Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Beth Wright, Medical Registrar, Perth, Australia; Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2013.
Introduction Prevalence Why do skin problems occur on the stump after amputation? Which skin conditions affect the amputation stump? The impact of stump dermatoses on the amputee Skin care for amputees Treatment of amputation stump dermatoses
Amputation stump dermatoses are skin diseases affecting the stump, following the amputation of a limb. They can occur immediately after surgery, or not until many years later. They are also called amputation-related dermatoses.

Artificial leg
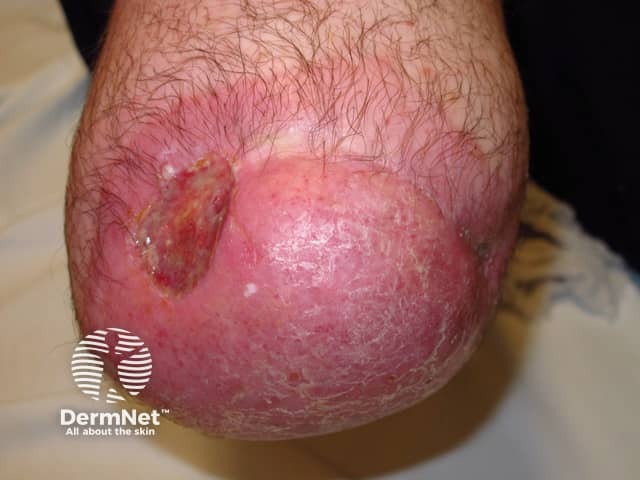
Ulceration and dermatitis
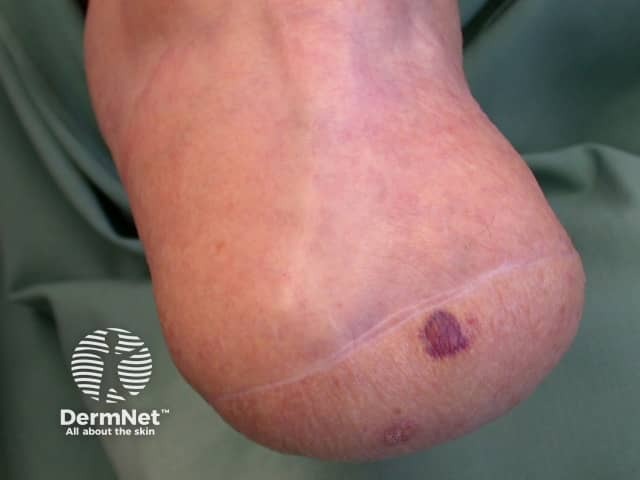
Pressure-induced purpura
Stump dermatoses are reported to affect between 34–74% of amputees [1]. Figures vary according to the design, population samples and methods used in the studies.
Skin problems tend to persist long term, as described in war veterans 38 years after amputation [1].
Factors that make the stump vulnerable to skin disease include:
Although dermatoses may arise before a prosthesis is fitted and used, the main contributing factors are the degree of activity and the use of a prosthesis [2]. Severity also depends on:
Skin problems affecting an amputation stump are listed below.
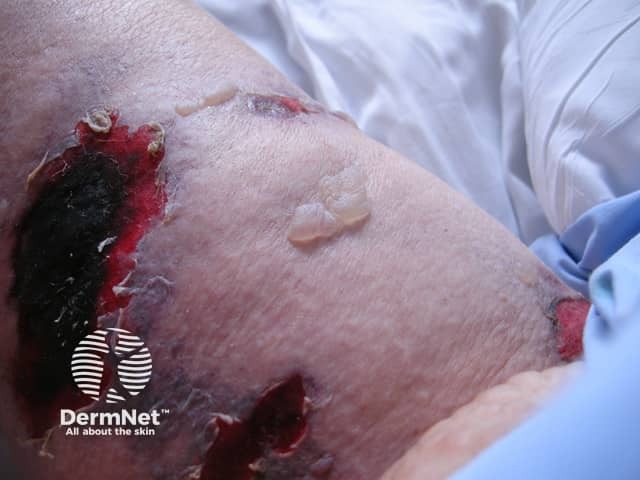
Vasculopathy affecting amputation stump diabetic
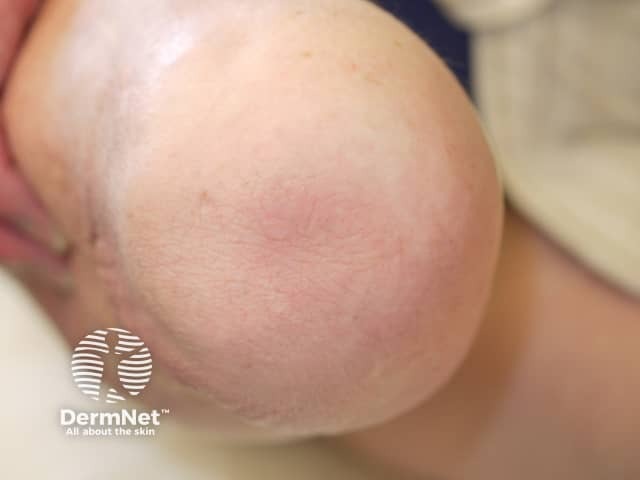
Callus formation on amputation stump
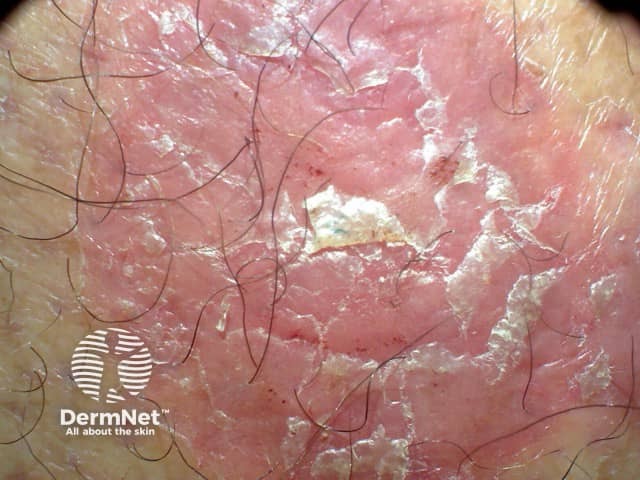
Psoriasis
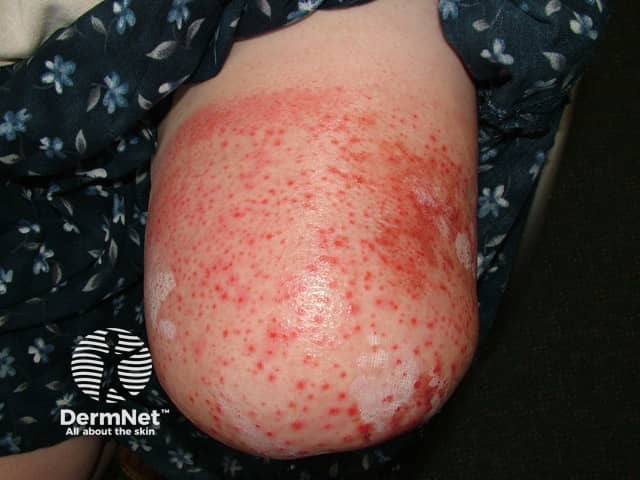
Acute dermatitis affecting amputation stump
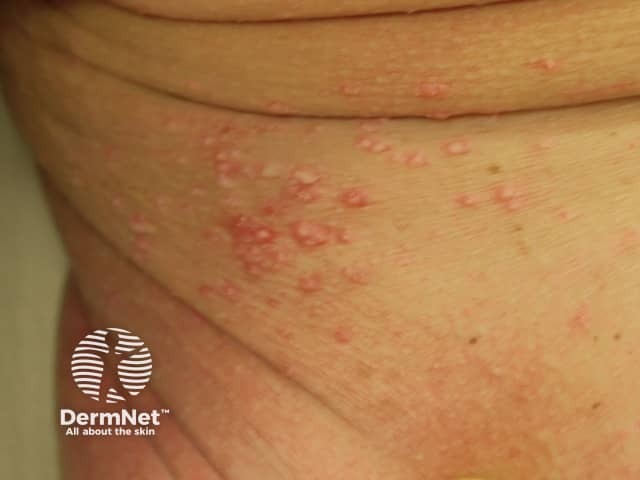
Molluscum contagiosum affecting amputation stump
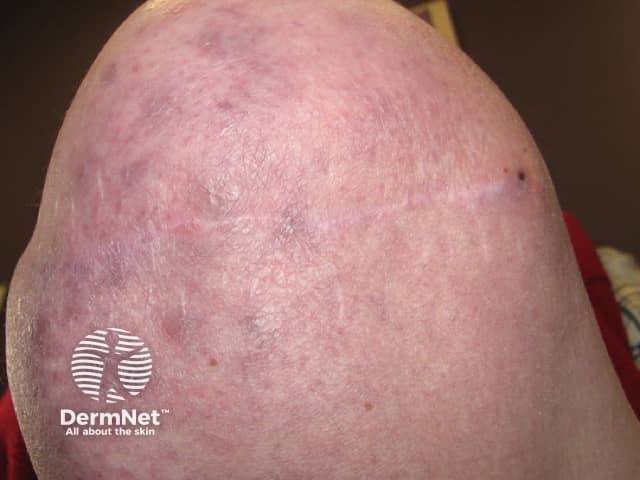
Perniosis affecting amputation stump
Of these, pressure ulcers and skin breakdown (39%) and infection (25%) are most common [1][2][5], with up to one quarter of amputees being affected more than 50% of the time.[1] In some cases, rashes are unexplained.
Common skin lesions such as warts, moles and skin cancer can also arise on the stump.
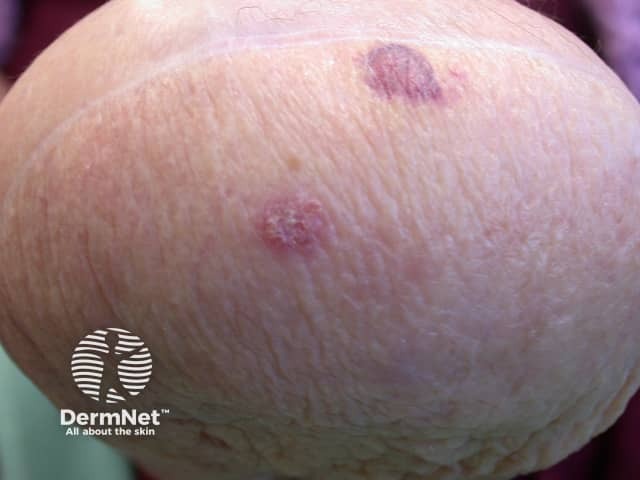
Intraepithelial carcinoma on amputation stump
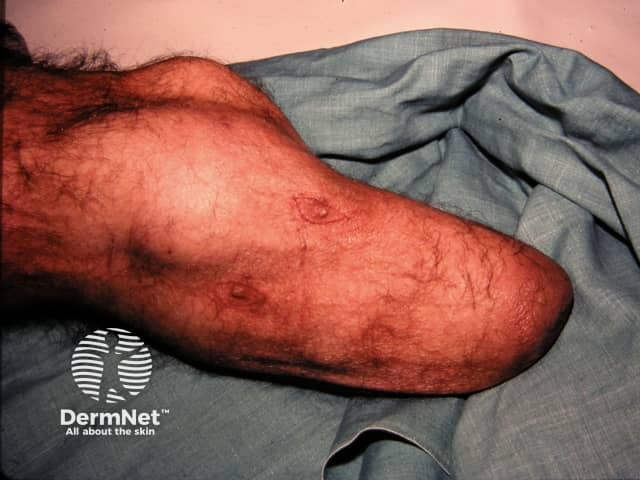
Squamous cell carcinoma on limb of amputee
Adverse physical, mental, and emotional effects of stump dermatoses may affect wellbeing and quality of life, including:
To prevent complications due to poor skin care, check the amputation stump daily, keep the skin dry by changing damp socks promptly, and protect bony prominences and pressure-sensitive areas from injury.
Diabetics need to be vigilant to monitor and control blood sugar levels, and to inspect numb areas of skin frequently.
Treatment of stump dermatoses depends on careful evaluation to establish contributing factors.
Unfortunately the skin may fail to adapt to mechanical pressures, materials, and closed environment associated with the use of a prosthesis [1].