Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Susan Ford BSc (Hons) Occupational Health, 2012.
Introduction
Occupational risks
Causes
Skin conditions in food handlers
Workplace risk assessment
Personal protective equipment
Hand care advice
Treatment
Occupational hand dermatitis in food handlers and kitchen staff is one of the main causes of ill health in the catering industry. Fifty-five per cent of all skin problems in the industry is caused by contact with water, soaps and detergents, with a further 40% of cases arising from contact with food. The number of new cases of occupational hand dermatitis every year is twice the average of other industries. Food handlers on sick leave take longer to return to work than employees who suffer skin problems in other professions. Similar problems may occur in housewives and other homemakers.
Food handlers may suffer from:

Food handlers

Food handlers

Food handlers
Hand dermatitis in food handlers is caused by four main factors:
Strict hand hygiene is paramount in any food-handling situation. Food Safety Standards require food handlers to wash their hands whenever handling food to avoid contamination of the food with harmful bacteria.
A wet work occupation is one where the skin is wet for more than 2 hours a day in total, or the hands are washed more than 20 times a day.
Soaps and detergents strip the surface of the skin weakening its barrier properties.
Antimicrobial chemicals used in the food industry include detergents and disinfectants used in cleaning the environment and food additives used as preservatives.
Detergents and disinfectants used for cleaning and control of microbial growth fall into different classes. The following chemicals can cause severe irritation or chemical burns to the skin when used in concentrated solutions or with repeated or prolonged exposure.
Chemicals used for food preservation include:
Foods can be chemical or physical irritants. For example, they may be acidic, e.g. citrus fruit, or have sharp fibres, e.g. the skin of kiwifruit. Proteins in food may cause skin reactions in susceptible individuals, leading to allergic contact dermatitis or contact urticaria.
Heat may result in:
Cold may result in:
The outermost layer of the skin (the horny cell layer of the epidermis) acts as a barrier to prevent infection and to prevent potential allergens from penetrating the skin. Its pH is slightly acidic which can help to neutralize the degreasing agents that are in soaps, which are alkaline. Excessive use of soaps and some detergents can destroy the acidity and de-fat the surface skin and therefore reduce the protection it offers.
If the moisture content is too high (overhydrated skin) or too low (dry skin), the skin barrier may also be less effective. Natural moisturising factors are diluted and may be washed out of the skin.
An allergy occurs when an individual's immune system comes to recognise certain harmless foreign particles or pathogens, normally harmless, as harmful. There are several types of food allergy, including:
Irritant contact dermatitis occurs when physical and/or chemical damage to the barrier layer of the skin exceeds the skin’s ability to repair the damage. Examples include:
The features of irritant contact dermatitis are varied.
Allergic contact dermatitis is an immunological response to an allergen. Only people who are allergic to a specific agent (the allergen) will show symptoms. The appearance can be exactly the same as irritant contact dermatitis. However, there are some specific features of allergic contact dermatitis:
Nickel allergy is the most common form of allergic contact dermatitis in food handlers and others.
Other common contact allergens that food handlers are exposed to include:
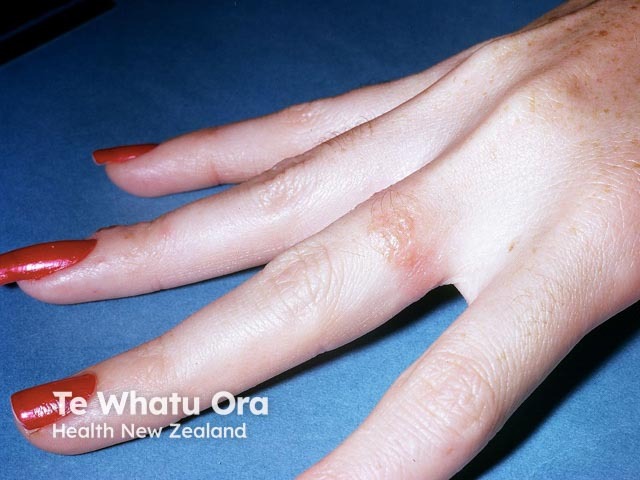
Nickel allergy
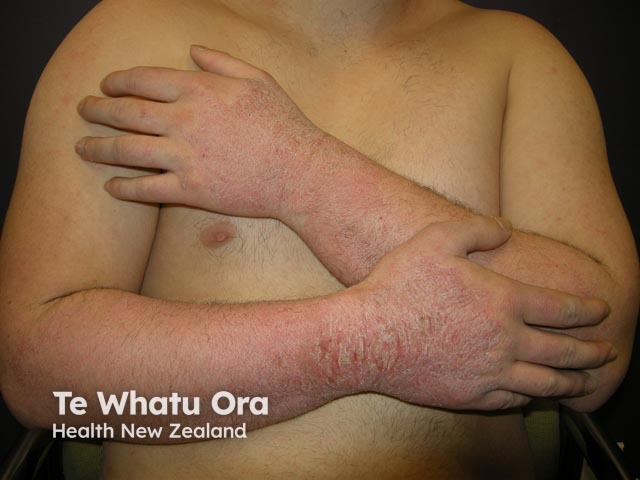
Rubber accelerant allergy
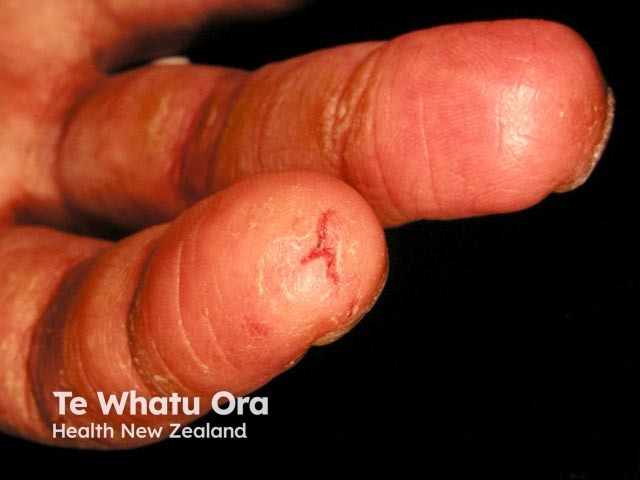
Garlic allergy
Contact urticaria occurs more rapidly than contact dermatitis. Following contact with the causative agent, the skin releases a chemical called histamine, causing itchy wheals (skin swelling) at the site of contact. These fade away within minutes to hours.
Contact urticaria may be non-immunological due to the release of vasoactive substances; immunological, i.e. an allergy response, where IgE antibodies are involved, and where the reaction may be generalised rather than limited to the site of contact; or a reaction of an uncertain mechanism.
Many raw foods can cause contact urticaria, including:
Contact urticaria to latex in rubber gloves is an immunologically mediated contact urticaria.
There are some specific features of contact urticaria.
