Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Robyn Moss, Intensivist, Australia (2022)
Previous contributors: Claire J. Wiggins, Riyad N.H. Seervai, Baylor College of Medicine, USA; Adjunct A/Prof Amanda Oakley, Dermatologist (2020).
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Causes and their specific skin signs
Skin signs from being in a coma
Other skin signs
Coma is a state of prolonged unconsciousness when the patient does not move or respond to a painful stimulus, light, or sound.
Coma usually requires management in an intensive care unit. Causes of coma include head injury, stroke, brain tumour, drugs, alcohol, diabetes mellitus, and infection. Assessment of the skin may provide a diagnostic clue as to the cause of the coma or reflect the patient’s comatose state.
Coma can result from a serious fall or accident.
Coma can be associated with a wide range of infections.
Bacterial meningitis
Viral encephalitis
Cryptococcal infection
Toxic shock syndrome and other severe skin infections can be associated with septic encephalopathy.
Coma is caused by a variety of toxins.
Cholinesterase inhibitor toxicity
Inhaled mercury exposure
Hypoxic ischaemic encephalopathy
Embolic stroke. There are different types of emboli. These may be distinguished by cutaneous findings:
Subarachnoid haemorrhage
Seizures
Coma can be a manifestation of a systemic disease.
Hepatic encephalopathy
End stage renal disease
Myxoedema coma
Hypoadrenalism
Diabetic ketoacidosis
Cutaneous vasculitic lesions can sometimes be associated with systemic pathology. This includes involvement of the cerebral vessels. Those particularly relevant to coma include:
Hyperviscosity syndrome
Cutaneous paraneoplastic syndromes
Coma can be associated with nutritional deficiencies.
Drug hypersensitivity syndromes
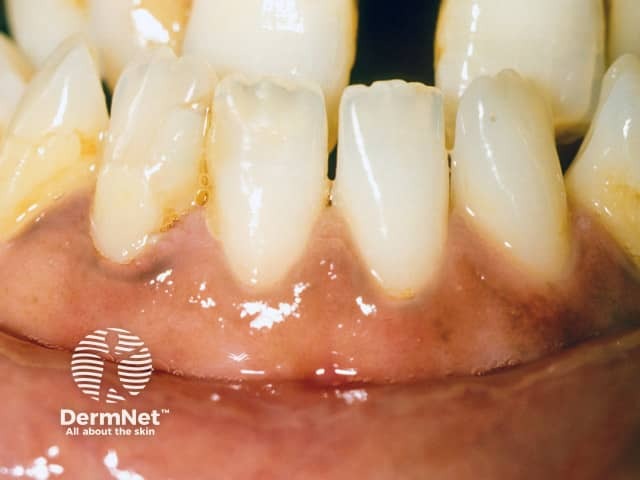
Gingival pigmentation was the clue to underlying Addison disease, presenting as an Addisonian crisis
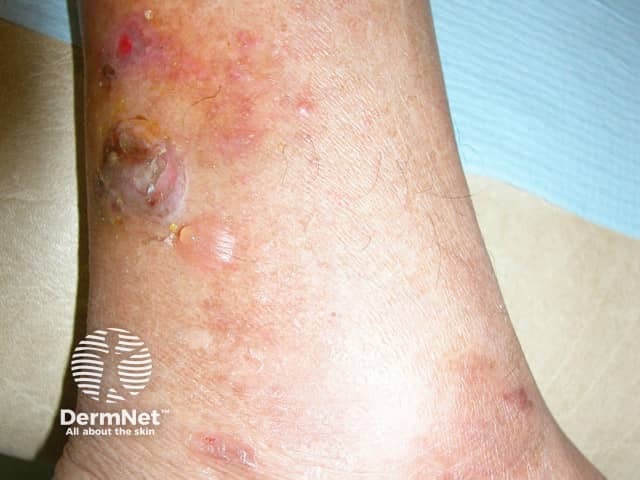
The blisters in this patient are due to bullosis diabeticorum; coma was due to hyperglycaemia
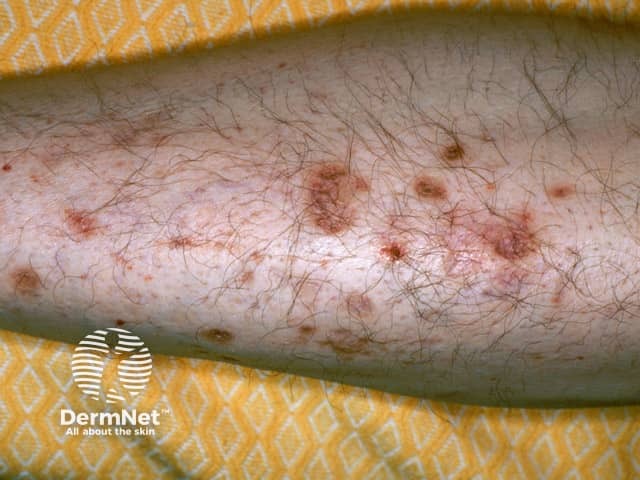
Diabetic shin spots, (diabetic dermopathy) was the clue to diabetes in this comatose patient
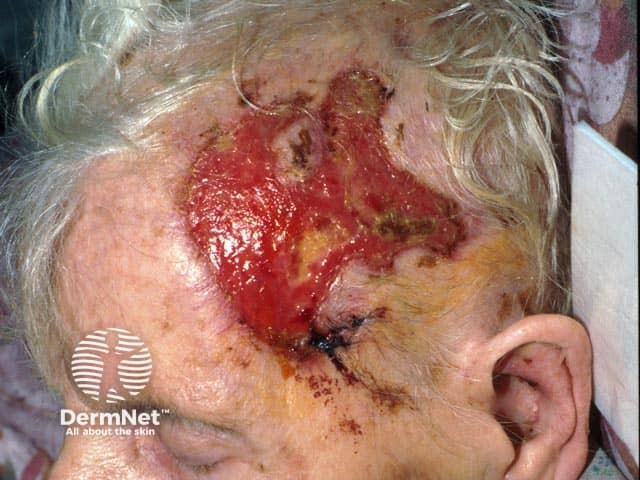
The extending ulcer on this lady's temple was the result of temporal arteritis, which had caused visual loss and ultimately coma
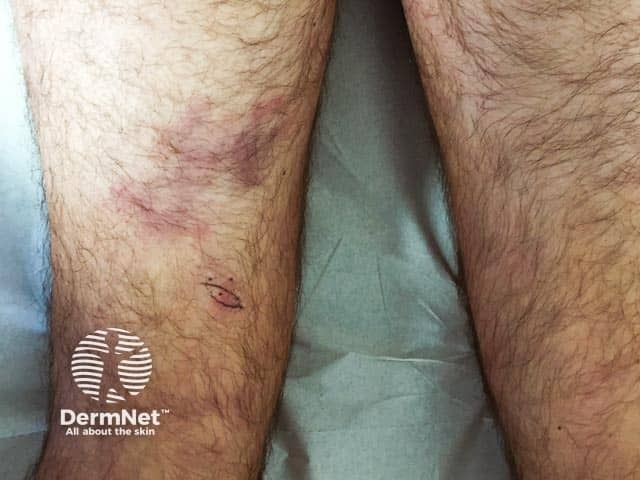
Livedo reticularis was the result of a medium-size-vessel vasculitis; associated cerebral vasculitis resulted in coma
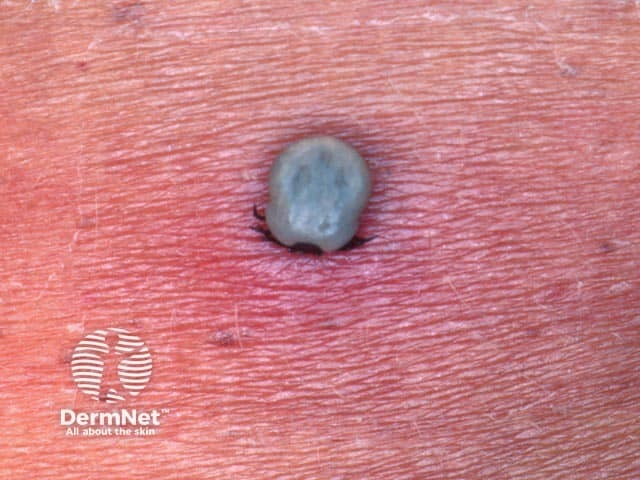
The tick causing tick-borne encephalitis was still attached
Pressure ulcers can occur due to immobility, hypotension, malnutrition, use of vasoactive medication, and inability to communicate their ischaemic pain.
Prevention of pressure ulcer includes limiting pressure, friction, and shear, while managing comorbid conditions that may interfere with wound healing, such as diabetes.
Coma blisters, multiple, tense, blood-filled blisters appearing at pressure sites, typically occur 2–3 days after the onset of coma and are often self-limiting, resolving after several weeks.
Traditionally associated with barbiturate overdose, coma blisters can develop in association with coma due to other causes (eg, diabetic coma). They are thought to be caused by hypotension-associated necrosis and pressure.
Skin biopsy shows a subepidermal blister and sweat gland and sweat duct necrosis. Thrombi in dermal vessels is often a clue the coma is not drug-induced.