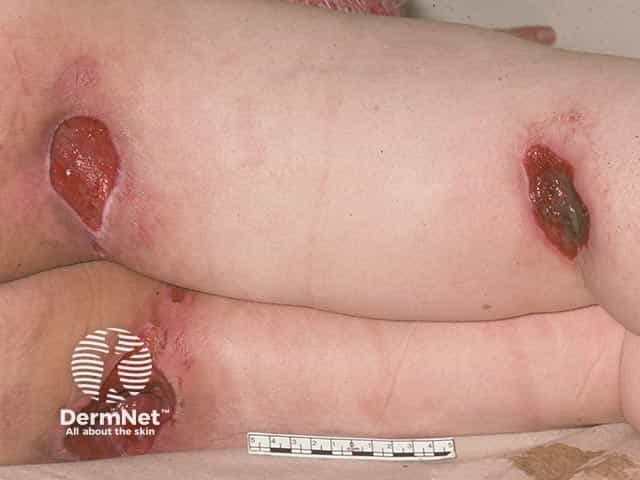
Pressure ulcers on gluteal fold and popliteal fossa in a wheelchair user with spina bifida
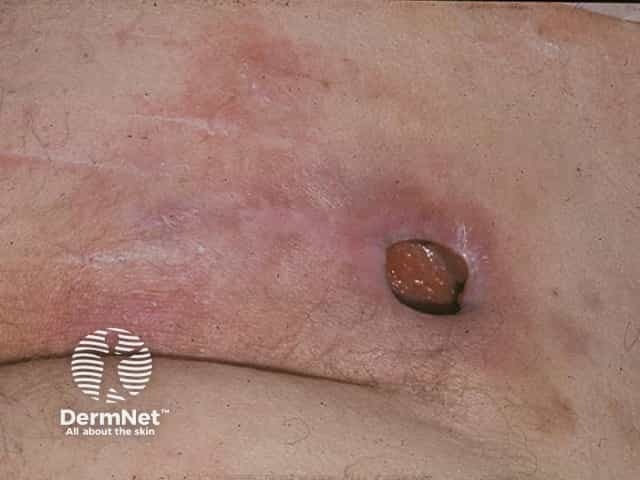
A deep and recalcitrant sacral pressue ulcer
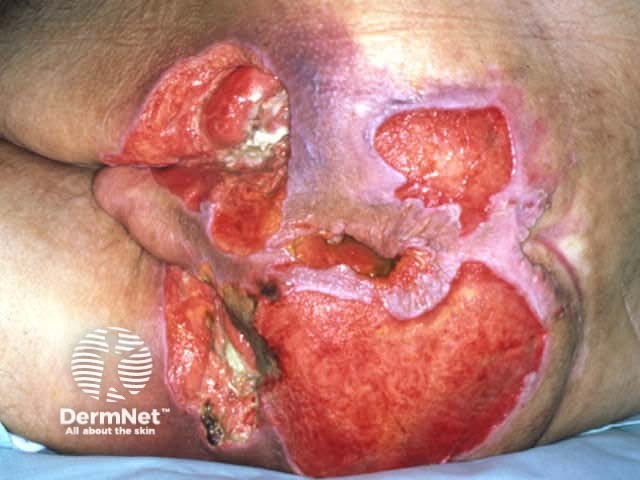
Chronic pressure ulcer
Although pressure ulcers can affect anyone, they are most often seen in the elderly and critically ill who are immobile for long periods.
High-risk groups include palliative care patients, comatose patients, quadriplegics, patients with spinal cord injuries, elderly people with orthopaedic fractures, and children with neurological dysfunction (eg, spina bifida, cerebral palsy, or spinal cord injury).
Pressure ulcers carry a high economic and psychological burden, due to hospital admissions for treatment of pressure ulcer complications and reduced quality of life for affected patients.
The most important cause of pressure ulcers is external pressure at a skin site for prolonged periods, although the exact mechanism is complex and poorly understood.
A proposed mechanism involves a complex interplay of local tissue ischaemia, reperfusion injury, increased capillary permeability, increased autophagy, and cell senescence causing direct insult to skin cells. After the inciting external pressure is gone, patients have a delayed reperfusion time which increases the risk of ulcer formation.
A ‘prolonged inflammatory phase’ hypothesis has also been proposed, whereby pressure ulcers do not follow the normal trajectory of inflammation, remodelling, and maturation, but are instead arrested in the ‘inflammatory’ phase of wound healing.
Identifying external and internal risk factors is important to prevent or minimise pressure ulcers.
External factors include:
Internal factors include:
The clinical features of pressure ulcers range from inflamed-looking, to severely ulcerated skin exposing muscle, tendon, and even bone. Commonly affected sites include the skin overlying the coccyx, vertebral column, heels, ankles, and elbows.
For patients who spend prolonged periods lying on their side, the iliac crest, the trochanters, and the ear helix may be affected. During the prolonged prone nursing of patients with severe COVID-induced respiratory disease, facial pressure ulcers were frequent.
The revised National Pressure Ulcer Advisory Panel’s (NPUAP) Pressure Injury Staging System is widely used in the staging and severity assessment of pressure ulcers based on their clinical features.
Other scoring systems, such as the Braden scale, are also used in some healthcare institutions.
Pressure ulcers remain a clinical diagnosis. The patient’s skin should be examined thoroughly from scalp to toe. Special attention must be given to skin in common pressure sites, under medical devices, and skin folds in patients with larger body habitus.
The mnemonic ‘BEST SHOT’ is used by the NHS Stop the Pressure campaign as a checklist for common pressure ulcer sites:
Temperature sensing technologies such as infrared thermography (IRT) have been developed to aid early prediction and early diagnosis of pressure ulcers. In a blinded prospective study of 70 patients in an ICU, IRT was found to detect skin changes 5–18 days before the visible appearance of pressure ulcers.
Stage 1 pressure ulcers may be missed in darker skin types (eg, Fitzpatrick type 4–6) due to the absence of visible blanching or erythema.
Other parameters such as altered skin sensation, warmth, and skin firmness should be assessed in patients with darker skin types.
Prevention of pressure ulcers can be classified into 3 domains: promoting movement, pressure reduction, and pressure distribution.
Prevention strategies include: