Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Eileen J McManus, Advanced Neurology Trainee, Waikato Hospital, Hamilton, New Zealand. Technical Editor: Elaine Mary Luther, Medical Student, Ross University School of Medicine, Barbados. DermNet Editor in Chief: Adjunct A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. February 2020.
Introduction Demographics Causes Clinical features Classification Complications Diagnosis Differential diagnoses Treatment Outcome
Cutaneous dysaesthesia is a condition defined as an unpleasant and abnormal sensation in the skin. In the mouth, a similar sensation is called oral dysaesthesia.
It can be classified as generalised or localised. There are multiple variants of localised cutaneous dysaesthesia, which differ in location, duration, and symptom severity.
Anyone can get cutaneous dysaesthesia. There is a possible female predominance in some variants, such as scalp dysaesthesia and notalgia paraesthetica [1].
Generalised cutaneous dysaesthesia is associated with neurological diseases, including:
Localised dysaesthesia often follows nerve trauma, impingement, or irritation. This can be intracranial (in trigeminal trophic syndrome), spinal, or peripheral.
Other reported causative associations with cutaneous dysaesthesia are described below.
Dysaesthesia or paraesthesia describes positive cutaneous symptoms such as pruritus, burning, crawling, stinging, hyperaesthesia, allodynia, and pain; and negative symptoms such as anaesthesia or cold sensation. One or more of these symptoms may be present.
The examination of the affected area may be normal or there may be signs of the underlying disease if any, or secondary to rubbing and scratching (if itchy).
Generalised cutaneous dysaesthesia presents with dysaesthesia affecting most or all of the skin surface. Symptoms can be exacerbated by temperature change, heat, or the touch of clothing.
Localised cutaneous dysaesthesia presents with symptoms confined to one area.
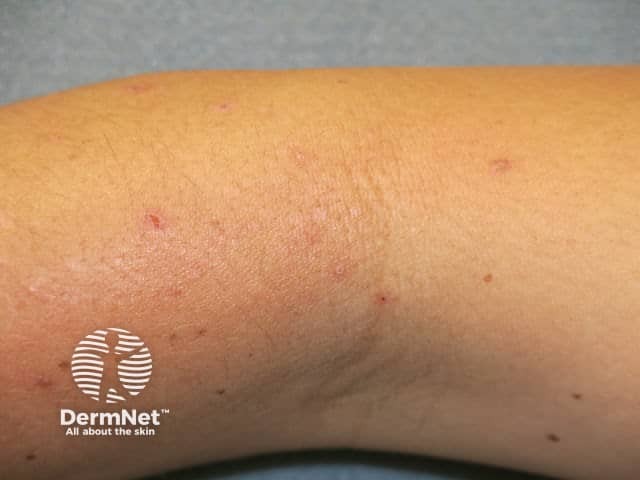
Lichenification from scratching
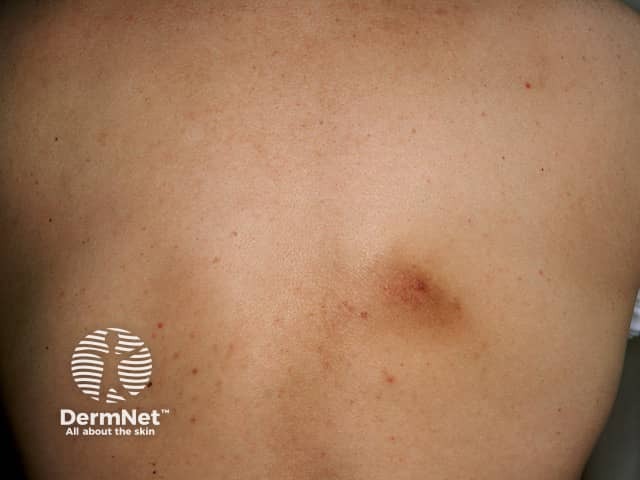
Notalgia paraesthetica
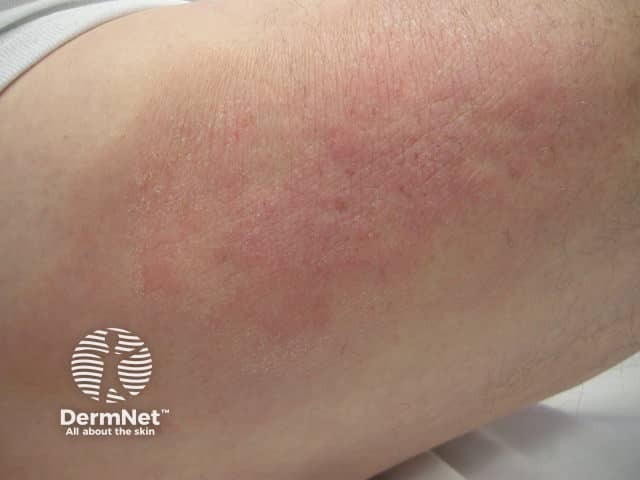
Meralgia paraesthetica
Localised cutaneous dysaesthesia has been classified in the following conditions.
The main complication of cutaneous dysaesthesia is decreased quality of life and impact on mood and mental health.
Generalised cutaneous dysaesthesia is a clinical diagnosis after a detailed history and examination have excluded a primary dermatological disease.
Serological tests may include testing for the following:
Other tests may include:
The diagnosis of localised cutaneous dysaesthesia is based on clinical suspicion. A comprehensive history and examination are needed to identify any underlying cause. For instance, hyperreflexia, weakness, or autonomic dysfunction can indicate a spinal cord pathology.
Other diagnostic tests may include:
The differential diagnosis of cutaneous dysaesthesia should be broadened if the skin is normal or abnormal (eg, lichenification might be due to eczema, nasal ulceration might be due to skin cancer).
Somatisation is sometimes implicated with cutaneous sensory disorders such as compulsive skin picking.
Cutaneous dysaesthesia is difficult to treat effectively. Management depends on the cause, body site, and severity of symptoms.
Symptomatic therapy may include:
Additional treatments may include:
Prognosis depends on aetiology, symptom severity, and treatment response. There is no effect on life expectancy.