Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Reviewed and updated by Dr Amanda Oakley Dermatologist, Hamilton, New Zealand; and Vanessa Ngan, Staff Writer; June 2014.
Introduction
Demographics
Clinical features
Complications
Investigations
Differential diagnoses
Treatment
Prevention
Anthrax is a serious bacterial infection caused by Bacillus anthracis. Untreated, up to one-fifth of infected individuals die of the disease. Prompt treatment with antibiotics is curative and most recover fully.
Anthrax is also called wool sorter's disease, splenic fever, charbon, and milzbrand.
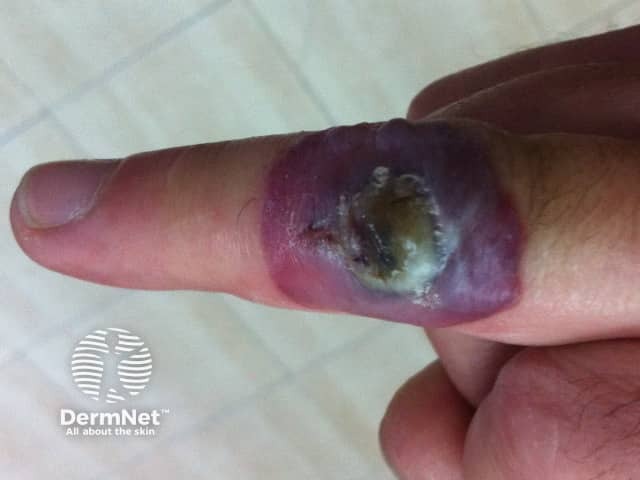
At diagnosis
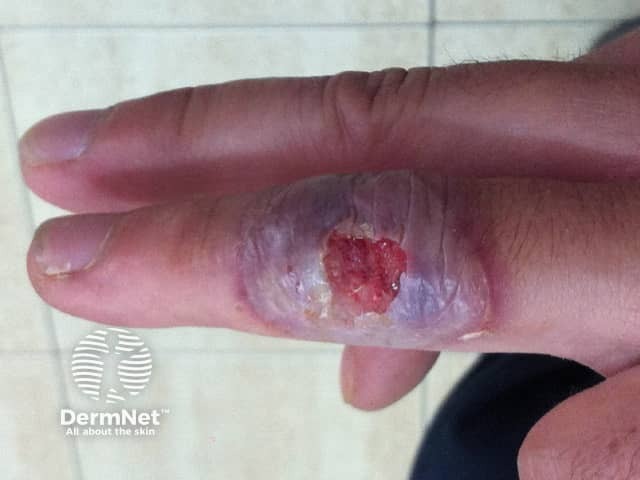
6 days later
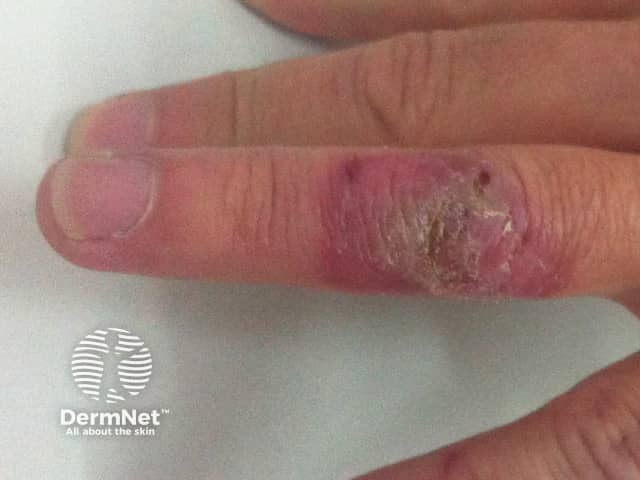
4 weeks after diagnosis
Anthrax is extremely rare in the developed world but sporadically occurs among farmers in Africa, the Middle East and the Caribbean. It can also infect workers in the wool, hair or bristle industries, butchers and gardeners.
Anthrax primarily affects sheep and cattle that ingest spores lying dormant in the pasture. Human infection can arise from spores entering the skin by inoculation through a minor injury, through the lungs by inhalation (wool sorter's disease) or by ingestion. Most anthrax infection (95%) is via the skin (cutaneous anthrax).
Cutaneous anthrax develops usually between 1-7 days after skin exposure.
The infection occasionally results in a red streak tracking to nearby lymph glands (lymphangitis). These lymph nodes then often swell and become sore.
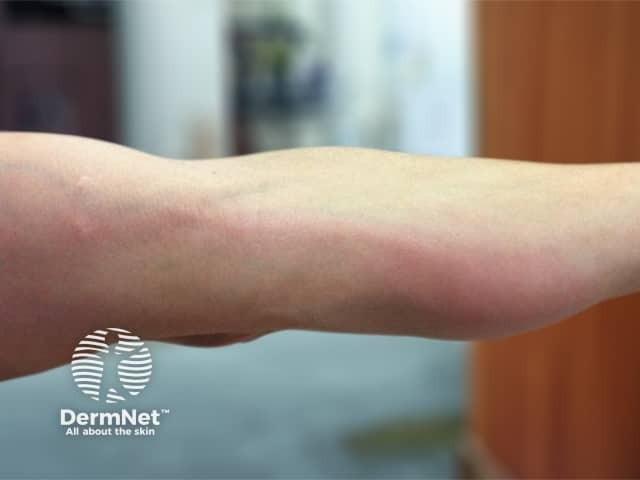
Lymphangiitis due to anthrax
Anthrax becomes dangerous if it spreads widely through the bloodstream. The risk of anthrax spreading through the body is higher if the infection is acquired by inhalation or ingestion.
Symptoms of this include fever, headache and weakness. In mild cases, recovery occurs within three weeks.
In severe infection, prostration, delirium, collapse and death often occur.
The appearance of anthrax can mimic the skin infections due to staphylococci and streptococci, and much less common viral infections due to cowpox, orf and cat scratch disease.
Cutaneous anthrax is treated with antibiotics. Treatment must be started straight away to reduce the chance of the anthrax spreading from the initial skin lesion.
In some cases, it is necessary to surgically scrape off the black eschar from the anthrax ulcer. It is essential that this is done with antibiotic cover as interfering with the wound could encourage the spread of the bacteria. If the eventual scar is unsightly, a plastic surgeon may be able to improve its appearance later.
A newer treatment for inhalational anthrax is the monoclonal antibody raxibacumab. It is used as part of combination therapy with appropriate antibiotic agents.
Anthrax spores can survive for over 20 years in dry pasture and soil. Precautionary measures people can take include:
For people who have been exposed to anthrax but don’t have symptoms, prophylactic treatment with an antibiotic should be given to reduce the risk of infection. A 60-day oral course of penicillin, tetracycline or quinolone is recommended.