Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2003. Update: Dr Thomas Stewart, General Practitioner, Sydney, Australia, November 2017.
Introduction
Causes
Clinical features
Diagnosis
Differential diagnoses
Treatment
Candidal intertrigo refers to superficial skin-fold infection caused by the yeast, candida.
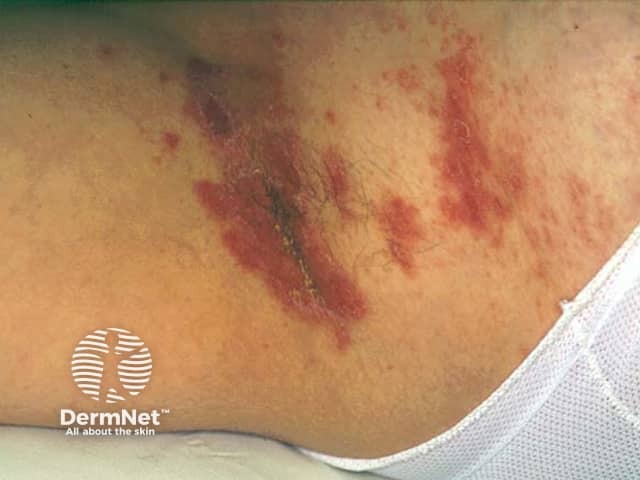
Axillary candidosis
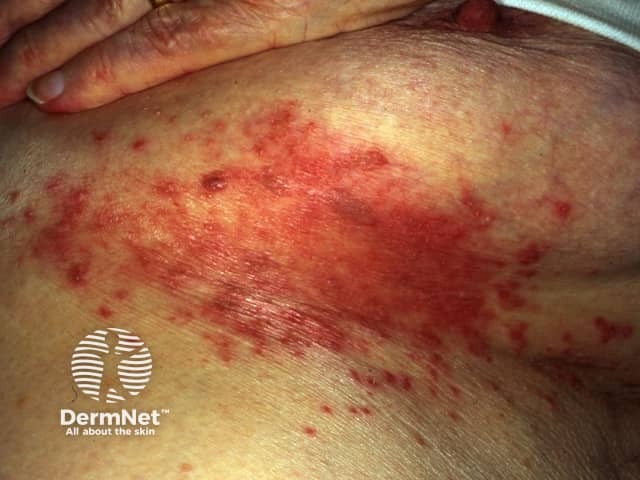
Submammary candidosis
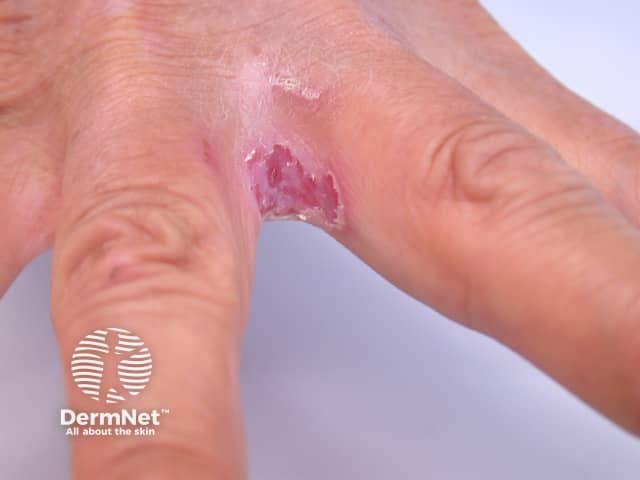
Erosio-interdigitalis blastomycetica
See more images of candida intertrigo.
Candidal intertrigo is triggered by a combination of the following factors:
Who gets candidal intertrigo?
Factors that increase an individual's risk of developing candidal intertrigo include:
Candidal intertrigo classically presents as erythematous and macerated plaques with peripheral scaling. There are often associated superficial satellite papules or pustules.
Affected areas may include:
Diagnosis of candidal intertrigo requires recognition of consistent clinical features. In cases of uncertainty, confirmation can be sought by way of fungal microscopy and culture of skin swabs and scrapings. Skin biopsy is usually not necessary.
Other forms of intertrigo should be considered, including: