Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated July 2015.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Treatment
Outlook
Future treatments
Hyperhidrosis is the name given to excessive and uncontrollable sweating.
Sweat is a weak salt solution produced by the eccrine sweat glands. These are distributed over the entire body but are most numerous on the palms and soles (with about 700 glands per square centimetre).
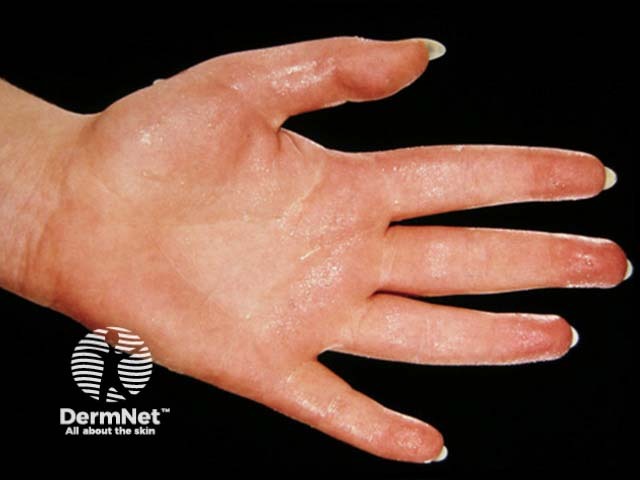
Hyperhidrosis
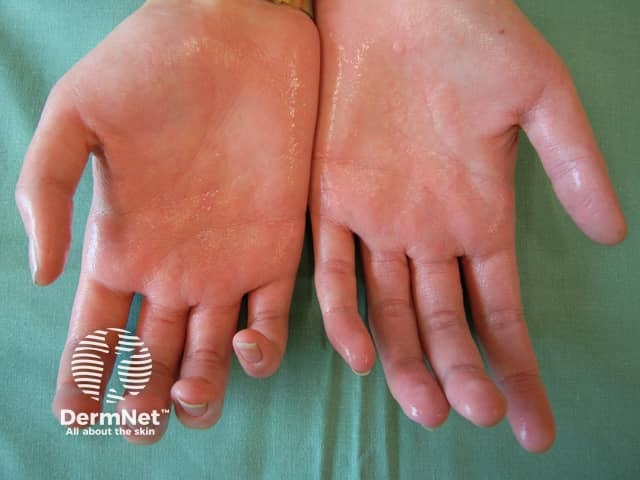
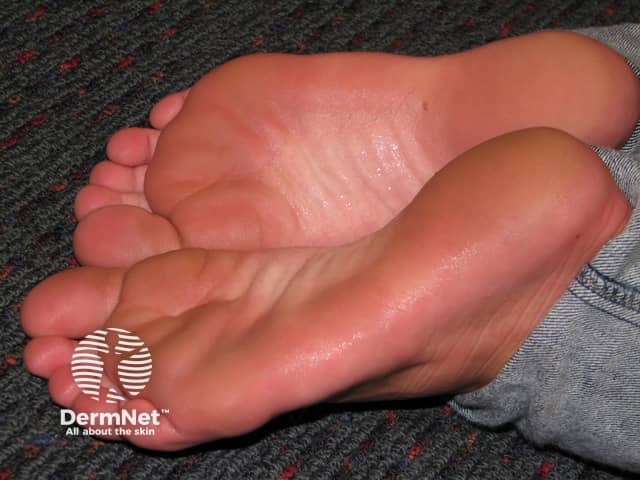
Primary hyperhidrosis is reported to affect 1–3% of the US population and nearly always starts during childhood or adolescence. The tendency may be inherited, and it is reported to be particularly prevalent in Japanese people.
Secondary hyperhidrosis is less common and can present at any age.
Primary hyperhidrosis appears to be due to overactivity of the hypothalamic thermoregulatory centre in the brain and is transmitted via the sympathetic nervous system to the eccrine sweat gland.
Triggers to attacks of sweating may include:
Causes of secondary localised hyperhidrosis include:
Causes of secondary generalised hyperhidrosis include:
Hyperhidrosis can be localised or generalised.
It can be primary or secondary.
Hyperhidrosis is embarrassing and interferes with many daily activities.

Excessive sweating in armpits
Hyperhidrosis is usually diagnosed clinically. Tests relate to the potential underlying cause of hyperhidrosis and are rarely necessary for primary hyperhidrosis.
The precise site of localised hyperhidrosis can be revealed using the Minor test.
Screening tests in secondary generalised hyperhidrosis depend on other clinical features but should include as a minimum:
Oral anticholinergic drugs
Beta-blockers
Calcium channel blockers, alpha-adrenergic agonists (clonidine), nonsteroidal anti-inflammatory drugs and anxiolytics may also be useful for some patients.
Overactive sweat glands in the armpits may be removed by several methods, usually under local anaesthetic.
Division of the sympathetic spinal nerves by chemical or surgical endoscopic thoracic sympathectomy (ETS) may reduce sweating of face (T2 ganglion) or armpit and hand (T3 or T4 ganglion) but is reserved for the most severely affected individuals due to potential risks and complications.
Lumbar sympathectomy is not recommended for hyperhidrosis affecting the feet, as it can interfere with sexual function.
Localised primary hyperhidrosis tends to improve with age. The outlook for secondary localised or generalised hyperhidrosis depends on the cause.
Several research projects are underway to find safer and more effective treatments for hyperhidrosis. These include: