Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: November, 2024
Author(s): Dr Jessica Gartside, Medical Registrar, Gold Coast University Hospital, Australia (2024)
Peer reviewed by: Dr Sarah Winter, Dermatology registrar, Welsh Institute of Dermatology, Wales (2024)
Previous contributors: Vanessa Ngan, Staff Writer (2003)
Reviewing dermatologist: Dr Ian Coulson (2024)
Edited by the DermNet content department
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Diagnosis
Differential diagnoses
Treatment
Prevention
Outcome
Anaphylaxis is an acute, life-threatening, systemic hypersensitivity reaction that requires immediate diagnosis and treatment.
Signs and symptoms of anaphylaxis include urticaria, angioedema, respiratory compromise, hypotension, and gastrointestinal upset.
The estimated lifetime prevalence of anaphylaxis from all causes is between 0.05-2% in the general population, and the rate of occurrence is increasing. Mortality remains low, estimated at 0.05–0.51 per million people/year for drugs, at 0.03–0.32 for food and at 0.09–0.13 for venom-induced anaphylaxis.
Mechanisms of anaphylaxis can be classified as:
Any food, insect sting or bite, or medication can potentially trigger this severe reaction. The topical application of a drug to the skin or mucosae, oral, intramuscular or intravenous route, eye drops, or inhalers can all induce anaphylaxis. Antibiotics and antiseptics contained in implants and intravenous lines can also be implicated.
Insect stings
Other causes
Food-induced anaphylaxis often produces skin reactions and respiratory symptoms while drug- or venom-induced anaphylaxis more often produces shock. Symptoms usually occur within 5–60 minutes of contact with the allergen, but sometimes happen after several hours, or even 3–4 days later. Fast onset and rapid progression of symptoms usually indicate severe, life-threatening anaphylaxis. One or more organ systems may be involved.
Typical features include the following:
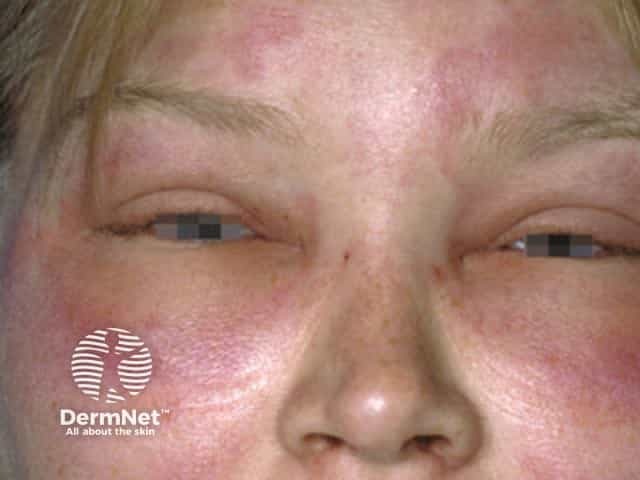
Acute angioedema of the face and lids during an attack of anaphylaxis
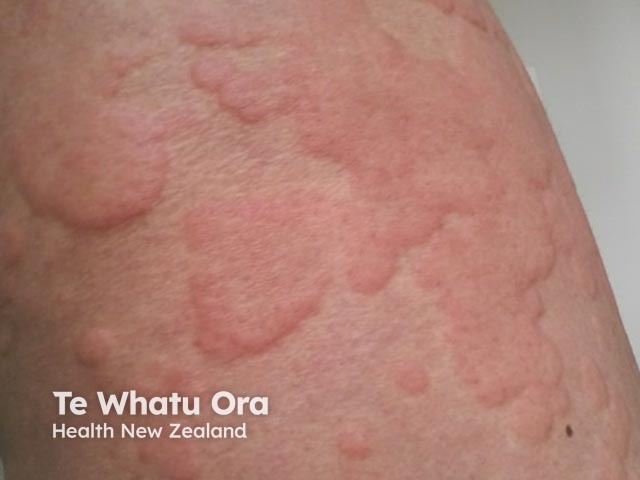
Severe acute urticaria during an anaphylactic attack
Temporal patterns of anaphylaxis include uniphasic (most common), biphasic, protracted, refractory, and delayed. After apparent initial recovery, up to 3-20% of patients may relapse (biphasic response).
See Urticaria and Angioedema
As per the World Allergy Organisation (WAO), anaphylaxis is highly likely when either one of the following two criteria are fulfilled:
Any acute onset of hypotension or bronchospasm or laryngeal involvement after exposure (minutes to several hours) to known or probable allergen, even if typical skin features are not present
Any acute onset illness with simultaneous involvement of the skin, mucosal tissue, or both (eg, generalised hives, pruritus or flushing, swollen lips-tongue-uvula) PLUS involvement of respiratory, cardiovascular, or persistent severe gastrointestinal symptoms (see WAO for specific details).
Serum tryptase measurements should be obtained (ideally within 2 hours of the episode) and reviewed. Elevated tryptase levels support a diagnosis of anaphylaxis, however normal levels do not exclude anaphylaxis.
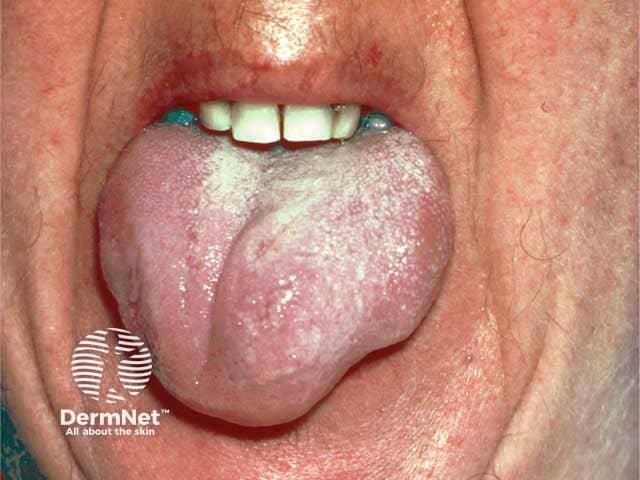
Severe lingual angioedema in acquired C1 esterase inhibitor deficiency
Prompt recognition and prompt treatment is critical in anaphylaxis. Stop delivery of any potential causative agent. Acute anaphylaxis must be treated as a medical emergency requiring hospitalisation for continued assessment and stabilisation of airway, breathing and circulation.
Lay the person flat, and do not allow them to stand or walk. Early and definitive treatment of suspected anaphylaxis with intramuscular adrenaline (epinephrine) 0.01mg/kg, to a max dose of 0.5mg IM in adults (0.5mL of 1:1000 adrenaline using an autoinjector or syringe), or as outlined by local protocol is indicated. Repeat IM adrenaline dose every 5 minutes as required. Additional treatments include supplemental oxygen, intravenous fluids, antihistamines, and intravenous corticosteroids.
Patients taking beta-blockers may respond poorly to adrenaline, with persistent hypotension and bradycardia.
Prevention is the best medicine. All those at risk of anaphylaxis should wear a Medic Alert/emergency bracelet with full details of allergies and contact details of their doctor. In some cases, a patient or caregiver should always carry an emergency kit containing self-injectable adrenaline and antihistamine tablets. Strict allergen avoidance should be adhered to.
The prognosis of anaphylaxis is unpredictable. It can be life-threatening; hence all anaphylactic reactions are considered medical emergencies that require emergency treatment. Fortunately, the majority of anaphylactic reactions do not result in severe outcomes and mortality from anaphylaxis remains low.