Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu, MD candidate, Keck School of Medicine, Los Angeles, USA. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. December 2016.
Introduction
Occupational risks
Occupational skin disorders
Workplace risk assessment
Diagnosis and treatment
Veterinarians and veterinary nurses provide an important service globally for pets, agricultural stock, service animals and exotic animals. However, the nature of veterinary work puts these professionals at risk for a variety of job-related skin disorders. Safe Work Australia, part of the Australian Government’s occupational health and safety service programme, listed veterinary work as being in the top 20 professions in regard to rates of skin disorders and skin disease.
Factors that contribute to the high-risk nature of veterinary work include:
Occupational skin disease is an umbrella term that refers to dermatological conditions that develop or are exacerbated by the nature of an individual’s work. Occupational skin disorders and skin diseases are the most common form of work-related health disorder. Allergic contact dermatitis or irritant contact dermatitis account for about 79–90% of occupational skin disorders. Occupational skin disorders have a strong economic impact due to missed days of work, medical costs, workers’ compensation and sometimes a need to change professions due to treatment-resistant skin disorders. Dermatoses develop when the nature of a person’s work breaches the natural barriers of the skin and makes the skin more vulnerable to breakdown and/or infection.
Contact dermatitis is a frequent complaint among veterinary workers.
Animal bites are common in veterinary practice.
Mechanical injury is another common risk for veterinary workers. This is largely due to use of syringes, lancets and other sharps.
Common fungal infections include tinea corporis (ringworm) and blastomycosis.
Veterinarians may be prone to other specific infections associated with agriculture and animal husbandry. Examples include:
Sun exposure or sunburn is another occupational hazard for veterinary workers.
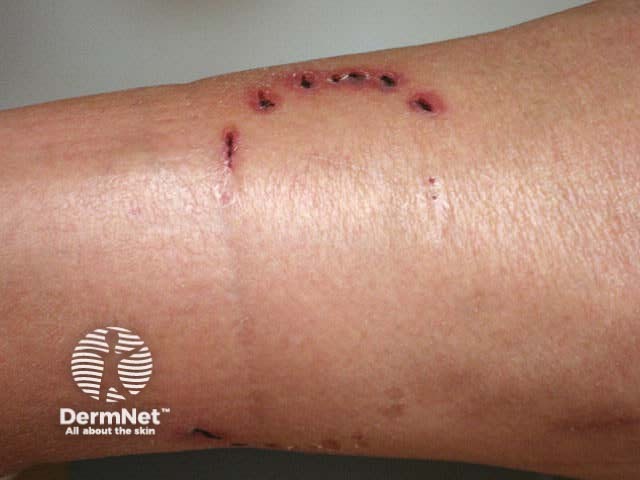
Dog bite
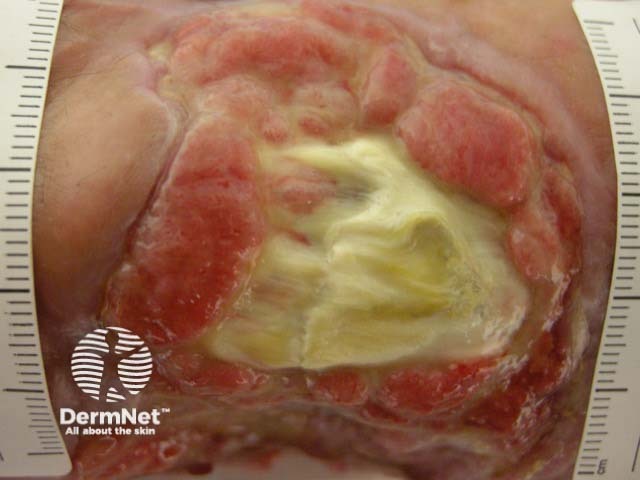
Dog bite
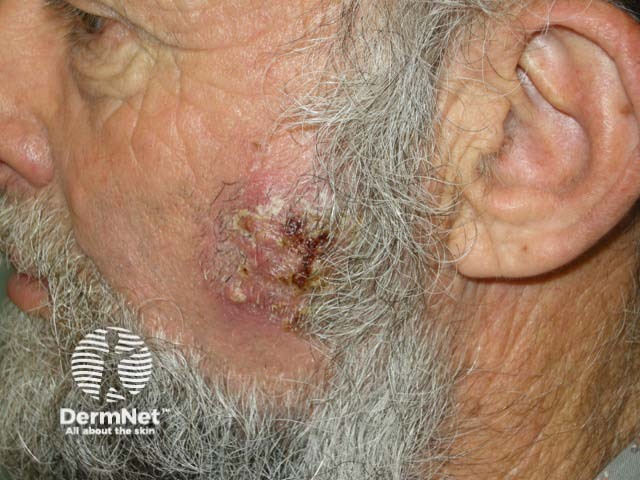
Kerion due to cattle ringworm
In order to provide a safe environment for veterinary workers, a workplace risk assessment should focus on:
Personal protective equipment for workers in a veterinary clinic should include the following:
In order to be effective, veterinary employees must be educated on the proper donning, use and disposal of personal protective equipment.
Good hand care is important to the health of veterinarians and veterinary nurses and may include:
The diagnosis of an occupational skin disorder should be based on:
Treatment can include: