Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Claudia Hadlow, Medical Student, University of Notre Dame Australia, Sydney, NSW, Australia; Matthew James Verheyden, Medical Student, University of Notre Dame Australia, Sydney, NSW, Australia; Dr Tevi Wain, Consultant Dermatologist, The Skin Hospital, Westmead, NSW, Australia. DermNet Editor in Chief: Adjunct A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. November 2019.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Aquagenic urticaria is a rare variant of chronic inducible urticaria induced by contact with water.
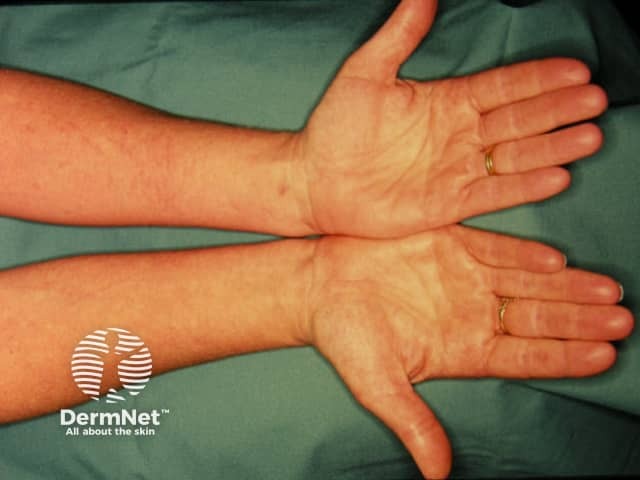
Aquagenic urticaria
Less than 100 cases of aquagenic urticaria have been reported in the medical literature. There is a higher prevalence among females, with the typical age of onset during or after puberty. Most cases have occurred sporadically, but several familial cases have also been reported.
The exact pathogenesis of aquagenic urticaria is not yet known, but a number of hypotheses have been proposed.
Water reacts with unknown components within the skin, causing histamine release from mast cells and the formation of an urticarial rash. Triggers may include:
Aquagenic urticaria appears whatever the water temperature, saltiness, or pH, and is not dependent on psychogenic factors.
Skin contact with water results in symptoms within 20–30 minutes.
Rarely, the patient may also experience systemic symptoms of wheezing and shortness of breath.
Intense or prolonged itching results in excoriations that can be secondarily infected and start to ulcerate and scar.
Patients with aquagenic urticaria may suffer from psychological stress due to a fear of water.
A clinical history of urticaria in response to water exposure is suspicious of aquagenic urticaria, but the diagnosis should be confirmed by a positive water provocation test and exclusion of other types of chronic inducible urticaria.
A water provocation test can be performed to test for aquagenic urticaria using the following method:
To exclude cholinergic urticaria, examine for urticaria after an exercise test to raise the core body temperature. Other physical urticarias to exclude on testing include pressure urticaria, cold urticaria, and heat urticaria.
Aquagenic urticaria must be distinguished from other forms of inducible urticaria, including:
As it is impossible to avoid water completely, treatment is aimed at preventing or minimising symptoms induced by contact with water.
The main treatment is to take a daily non-sedating, second-generation H1 antihistamine, such as cetirizine, loratadine, or fexofenadine prophylactically.
Other reported treatments include:
The rate of remission of aquagenic urticaria is unknown.