Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Matthew James Verheyden, Junior Medical Officer, Royal North Shore Hospital, Sydney, NSW, Australia; Dr Claudia Hadlow, Junior Medical Officer, John Hunter Hospital, Newcastle, NSW, Australia; Dr Monisha Gupta, Senior Staff Specialist, Liverpool Hospital; Conjoint Senior Lecturer, UNSW; VMO, The Skin Hospital, NSW, Australia. DermNet Technical Editor: Elaine Luther, Medical Student, Ross University School of Medicine, Barbados. DermNet Editor in Chief: Adjunct A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. February 2020.
Introduction - urticaria
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Urticaria is commonly called hives, a skin reaction characterised by weals, which are caused by the release of histamine and other vasoactive substances from mast cells. Oedema is located in the superficial dermis in urticaria, whereas the swelling is deeper in the skin in angioedema.
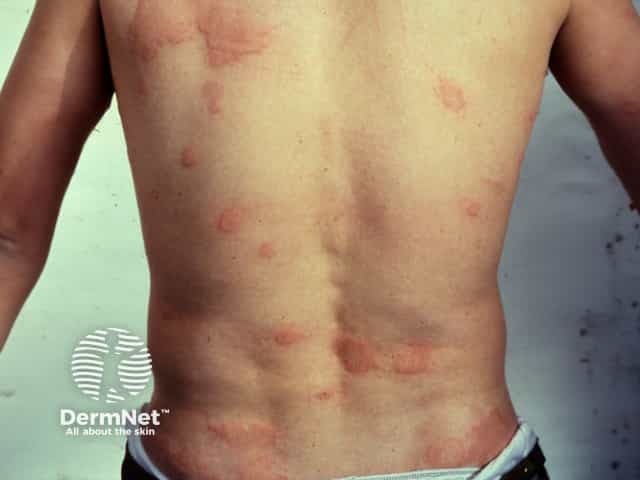
Urticaria
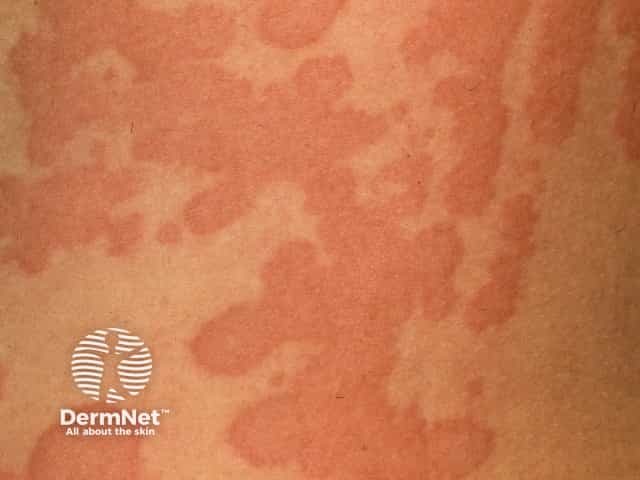
Urticaria
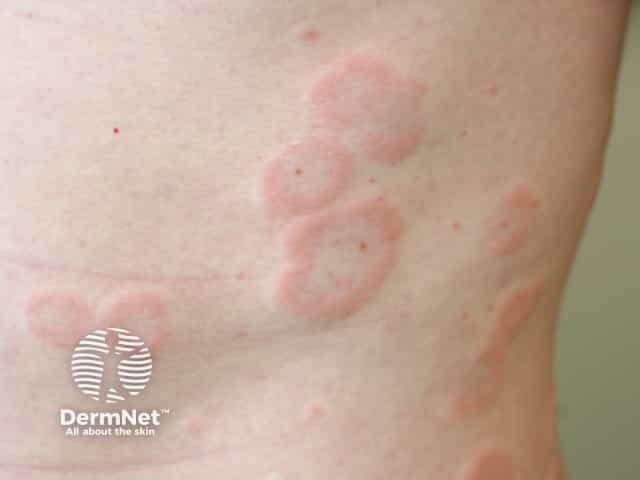
Drug-induced urticaria is the term used when urticaria is caused by a drug, most often penicillin, a non-steroidal anti-inflammatory agent (NSAID), or sulfamethoxasole in combination with trimethoprim (see Sulfa drugs and the skin). The drug may be ingested or applied to the skin surface (contact urticaria).
The clinical features and treatment for drug-induced urticaria are identical to those for urticaria not related to drugs. It can be associated with angioedema, anaphylaxis, and serum sickness.
Drugs are capable of inducing three subtypes of urticaria:
Acute urticaria is less than six weeks’ duration and is often gone within hours to days.
Chronic urticaria is greater than six weeks’ duration, with daily or episodic weals.
Drug-induced urticaria is sometimes called urticaria medicamentosa.
Urticaria is one of the most common drug-induced skin eruptions, second only to morbilliform eruption. In outpatient dermatology clinics, drug-induced urticaria is estimated to affect 9% of patients presenting with urticaria. There does not appear to be any relationship to sex or race.
Drug-induced urticaria can be mediated by immune or non-immune mechanisms related to the administration or contact with a drug.
Immune mechanisms are allergic reactions mediated by the immune system (see Allergies explained) and include urticaria due to type I hypersensitivity (IgE dependent) and type III hypersensitivity (immune complex-mediated).
Non-immunological mechanisms are pseudo-allergic reactions and are not dependent on the immune system. Non-immunological mechanisms include the direct release of mast cell mediators, an effect on the cell membrane, and activation of the complement system without immunoglobulin.
Drugs that are known to cause urticaria are listed below. The drugs marked with an asterisk (*) are strongly associated with urticaria.
The clinical features of drug-induced urticaria are identical to urticaria that is not related to drugs. The severity of the reaction can be variable.
Urticaria can affect any site of the body and tends to be widely distributed. The trunk is most commonly affected, though this is not specific to drug-induced urticaria. The palms, soles, and scalp can also be affected.
Lesions are typically intensely pruritic and can induce a burning sensation. Urticaria is classified according to its duration.
In acute drug-induced urticaria, weals appear within a few hours to a few days after the administration of the drug. They usually disappear within several days of drug cessation.
In chronic drug-induced urticaria, a prolonged relapsing-remitting course is often observed, with the urticaria resolving from time to time.
In contact urticaria, lesions are localised to the site of application, though on occasion the urticarial lesions can become generalised to the rest of the body. Contact urticaria develops within minutes to hours of application of a topical agent and resolves within a couple of hours of removal of the cause.
Drug-induced urticaria can be more severe and serious than spontaneous urticaria resulting in hypotension, dyspnoea, and anaphylaxis.
Persistent urticaria can have a substantial impact on the quality of life.
The diagnosis of drug-induced urticaria requires a comprehensive clinical history. If necessary, the diagnosis can be confirmed by prick testing, immunoglobulin E tests, and oral provocation tests. Other investigations can include haematology, tryptase, complement (C3/C4, C3d), leukocyte histamine release, and urinary tryptase. These tests are not always reliable and often a decision must be made clinically.
Drug-induced urticaria can be confused with many conditions, which include:
Note that angioedema can present years after starting acetylcholinesterase (ACE) inhibitors. This is not accompanied by urticarial weals.
The causative drug should be stopped when possible. If due to a type 1 (IgE-mediated) allergy, the urticaria clears within 48 hours. See Allergies explained.
Non-essential medications should be avoided if they may be contributing to the urticaria.
Cooling the affected area with a fan, cold flannel, ice pack, or soothing refrigerated moisturising lotion may provide relief.
The main pharmacological treatment for acute urticaria is an oral second-generation antihistamine such as cetirizine, loratadine, fexofenadine, desloratadine, or levocetirizine. If the standard dose (eg, 10 mg for cetirizine) is not effective, the dose may be increased fourfold (eg, 40 mg cetirizine daily). Continue treatment until the urticaria is well controlled, and then gradually reduce the dose of the antihistamine. A second type of antihistamine provides no additional benefit.
Although systemic treatment is best avoided during pregnancy and breastfeeding, there have been no reports of birth defects due to second-generation antihistamines. If treatment in pregnancy is required, loratadine and cetirizine are currently preferred.
Conventional first-generation antihistamines such as promethazine or chlorpheniramine are not recommended for urticaria.
If non-sedating antihistamines alone are not effective, a four- to five-day course of oral prednisone or prednisolone (systemic corticosteroids) might be added in severe acute urticaria, particularly if there is angioedema. However, systemic corticosteroids do not speed up the resolution of symptoms. Steroids are best avoided for long-term therapy due to their adverse effects and the risk of rebound when they are discontinued.
Intramuscular adrenaline (epinephrine) is reserved for cases with life-threatening anaphylaxis or swelling of the throat.
Patients who have had true drug-induced urticaria due to type 1 hypersensitivity will have another attack — possibly worse — if re-exposed. Patients should be advised to wear a medical alert bracelet and to inform their healthcare providers about their adverse reaction to the causative drug.
Patients who have been sensitised to a class of medication can, in certain cases, cross-react with another drug of the same class. Substitution with a drug from another class should be considered if the clinical need emerges.
Desensitisation is rarely performed for drug-induced urticaria.