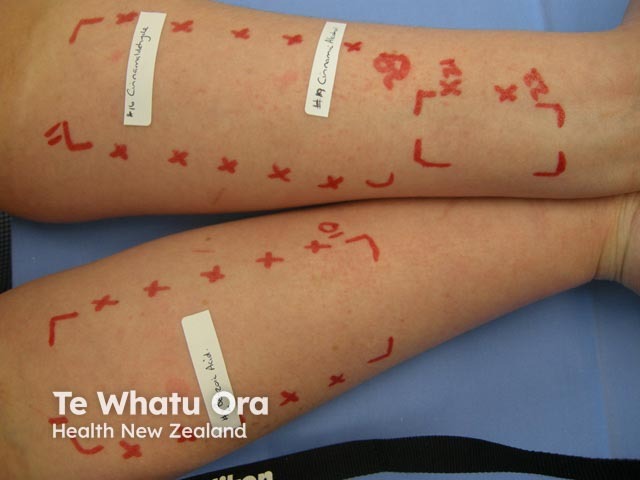
Contact urticaria testing
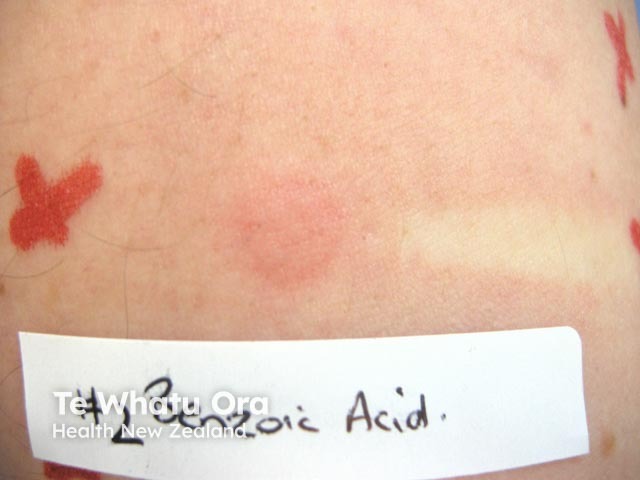
Contact urticaria testing
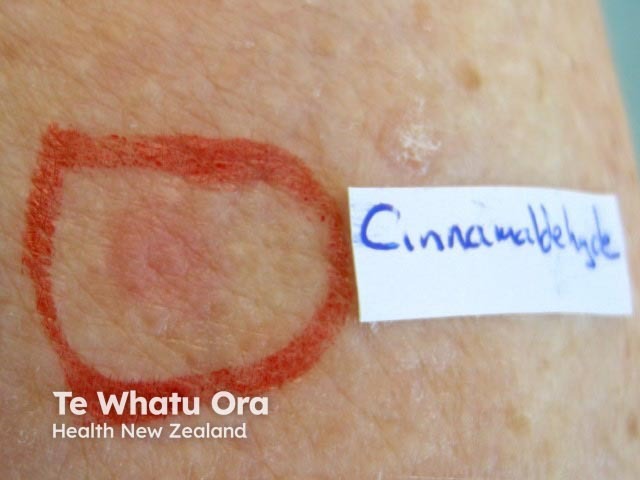
Contact urticaria testing
Protein contact dermatitis is more common in atopic patients. It presents as a combination of early contact urticaria and delayed contact dermatitis, and may follow repetitive contact with meat or fish proteins. It may manifest as hand dermatitis, fingertip dermatitis or chronic paronychia, with or without weals or microvesicles, within an hour of exposure to the causative agent. Protein contact dermatitis is relatively common in fish processing plants, and in abattoirs (where it is usually seen in workers who cut the animals’ throats and in those who handle the gut).
Bacterial infection (impetigo, boils and folliculitis) is usually caused by Staphylococcus aureus and Streptococcus pyogenes.
Food handlers with bacterial skin infections should remain on leave until the infection has resolved, to avoid bacterial contamination of the food
Hand dermatitis and wet work also predispose to yeast infection, usually presenting as chronic paronychia infected by Candida albicans, or as intertrigo between the fingers (also called erosio interdigitalis blastomycetica).
Workers in the meat, poultry and fish processing industries have an increased risk of warts, with human papillomavirus type 7 being responsible for the excess.
