Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Leeatt Green, Resident Medical Officer, Western Health, Melbourne, Victoria, Australia. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. September 2018.
Introduction
The classical complement pathway
The alternate pathway
Mannose-binding lectin
Complement system regulation
Skin conditions from defects in complement system
Complement testing and diagnosis
Complement is part of the innate immune system.
Complement incorporates proteins, which circulate in the blood in their inactive form, and some cell membrane receptors [2]. The proteins are mostly synthesised by the hepatocytes in the liver.
The components of complement are systematically named alphanumerically: C1, C2, C3, C3a, C3b, C4, C4a, and so on.
There are three ways to activate the complement system:
All three pathways culminate in the conversion of C3 to C3 convertase [2].
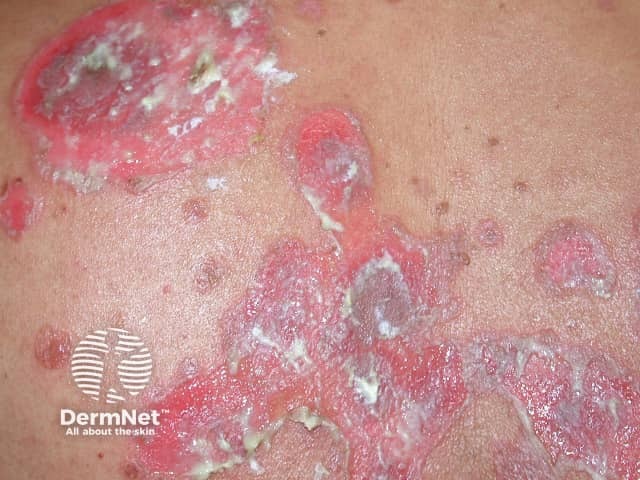
Pemphigus vulgaris
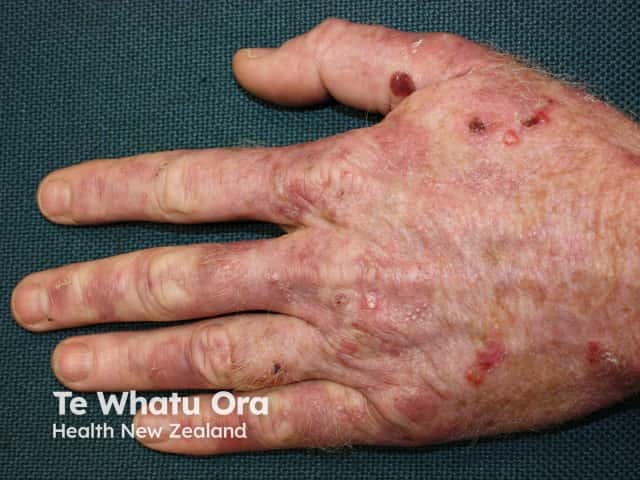
Porphyria cutanea tarda
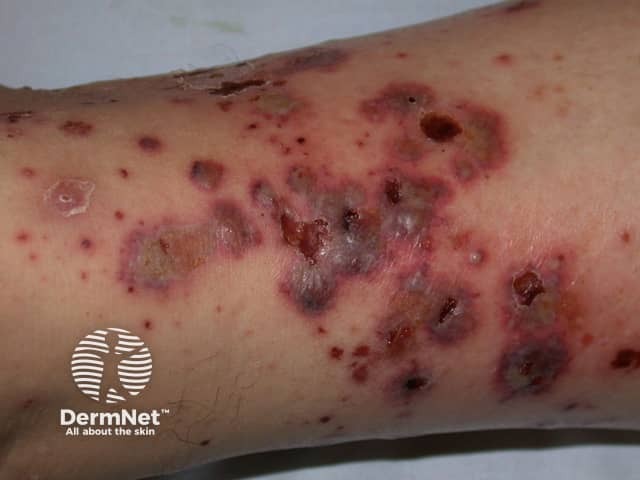
Cutaneous vasculitis
When an antibody binds to an antigen, it forms an antigen–antibody immune complex, and this activates the classical complement pathway.
C1 is a protein complex is made up of subunits C1q, C1s, and C1r.
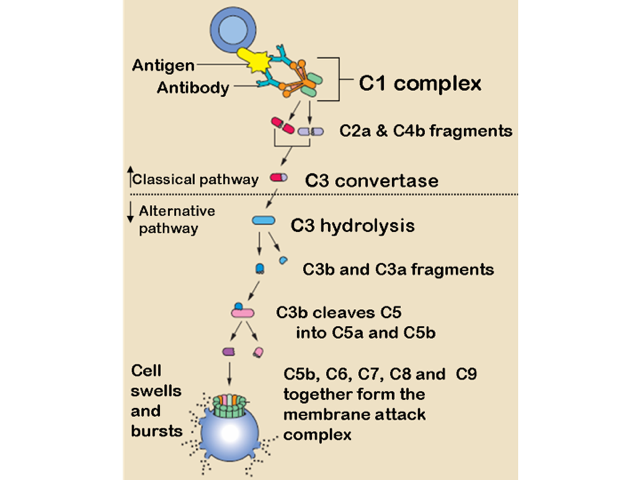
The complement pathway
The membrane attack complex is composed of C5b, C6, C7, and C8.
The alternate pathway does not require an antigen–antibody complex.
C3 spontaneously converts to C3a and C3b.
The C3b–Bb complex does two things.
A lectin is a protein that binds sugars such as mannose.
The mannose-binding lectin pathway involves two proteins:
MBL binds mannose on the surface of bacteria, which causes a conformation change in the structure of MBL that allows MASP to cleave C2 into C2a and C2b, and to cleave C4 into C4a and C4b [4].
C2b and C4b form C3 convertase and amplify the complement system (see alternate pathway).
There are regulators to stop the complement system being constantly activated.
Several skin conditions are associated with defects in the complement system [3].
Blistering skin diseases that involve defects in the complement system include:
Vascular diseases that involve defects in the complement system include:
Other inflammatory diseases that involve defects in the complement system include:
Complement levels can be measured by adding a serum sample into a solution with antigens. Any antibodies bind the antigens to form an immune complex which precipitates out of solution.
The components of the complement system are heat labile, therefore specimens sent for complement assays must be handled carefully. An abnormal result may be due to mishandling during transport of the specimen.