Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Amanda Oakley, Dermatologist, New Zealand, 2002. Updated: Dr Annabelle Yi Zhang, Auckland City Hospital, New Zealand; Honorary Associate Professor Paul Jarrett, Dermatologist, Middlemore Hospital and Department of Medicine, The University of Auckland, Auckland, New Zealand. Copy edited by Gus Mitchell. March 2021
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Brachioradial pruritus is a localised form of neuropathic cutaneous dysaesthesia on one or both upper limbs. The presentation is usually an itch without rash; however, scratching and rubbing can result in secondary skin changes.
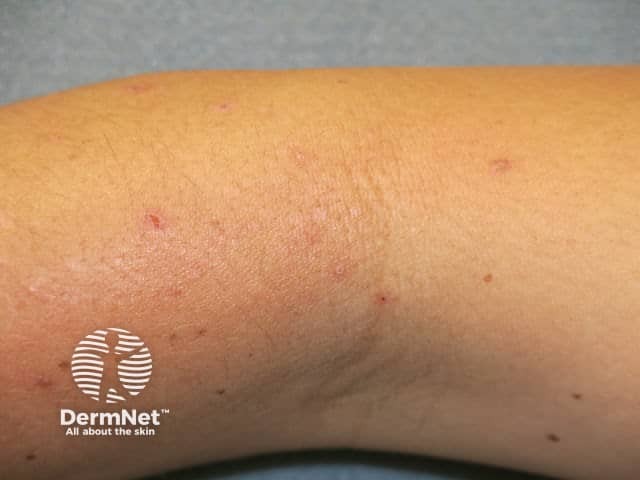
Lichenification from scratching
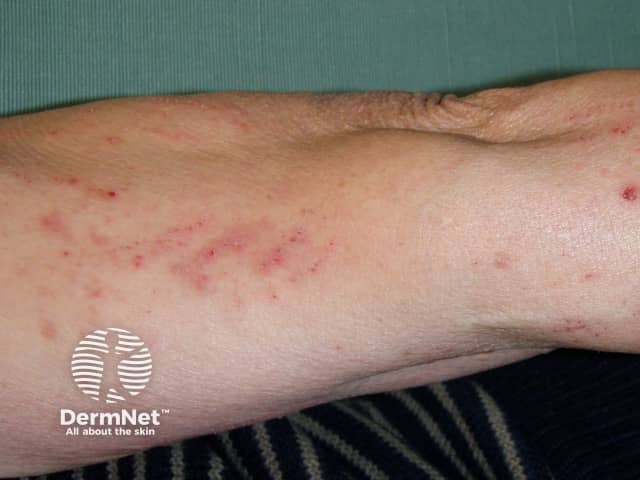
Excoriations
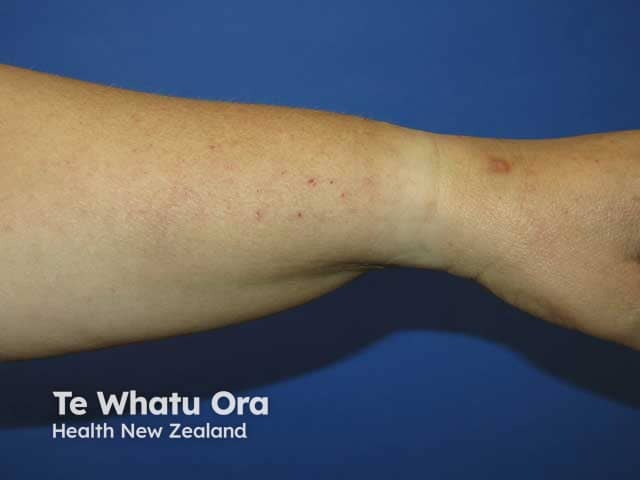
Excoriations
Brachioradial pruritus can affect both sexes, all skin types, and age groups ranging from early teenage years through to the elderly, but is typically seen in fair-skinned women in late middle-age.
Brachioradial pruritus is likely to be multifactorial in origin. There are two current theories to explain brachioradial pruritus:
Brachioradial pruritus presents as itch without rash, most commonly on the proximal forearm in the C6 distribution overlying the brachioradial muscle. It may be unilateral or bilateral, and may extend to adjacent dermatomes or skin sites, such as the shoulders, back, and chest.
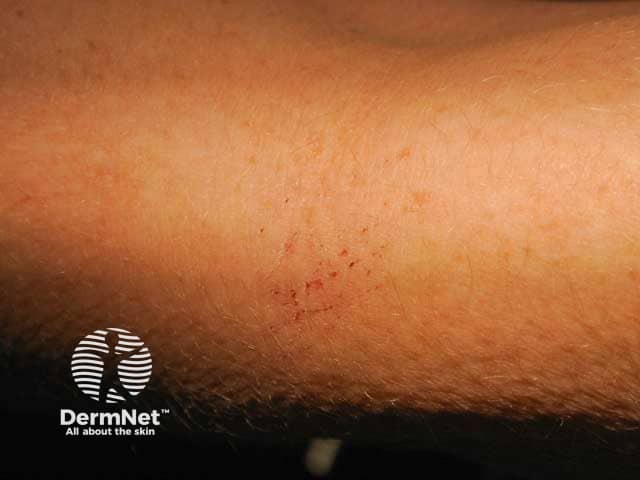
Brachioradial pruritus, forearm early excoriations
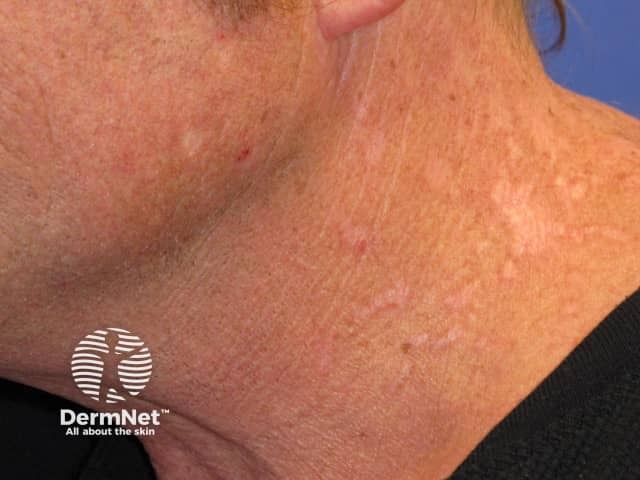
Brachioradial pruritus, scarring on the neck
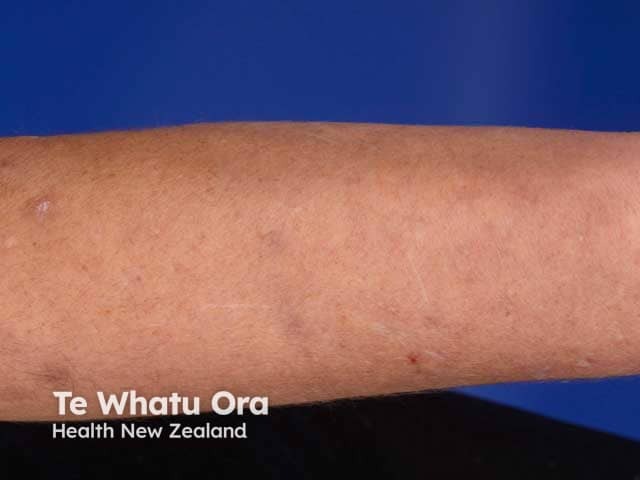
Brachioradial pruritus, upper limb secondary skin lichenification
Brachioradial pruritus is a clinical diagnosis based on history and examination.
Cervical spine imaging (X-ray, MRI) should be considered particularly in patients with neurological symptoms/signs and/or a lack of seasonal variation.