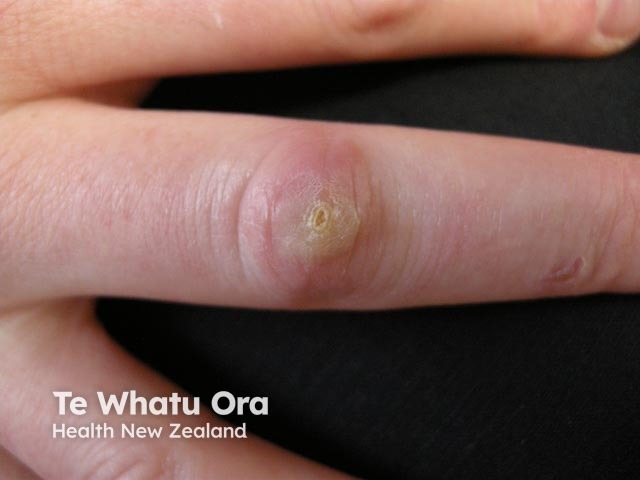
Infected injury
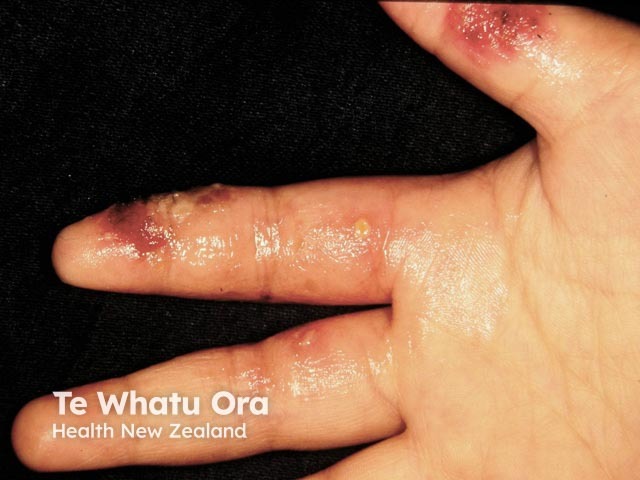
Infected dermatitis
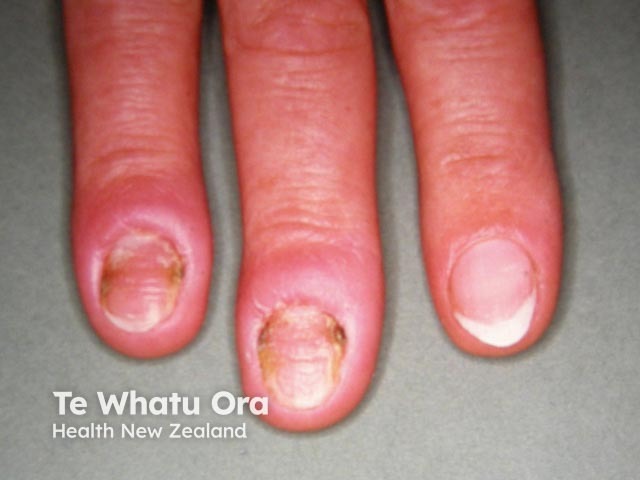
Chronic paronychia
Thermal burns from hot oil or fluids are particularly hazardous for food handlers. Steam from opening oven doors or taking lids from saucepans can cause scalds to hands, forearm or face.
Knife cuts are common in the food industry, usually affecting the non-knife hand and fingers. A chain mail or cut-resistant glove is recommended for the non-knife hand when boning meat.
Workplace risk assessments identify ‘hazards’ (anything that has the potential to cause harm) and ‘risk’ (the likelihood of an event occurring). The aim should be to reduce these, as sickness absence from work can be prolonged and costly. Ill health can adversely affect the quality of life; the ability to work in a chosen industry; insurance costs and litigation claims. A generic risk assessment in any catering establishment and should include a specific section on skin exposure and should cover:
Results of the risk assessments must be recorded and kept.
Health surveillance should be carried out when a workplace hazard is minimised rather than eliminated. Employees should be encouraged to report any signs of skin problems and all reasonable steps should be taken to resolve the problem and prevent recurrences. This may involve a referral for medical advice.
When hazards in the food industry cannot be eliminated, the use of personal protective equipment such as gloves, face masks and overalls must be considered.
When exposure to wet work, chemicals and foods cannot be avoided, the wearing of personal protective equipment such as gloves, face masks and overalls must be considered.
To maximise the benefits and minimise the disadvantages of gloves they should be:
Do Not
Do
If a food handler has developed hand dermatitis, they may be advised to: