Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction Demographics Causes Clinical features Diagnosis Treatment
Contact urticaria is an immediate but transient localised swelling and redness that occurs on the skin after direct contact with an offending substance. Contact urticaria should be distinguished from contact dermatitis where a dermatitis reaction develops hours to days after contact with the offending agent.
Contact urticaria can be immunological (due to allergy) or non-immunological. It is a form of inducible urticaria and can be acute or chronic.
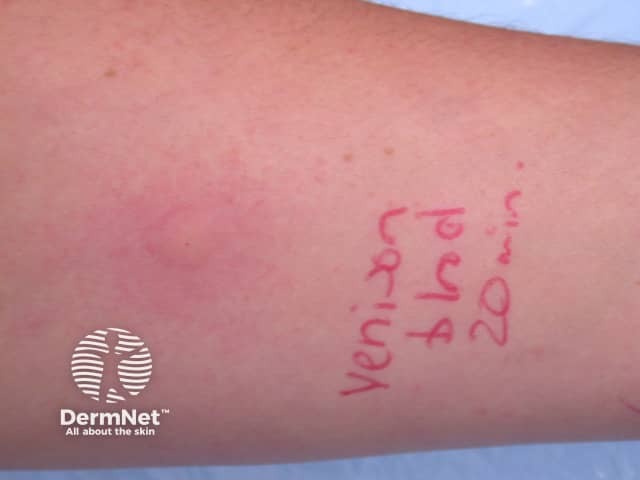
Venison reaction
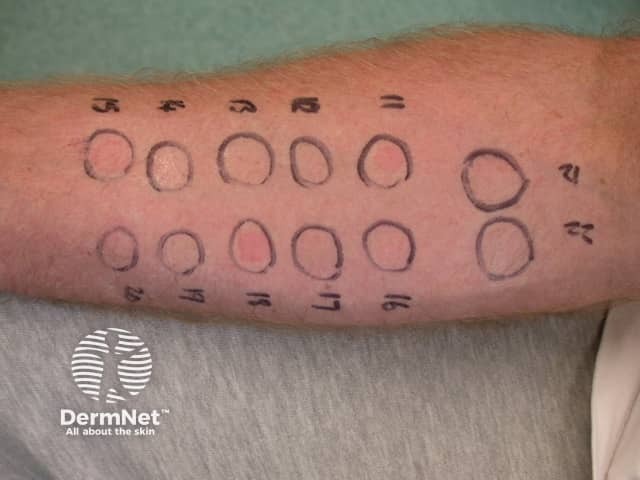
Prick testing
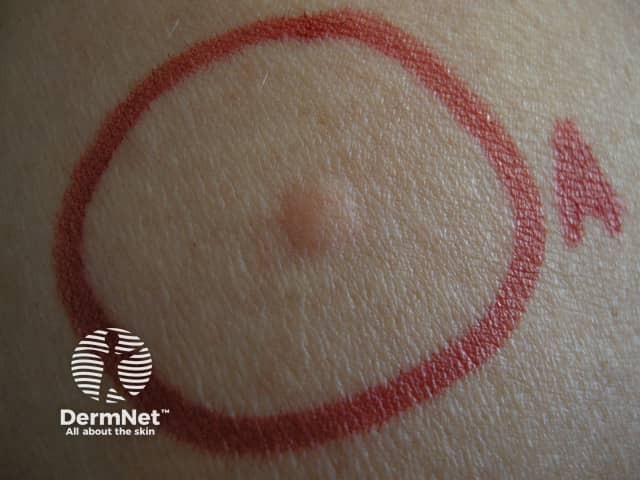
Latex reaction
See more contact urticaria images
Anyone is able to get contact urticaria, however, there are some groups of people that are at increased risk for the condition to occur. Occupational groups at risk and the substances that cause contact urticaria are listed below. In most cases, exposure has occurred over time and the response is of the immunological type of contact urticaria.
Contact urticaria is caused by a variety of compounds, such as foods, preservatives, fragrances, plant and animal products, metals, and rubber latex. The mechanism by which these provoke an immediate urticarial rash at the area of contact can be divided into two categories: non-immunological contact urticaria and immunological (allergic) contact urticaria.
Commonly reported causes of the different types of contact urticaria are shown below.
Contact urticaria reactions appear within minutes to about one hour after exposure of the offending substance to the skin. Signs and symptoms of affected skin areas include:
Signs and symptoms may occur in other organs other than the skin. These are known as extracutaneous reactions and are more likely to occur in patients with immunological contact urticaria. Features of extracutaneous reactions include:
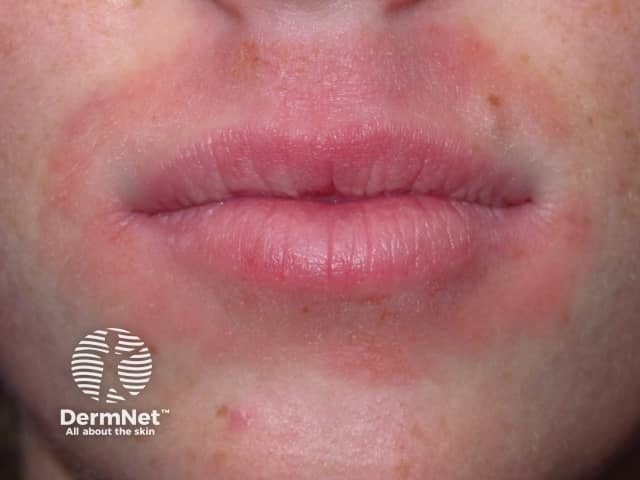
Periroral contact urticaria

Wheal in dark skin
Sometimes it is easy to recognise contact urticaria and no specific tests are necessary. RAST tests (specific IgE blood test) where available, can be used to confirm the allergy. Skin prick test and scratch patch tests confirm the diagnosis of contact urticaria but do not differentiate between allergic and non-allergic mechanisms.
The patient should have an understanding of the nature of their urticarial reaction (non-immunological vs immunological). Patients with immunological contact urticaria should wear medical alert tags and be aware of the potential life-threatening reactions of the condition.
In most cases, the rash rapidly clears up completely once the offending substance is no longer in contact with the skin.
The main aim of treatment is to avoid the substances that cause the urticarial reaction and find suitable alternatives. Gloves may be used to protect hands from contact with materials of concern, but avoid rubber gloves if allergic to latex.
Medications that may be used to minimise the reaction include antihistamines and adrenaline for more severe reactions.