Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction
Classification
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Urticaria refers to a group of conditions in which weals (hives) or angioedema (swelling) develop in the skin. It is very common in children.
A weal is a superficial swelling, usually pale or skin-coloured. It is often surrounded by an area of erythema and can last from a few minutes to 24 hours. Children will usually complain of itch and sometimes of a burning sensation.
Angioedema is a deeper swelling from within the skin or mucous membranes. It usually looks red and puffy. The most common areas for angioedema in children are the lips, tongue, and eyelids.
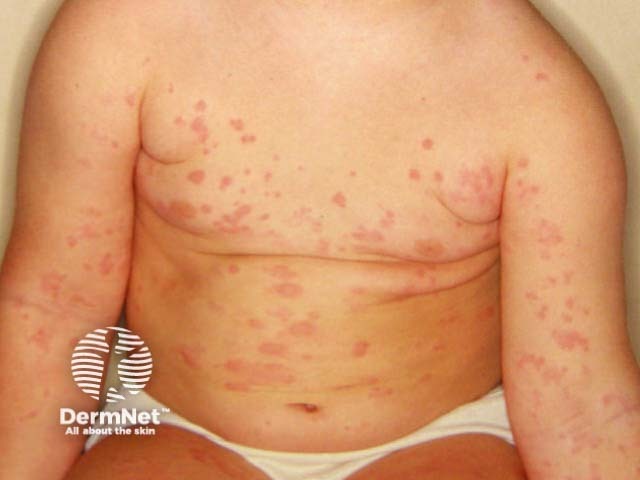
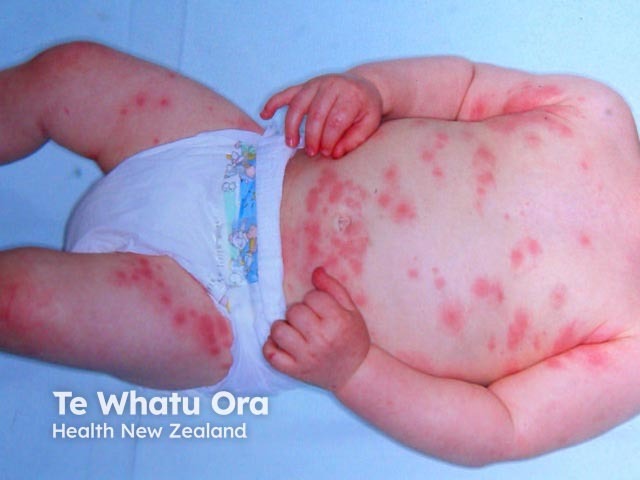
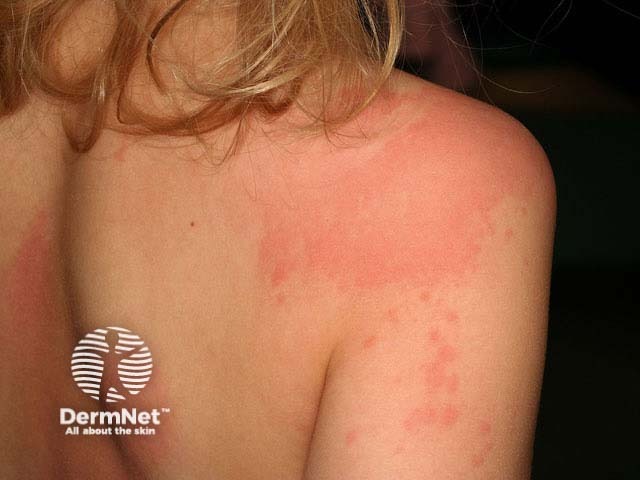
Urticaria in children can be either acute (often gone within hours to days) or chronic (lasting longer than 6 weeks). In children, acute urticaria is much more common than chronic urticaria. About 40% of children with acute urticaria also have angioedema.
Chronic urticaria can be spontaneous (when weals occur without any specific trigger) or inducible (when weals occur with a specific trigger).
Chronic inducible urticaria is classified by the various physical triggers, such as dermographism (stroking or scratching the skin).
Approximately 15% of all children under 10 years of age will have at least one episode of acute urticaria. The risk is slightly higher for girls than for boys. However, if a child is atopic (has asthma, dermatitis, and allergies), this risk is around 20%.
Weals are caused by a number of chemical mediators, such as histamine and cytokines, which are released from inflammatory cells, including mast cells. The mediators cause vasodilation and leakage of fluid into surrounding tissues to produce the redness and swelling of urticarial weals.
Triggers of acute spontaneous urticaria can include:
There is no obvious trigger in approximately 50% of cases of acute urticaria. This may be called ‘idiopathic’ urticaria.
Chronic urticaria is usually caused by autoimmunity or a chronic underlying infection. It is rare in children.
Inducible urticaria is caused by a direct stimulus, such as dermographism, delayed pressure, cold, heat, sunlight, vibration, or exercise. It is linked with atopy and chronic urticaria, but the pathogenesis is not fully understood.
