Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Georgia Moore, Junior Medical Officer, The Wollongong Hospital, Wollongong, NSW, Australia; Dr Monisha Gupta, Dermatologist, The Skin Hospital, Sydney, NSW, Australia. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. June 2019.
Introduction Demographics Causes Clinical features Diagnosis Differential diagnoses Treatment Outcome
Heat urticaria is a rare type of physical or chronic inducible urticaria. It is also called contact heat urticaria and localised heat urticaria.
Heat urticaria occurs following the direct contact of a warm stimulus to the skin. The onset of urticaria is typically rapid (within minutes) and the urticaria resolves within 1–2 hours. It can also cause angioedema and systemic symptoms.
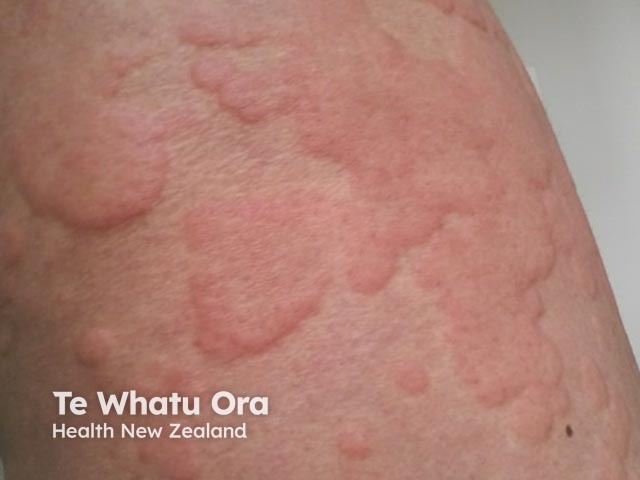
Urticarial weals
Heat urticaria is very rare, with few reported cases, so the exact prevalence is unknown. In one family, delayed heat urticaria was inherited in an autosomal dominant pattern (one parent had the condition and passed on the condition). Most reported patients have been women aged 20–45 years, with familial cases having onset during childhood.
Chronic inducible urticaria, in general, has an estimated prevalence of 0.5% and predominantly occurs in women, at a rate of 74% of those afflicted. People with heat urticaria may develop another type of inducible urticaria such as cold urticaria or dermographism.
Examples of stimuli that may cause heat urticaria may include:
The exact development process of heat urticaria is unknown. Heat on the skin activates mast cells to release proinflammatory mediators, mainly histamine. This causes small vessels in the skin to dilate, leading to a localised area of swelling, erythema, and wealing.
Unlike cholinergic urticaria (a heat-related urticaria caused by sweating), heat urticaria does not involve the activation of cholinergic (sweat) glands and it is independent of the whole core body temperature.
The clinical features of heat urticaria are usually confined to the area affected by the heat stimulus. There are three clinical subtypes of heat urticaria.
Immediate localised heat urticaria is the most common type and presents as large, well-circumscribed, itchy weals.
Some patients with heat urticaria develop generalised wealing if exposed to a hot environment.
Delayed heat urticaria presents as weals that cause an itch or burning sensation.
Heat urticaria is typically diagnosed by the clinical features of a localised area of urticaria following the application and removal of a heat stimulus to the skin.
The diagnosis is confirmed by provocation tests. A warm stimulus (a test tube with water > 44° or a heated cylinder) is applied to the inner forearm. Urticaria develops typically within minutes after the warm stimulus has been removed. The test can be repeated using different temperatures to determine sensitivity to heat and to monitor treatment response.
Heat urticaria must be differentiated from cholinergic urticaria (generalised heat urticaria) in that it is localised to the skin in contact with the heat stimulus and doesn’t involve the activation of sweat glands systemically.
Urticaria is a common symptom and can result from many precipitating or unknown causes, as described below.
It is important to identify and avoid the triggering factors for heat urticaria.
Antihistamines tend to be less effective for heat urticaria than for other forms of urticaria.
First-line treatment is a non-sedating second-generation H1 antihistamine, such as cetirizine or loratadine 10 mg daily. If symptoms persist, the dose is increased, up to four times the standard dose each day. This is at least somewhat effective for about 60% of patients with heat urticaria.
Possible additional options may include:
Chronic inducible urticaria overall has a long duration, with lower rates of remission at 1 year when compared to chronic spontaneous urticaria. The impact on quality of life can be significant.