Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Vanessa Ngan, Staff Writer, 2006 Updated: Dr Georgia Morley, NHS, England. Copy edited by Gus Mitchell. April 2022
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Angioedema is a skin reaction similar to urticaria. It is characterised by an abrupt, temporary, localised swelling of the deep dermal layer, subcutaneous tissue, and mucous membranes. Although it can affect any part of the body, it most often occurs around the eyes, lips, and genitals. In severe cases, the internal lining of the upper respiratory tract and intestines may also be affected.
There are multiple types of angioedema, including allergic, drug-induced, idiopathic, and hereditary angioedema (HAE).
Urticaria is the development of transient localised oedema in the dermis, characterised by wheals and often co-exists with angioedema. Wheals are usually superficial skin-coloured or pale swellings, surrounded by erythema.
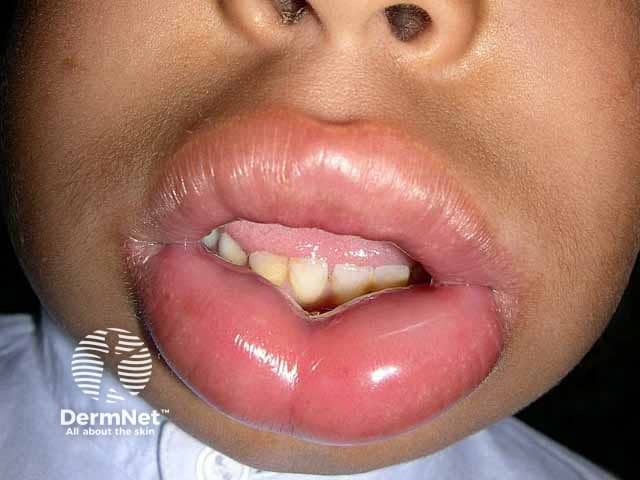
Severe lip angioedema
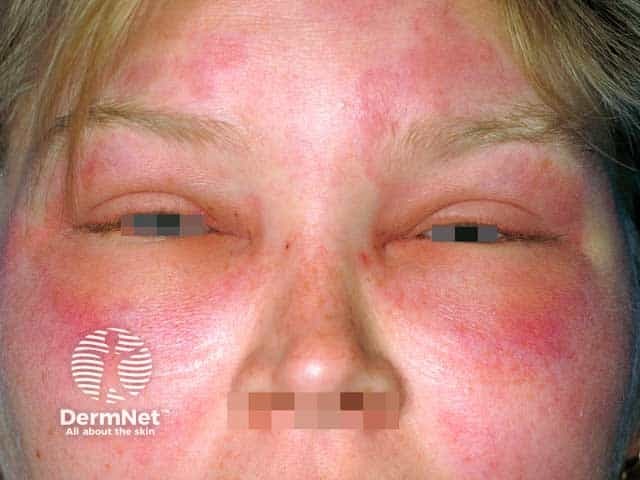
Lid angioedema - there was typical urticaria elsewhere on the body
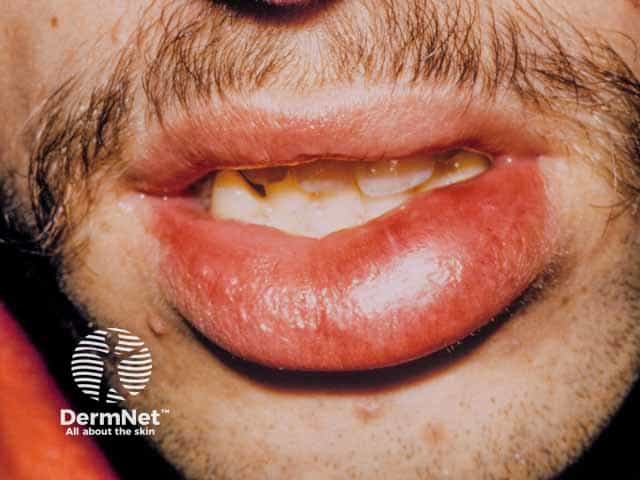
Resolving lip angioedema
Urticaria is a common skin presentation, affecting up to 20% of people; an estimated 40% of patients with chronic urticaria (lasting over 6 weeks) have associated angioedema. The prevalence of hereditary angioedema is estimated to be 1 in 500,000.
ACE-inhibitor induced angioedema is rare, however, it is the sub-type most likely to result in hospitalisation and is more common in African-Americans.
Angioedema is caused by an increase in local capillary permeability and plasma extravasation, usually mediated by mast cells, histamine, or bradykinin release.
Angioedema is most commonly histamine-mediated; mast cell and basophil stimulation results in histamine release. Angioedema with urticaria tends to suggest a histaminergic form, which includes acute allergic angioedema and histaminergic idiopathic angioedema. The exact cause depends on the type of angioedema a patient has.
Angioedema type |
Causes |
|---|---|
Acute allergic angioedema |
|
Non-allergic drug reaction |
|
Idiopathic angioedema |
|
Hereditary angioedema |
|
Acquired C1 inhibitor deficiency |
|
Inducible angioedema |
|
General features include:
Angioedema type |
Clinical features |
|---|---|
Acute allergic angioedema |
|
Non-allergic drug reaction |
|
Idiopathic/chronic angioedema |
|
Hereditary angioedema |
|
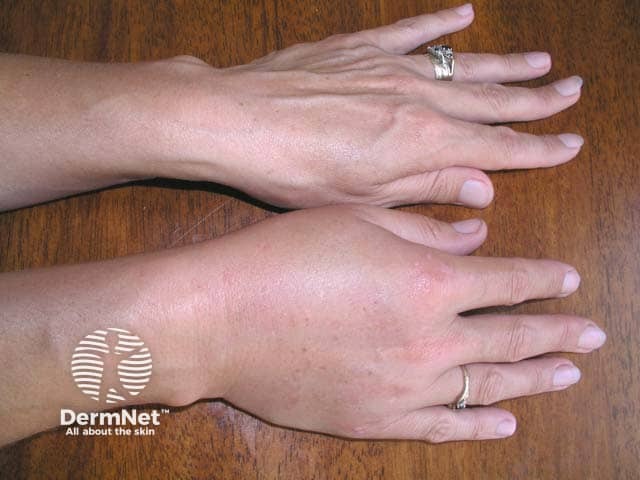
Angioedema of the right hand
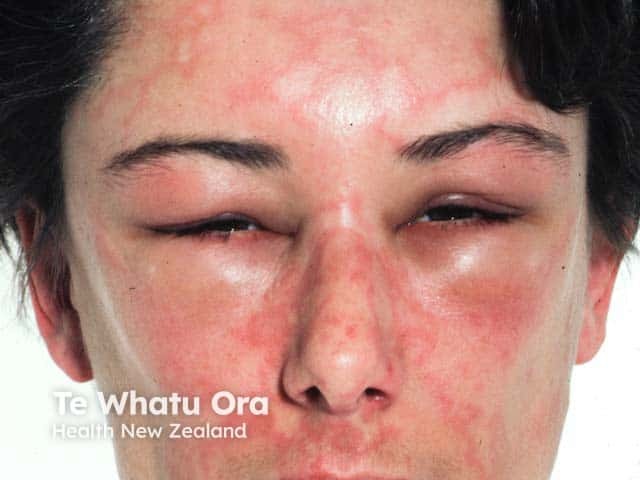
Angioedema and facial urticaria

Angioedema of the penis and prepuce
When angioedema is associated with urticaria, erythematous skin may appear purplish on darker skin tones.
Angioedema is usually diagnosed following clinical examination and detailed history taking. Important features include:
Examination of the patient is important for assessing severity and determining the likely cause.
If hereditary angioedema is suspected, testing can find low C4 and C1-INH levels (part of the complement system). However, cases of HAE with normal C4 levels have been reported.
Skin prick testing or RAST testing may be used when allergic angioedema is suspected.
Treatment is dependent on the subtype of angioedema. Angioedema is usually treated in the same way as acute urticaria when mild.
Treatment for HAE aims to decrease morbidity and mortality, and reduce the need for hospitalisation.
Acute presentations
Prophylaxis
For more information, see Hereditary angioedema.
The prognosis of angioedema is dependent on the presentation, severity and the initiation of, and response to appropriate treatment.
Mild symptoms often self-resolve within 72 hours. However, angioedema can be life-threatening, particularly after insect bites and stings, and in hereditary and ACE-inhibitor induced angioedema if there is airway involvement. This requires emergency assessment and intervention.