Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2006. Updated by A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, January 2016.
Urticarial vasculitis is a variant of cutaneous small vessel vasculitis. It is characterised by inflamed and reddened patches or weals on the skin that appears to resemble urticaria, but when the skin is examined closely under a microscope, a vasculitis is found (inflamed blood vessels).
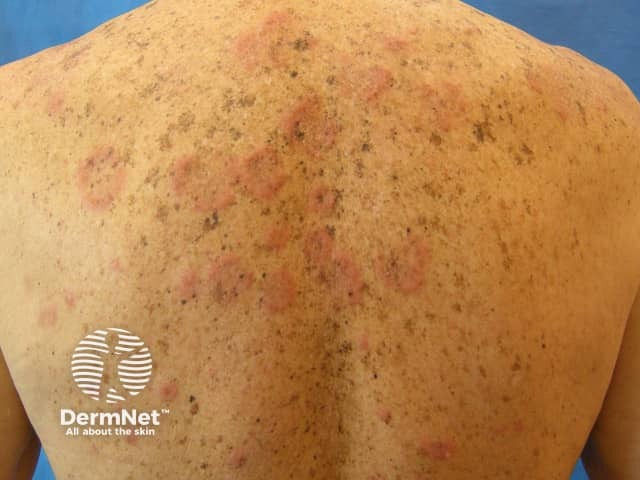
Urticarial vasculitis
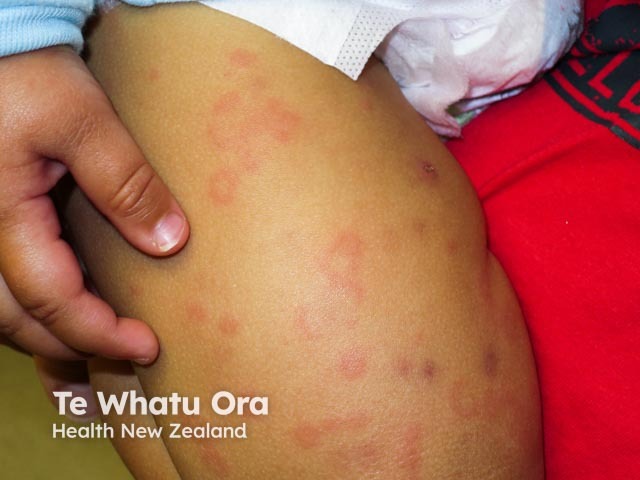
Urticarial vasculitis in skin of colour
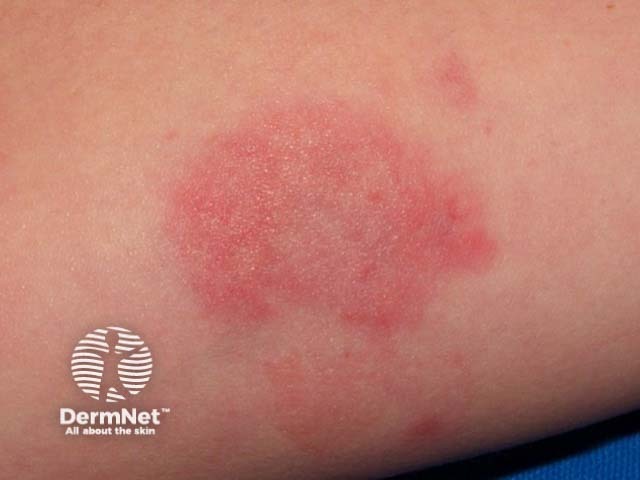
Urticarial vasculitis
Urticarial vasculitis is generally classified as two types:
These are distinguished by finding normal or lowered levels of complement proteins on blood testing. Although both types may be associated with systemic symptoms such as angioedema, abdominal or chest pain, fever, and joint pain, this is more apparent in the hypocomplementaemic form. This form has also been linked to the connective tissue disease systemic lupus erythematosus (SLE).
The cause of urticarial vasculitis is unknown, but it has been associated with the following conditions:
However, the majority of cases of urticarial vasculitis are idiopathic (ie there is no known cause).
The first symptom of urticarial vasculitis is an urticarial eruption (these are characterised by weals) that is often painful or has a burning sensation. In some cases, the weals are itchy. The lesions are red patches or plaques that may have a white centre, and petechiae may appear. Unlike urticaria, urticarial vasculitis lesions usually last for more than 24 hours in a fixed location, after which they will slowly resolve spontaneously. Ecchymoses or hyperpigmentation may occur in the healing process.
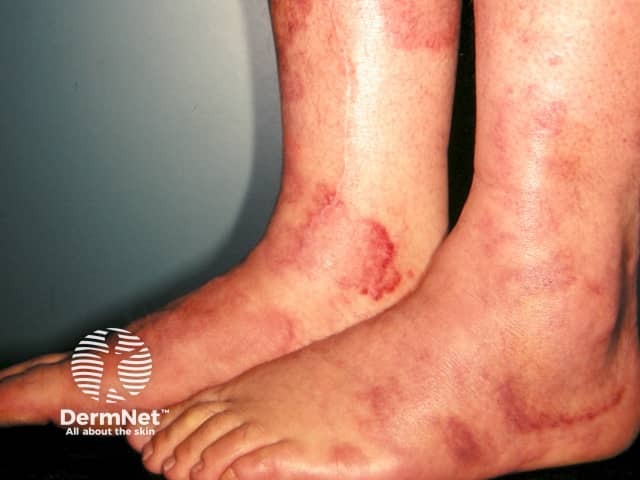
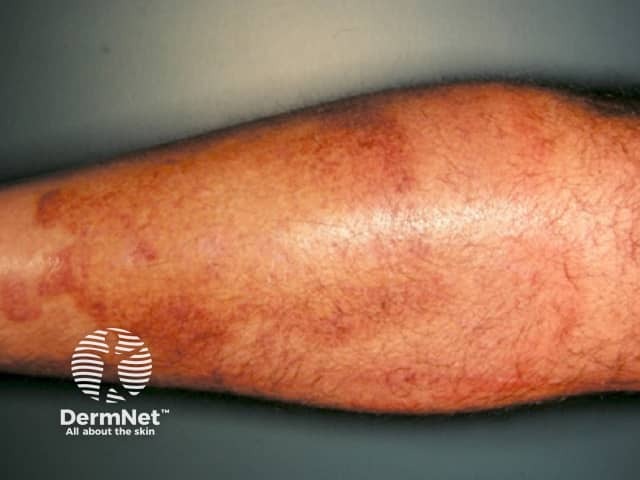
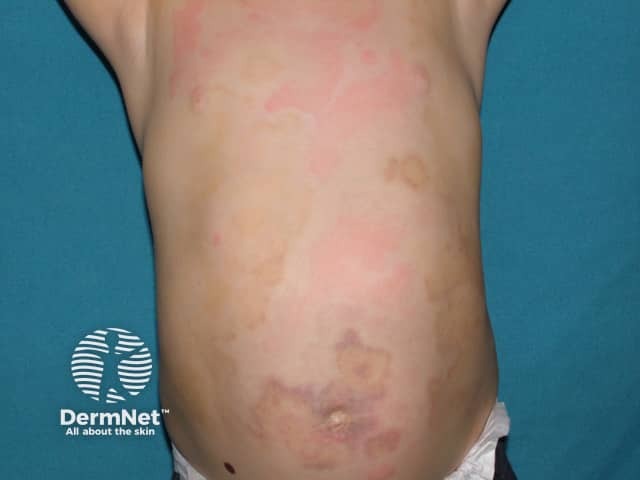
In addition to the skin lesions, patients with urticarial vasculitis may also develop systemic symptoms including photosensitivity, swollen lymph nodes, joint pain (50%), fever, abdominal pain (20%), difficulty breathing, and lung and kidney problems.
See more images of urticarial vasculitis.
A skin biopsy may be performed to confirm urticarial vasculitis. Microscopic findings of early lesions include a neutrophil leukocytoclastic vasculitis, in which there is damage to small vessels in the middle layers of the skin (dermis). In later lesions, a lymphocytic vasculitis may be seen.
Further investigation may find associated diseases. Laboratory studies may include renal function and immunological status. A chest x-ray should be performed in patients with hypocomplementaemia and breathing problems.
Patients with normocomplementaemic urticarial vasculitis usually have minimal or no systemic involvement and lesions often resolve on their own over time.
Treatment is based on the systemic effects of the disease and the extent of cutaneous involvement. Antihistamines or non-steroidal anti-inflammatory drugs (NSAIDs) may be used to relieve symptoms.
Treatments that may be used in the long-term control of severe urticarial vasculitis that may be associated with systemic symptoms include:
For cases of urticarial vasculitis that are resistant to treatment with corticosteroids other immunosuppressive agents such as azathioprine, cyclophosphamide or ciclosporin may be considered.