Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Systemic diseases Autoimmune/autoinflammatory
Author: Lauren Eddy, Medical Student, Norwich Medical School, United Kingdom. Copy edited by Gus Mitchell. November 2020.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Treatment
Outcome
Psoriasis is an inflammatory systemic disorder with cutaneous, joint, and other manifestations, including the metabolic syndrome. Liver problems in psoriasis can be:
Non-alcoholic fatty liver disease is found in 20–30% of the general population, and up to 50% of patients with psoriasis, affecting both children and adults. The higher the PASI score (and thus the worse the psoriasis), the more likely there will be associated NAFLD. NAFLD is particularly seen with metabolic syndrome. In psoriasis, abdominal obesity, hypertriglyceridaemia, and hyperglycaemia are the three features of metabolic syndrome most likely to predict the additional presence of NAFLD. In children with psoriasis, obesity is an important marker for NAFLD.
The development of NAFLD can occur even in patients who have never had systemic psoriasis treatment. Case series have been reported from many countries and racial groups, with consistent prevalence results. There is no consistent distribution difference between sexes.
Primary biliary cirrhosis has been reported in 13% of psoriasis patients.
Hepatitis C infection is a known trigger for late-onset psoriasis. There is a risk of reactivation of latent hepatitis B and C with some systemic psoriasis treatments.
Adverse effects of systemic medications on the liver appear to be more common in those with pre-existing liver disease such as NAFLD.
A hepatodermal axis of circulating cytokines has been postulated to explain the strong association between psoriasis and liver disease. It is not clear whether it is hepatic inflammatory cytokines that stimulate keratinocyte hyperproliferation in the skin, or pro-inflammatory cytokine release from skin lymphocytes that causes insulin resistance and hence hepatic lipid accumulation. Adiponectin, an anti-inflammatory cytokine, is decreased in psoriasis.
Liver disease in psoriasis patients can range from simple steatosis (NAFLD) and nonalcoholic steatohepatitis (NASH), through to fibrosis and cirrhosis. However, it is usually asymptomatic and is found on blood tests incidentally or when planning systemic treatment. Rarely, the liver may be enlarged and palpable on examination or, in advanced disease, there may be skin signs of liver failure (see Skin signs of gastrointestinal disease).
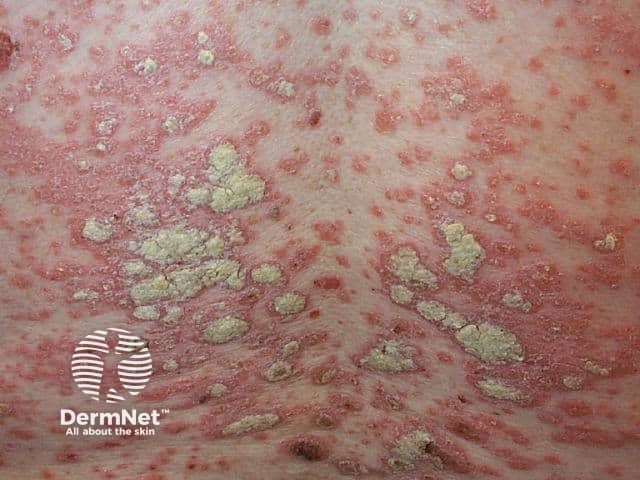
Chronic plaque psoriasis
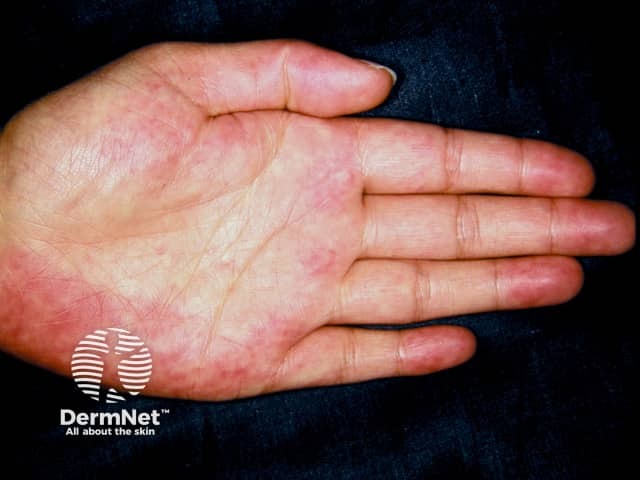
Palmar erythema of liver disease
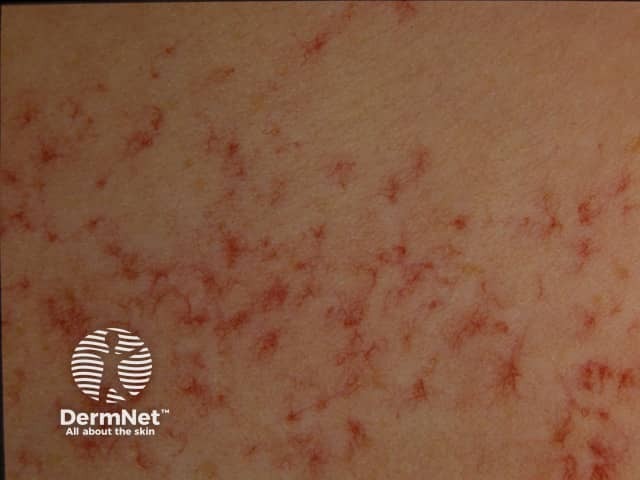
Multiple spider telangiectases - a sign of liver cirrhosis
Liver disease can progress from being asymptomatic to liver failure, hepatocellular carcinoma, and liver cirrhosis. Viral hepatitis can be reactivated by immunosuppressive systemic treatments used to treat psoriasis, so screening is essential before commencing these.
Liver disease is diagnosed initially on blood tests showing mild elevation of the liver enzymes alanine transaminase (ALT), aspartate transaminase (AST), and gamma-glutamyl transferase (GGT). Changes in albumin (low) and bilirubin (high) may also be seen. NAFLD is characterised by the AST/ALT ratio being less than 1, whereas in alcoholic liver disease this ratio is greater than 2. Blood tests for hepatitis B and hepatitis C infection should be included.
The Fatty Liver Index (FLI) tool looks at 4 parameters:
Imaging of the liver using ultrasound and transient elastography reduces the need for liver biopsy.
A study on the Steatosis-Associated Fibrosis Estimator (SAFE) suggests assessment using this scoring tool can assess significant liver fibrosis in patients with psoriasis with good accuracy.
Lifestyle changes to minimise the risk or prevent progression of NAFLD include:
Systemic treatments used to treat psoriasis may affect the liver or lipids, and so should be avoided or minimised with careful monitoring in patients with liver disease; methotrexate, ciclosporin, and acitretin. High doses of ciclosporin and acitretin are needed in obese patients, which further increases the risk of adverse effects. Apremilast may be a suitable alternative.
Biologic agents (see Biological agents for psoriasis) approved for use in psoriasis vary in their effects on the liver. Etanercept has been reported to improve insulin sensitivity, reduce the AST/ALT ratio, and reduce the hepatic fibrosis risk. Adalimumab and ustekinumab are reported to be safe to use for those with liver disease. Infliximab, however, may cause liver problems and should be used with caution in patients with liver failure.
Hepatitis C infection is now a curable disease. Treatment of associated hypertension, type II diabetes mellitus, and/or hyperlipidaemia reduces the risk of further complications of the metabolic syndrome.
NAFLD is predicted to be the major indication for liver transplantation world-wide.
A large study in the UK found 14.1% of patients with severe psoriasis (PASI>10) had advanced liver fibrosis. This was a 7-fold increase above the general population. It was associated with insulin resistance, diabetes, and obesity.
Liver cirrhosis and hepatocellular carcinoma reduce long-term survival.