Urticarial weals may appear on any part of the body and are often very itchy. They can vary in size from the size of a pinpoint to several centimetres in diameter. They are either white or red and can be either localised or widespread. Weals change shape and size and each one lasts from a few minutes to several hours.
Angioedema is usually localised to a single area such as the hands, feet, and genitalia. It most commonly affects the face in children. The child may have a swollen tongue, eyelids, or lips. Angioedema is often tender or painful.
Inducible urticaria due to a physical stimulus often comes on within minutes after exposure and resolves in less than an hour. The weals will be localised to the exposed site. Angioedema is exceptionally rare in these cases.
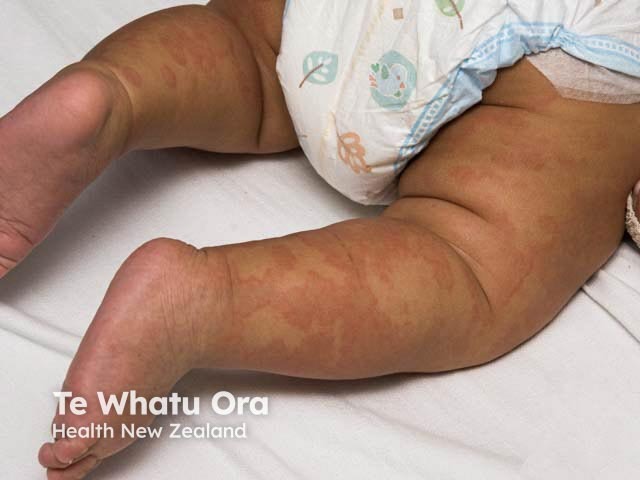
Acute urticarial rash in skin of colour
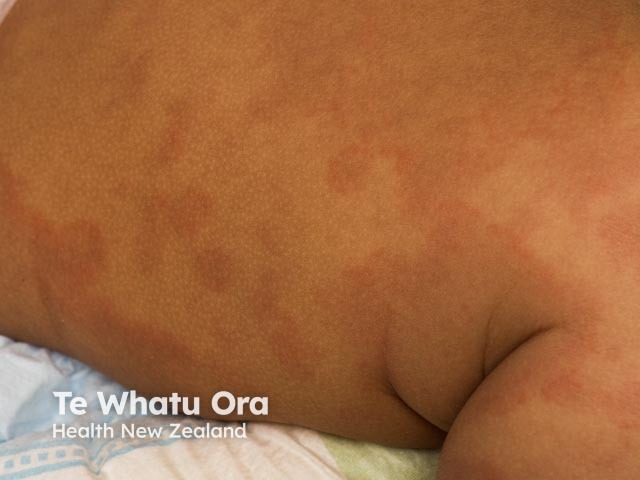
Acute urticarial rash in skin of colour
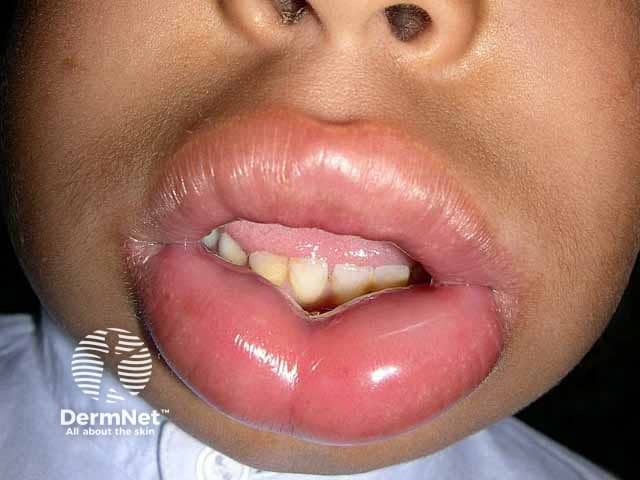
Severe lip angioedema
Urticaria is usually self-limiting and will go away on its own. However, it can often be very uncomfortable for a child due to the intense itchiness. There are usually no serious long-term consequences for children.
Urticaria may be a component of anaphylaxis (severe allergic response). If the child is also struggling to breathe, wheezing, collapses, or seems unwell, seek urgent medical attention.
Urticaria is usually diagnosed by taking a medical history. Urticaria is characterised by individual weals resolving or changing within 24 hours. The child should be thoroughly examined to detect possible causes.
If a food or drug allergy is suspected, a skin prick test or immunoglobulin E (IgE) tests may occasionally be arranged to investigate further.
The differential diagnosis for urticaria in children includes a variety of infections and skin conditions.
Urticaria in children is treated with a non-sedating antihistamine, such as cetirizine. This is not curative, but often controls the itch and the spread of weals until the urticaria settles on its own.
Dosage recommendations based on age groups are as follows:
In severe cases that are unresponsive to antihistamines, oral prednisone may be given for a few days.
Children may also be advised to avoid triggers such as foods or drugs, cold or heat.
The itch may be reduced by cooling with a fan, ice pack, or moisturising lotion.
If there is life-threatening anaphylaxis, an intramuscular injection of adrenaline is advised.